Incidence and determinants of extrapulmonary tuberculosis in Egypt: a retrospective cohort study
- PMID: 40254648
- PMCID: PMC12009986
- DOI: 10.1038/s41598-025-95699-z
Incidence and determinants of extrapulmonary tuberculosis in Egypt: a retrospective cohort study
Abstract
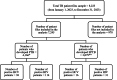
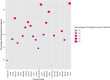
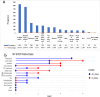
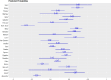
Tuberculosis (TB) is a significant global public health concern. The incidence of extrapulmonary tuberculosis (EPTB) is increasing; however, comprehensive data on its epidemiological and clinical characteristics remain limited, especially among populations who are co-infected with human immunodeficiency virus (HIV) or hepatitis C virus (HCV). This study aimed to assess the incidence and predictors of EPTB in patients co-infected with HIV or HCV in Egypt. We conducted a retrospective cohort study on patients infected with TB who are treated in Egyptian chest hospitals from January 1 to December 31, 2023. Patients were categorized into pulmonary TB (PTB) and EPTB. Clinical data, including HIV or HCV co-infection status, were analyzed to identify risk factors and comorbidities associated with EPTB. Multilevel logistic regression was employed to examine predictors of EPTB. Among 7,245 TB patients, 42.5% were diagnosed with EPTB. Determinant of EPTB were HIV-positive (OR = 0.46, 95% CI: 0.30-0.71, p < 0.001), being male (OR = 0.31, 95% CI: 0.27-0.35, p < 0.001 ), age (particularly children under 5 years) (OR = 4.75, 95% CI: 2.29-9.84, p < 0.001 ), urban residency (OR = 1.05, 95% CI: 0.87-1.27, p < 0.05), and comorbidities (OR = 0.59, 95% CI: 0.35-0.98, p < 0.05). The most common sites for EPTB were the lymph nodes (27.10%) and pleural cavity/effusion (24.60%). EPTB represents a substantial proportion of TB cases in Egypt, particularly among younger individuals and females. Despite the low percentage of HIV or HCV co-infection in EPTB cases, further analysis and diagnostic testing of undiagnosed patients are required. These findings underscore the need for targeted interventions and comprehensive care models for TB patients, especially in the context of HIV co-infection.
Keywords: Co-infection; Extrapulmonary tuberculosis; Hepatitis C; Human immunodeficiency virus; Pulmonary tuberculosis.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests. Ethics approval and consent to participate: The study protocol was reviewed and approved by the Research Ethics Committee of the Egyptian Ministry of Health (MoHP-REC) under Communication/Decision Number 16-2023/17. Informed consent was obtained from all study participants or their legal guardians, permitting the use of their medical information for research purposes. This consent was documented in their medical records as part of the standard procedure before treatment initiation. This study adhered to the ethical principles outlined in the Declaration of Helsinki and relevant national guidelines to ensure the protection and rights of all participants. Consent for publication: Not available.
Figures
References
-
- Bagcchi, S. WHO’s global tuberculosis report 2022. Lancet Microbe4, e20 (2023). - PubMed
-
- World Health Organization (WHO). Global tuberculosis report. (2024).
-
- World Health Organization (WHO). Global tuberculosis report 2021. (2021). https://www.who.int/publications/i/item/9789240037021. Accessed 17 Jun 2024.
-
- World Health Organization (WHO). New report flags major increase in sexually transmitted infections, amidst challenges in HIV and hepatitis. (2024). https://www.who.int/news/item/21-05-2024-new-report-flags-major-increase.... Accessed 16 Jun 2024.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

