Ultrasound-based assessment of impaired gastric emptying in patients with hepatitis B cirrhosis
- PMID: 40254679
- PMCID: PMC12009778
- DOI: 10.1007/s10238-025-01650-x
Ultrasound-based assessment of impaired gastric emptying in patients with hepatitis B cirrhosis
Abstract
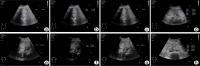
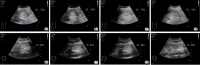
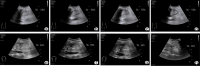
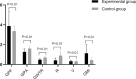
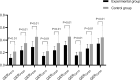
This study aims to evaluate the utility of gastric ultrasound in assessing gastric emptying dysfunction in patients with hepatitis B cirrhosis and its correlation with alterations in portal venous flow and liver stiffness. Gastric motility and emptying parameters, portal venous flow parameters, and liver stiffness were measured by ultrasound in 42 patients with hepatitis B cirrhosis and 48 healthy controls. Statistical analysis was performed to compare the differences in these parameters between the two groups and to analyze the correlation between gastric ultrasound parameters and alternations in portal venous blood flow and liver stiffness. Firstly, the Gastric Motility Index was significantly lower in the experimental group than in the control group, while other gastric ultrasound parameters were significantly higher (p < 0.01). Secondly, measurements obtained from two-dimensional ultrasound, Color Doppler Flow Imaging, and two-dimensional Shear Wave Elastography revealed that Portal Vein Diameter (PVD) and Liver Stiffness (LS) were significantly higher in the experimental group compared to the control group, while the maximum portal vein velocity (PVmax) was significantly lower (p < 0.01). Finally, correlation analysis demonstrated that gastric ultrasound parameters correlated with PVD, PVmax, and LS. Gastric function is significantly impaired in patients with hepatitis B cirrhosis compared to controls, and gastric ultrasound parameters demonstrate a notable correlation with PVD, PVmax, and LS. Gastric ultrasound effectively evaluates gastric motility and emptying function in these patients, offering a reliable foundation for clinical diagnosis and management.
Keywords: Chronic hepatitis B; Gastric dynamics; Gastric emptying; Gastric ultrasound; Hepatic B cirrhosis.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Conflict of interest: The authors have no relevant financial or non-financial interests to disclose. Consent to participate: Informed consent was obtained from all individual participants included in the study. Consent to publish: The authors affirm that human research participants provided informed consent for publication of the images in Figs. 1, 2, 3, 4, 5. Ethics approval: This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of the Affiliated Hospital of North Sichuan Medical College (Date March 29, 2024/No. 2024ER213-1).
Figures


Similar articles
-
Diagnostic value of conventional ultrasound and shear wave elastography in detecting transjugular intrahepatic portosystemic shunt dysfunction.Acta Radiol. 2021 Dec;62(12):1575-1582. doi: 10.1177/0284185120975183. Epub 2020 Nov 28. Acta Radiol. 2021. PMID: 33251812
-
Value of Doppler ultrasound parameters of portal vein and hepatic artery in the diagnosis of cirrhosis and portal hypertension.Am J Gastroenterol. 1997 Jun;92(6):1012-7. Am J Gastroenterol. 1997. PMID: 9177521
-
Predictive value of liver and spleen stiffness measurement based on two-dimensional shear wave elastography for the portal vein pressure in patients with compensatory viral cirrhosis.PeerJ. 2023 Sep 15;11:e15956. doi: 10.7717/peerj.15956. eCollection 2023. PeerJ. 2023. PMID: 37727690 Free PMC article.
-
Non-invasive evaluation of liver cirrhosis using ultrasound.Clin Radiol. 2009 Nov;64(11):1056-66. doi: 10.1016/j.crad.2009.05.010. Epub 2009 Aug 14. Clin Radiol. 2009. PMID: 19822238 Review.
-
Ultrasound or MR elastography of liver: which one shall I use?Abdom Radiol (NY). 2018 Jul;43(7):1546-1551. doi: 10.1007/s00261-017-1340-z. Abdom Radiol (NY). 2018. PMID: 28988274 Free PMC article. Review.
References
-
- Burki T. WHO’s 2024 global hepatitis report. Lancet Infect Dis. 2024;24(6):e362–3. 10.1016/S1473-3099(24)00307-4. - PubMed
-
- Chinese Society of Gastroenterology, Chinese Medical Association. Chinese consensus on the management of liver cirrhosis. J Dig Dis. 2024;25(6):332–52. 10.1111/1751-2980.13294. - PubMed
-
- Kalaitzakis E, Sadik R, Holst JJ, Ohman L, Björnsson E. Gut transit is associated with gastrointestinal symptoms and gut hormone profile in patients with cirrhosis. Clin Gastroenterol Hepatol. 2009;7(3):346–52. 10.1016/j.cgh.2008.11.022. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

