Hybrid Open Anterior and Laparoscopic Repair Using Self-Gripping Mesh for Parastomal Hernia Following Ileal Conduit With Extensive Intra-abdominal Adhesions: A Case Report
- PMID: 40255524
- PMCID: PMC12006874
- DOI: 10.7759/cureus.82500
Hybrid Open Anterior and Laparoscopic Repair Using Self-Gripping Mesh for Parastomal Hernia Following Ileal Conduit With Extensive Intra-abdominal Adhesions: A Case Report
Abstract
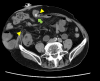
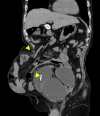
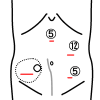
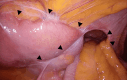
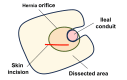
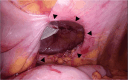
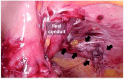
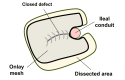
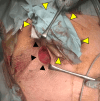
Parastomal hernia (PSH) is the protrusion of visceral organs through an abdominal wall defect adjacent to a stoma and is one of the major complications following cystectomy and ileal conduit (IC) formation. We report a case of hybrid open anterior and laparoscopic repair using self-gripping mesh for a PSH following IC, complicated by extensive intra-abdominal adhesions. An 89-year-old man presented with recurrent episodes of small bowel obstruction (SBO) caused by PSH following IC. The patient had undergone total cystectomy with IC for urinary bladder cancer 30 years prior and had been hospitalized nine times for SBO due to PSH. The patient was referred for surgical treatment. Computed tomography revealed protrusion of the small bowel through a 10 × 7 cm hernia orifice around the IC. Considering the symptomatic PSH with a persistent risk of SBO, laparoscopic repair was planned. Laparoscopic exploration revealed extensive adhesions of the small bowel to the hernia orifice and IC, extending to the pelvis. The IC was also widely attached to the anterior abdominal wall, preventing visual assessment of the contralateral side of the conduit. Therefore, an additional transverse skin incision was made laterally and caudally to the stoma. The defect was closed anteriorly under direct vision with interrupted transfascial sutures and reinforced by onlay mesh placement using a trimmed (15 × 12 cm) self-gripping mesh (ProgripTM, Medtronic). The postoperative course was uneventful. At the 15-month follow-up, the patient was in good physical condition without hernia recurrence or SBO, except for intermittent episodes of urinary obstruction requiring drainage. Hybrid open anterior and laparoscopic repair using self-gripping mesh may be considered a surgical option for PSH following IC with extensive intra-abdominal adhesions around the stoma.
Keywords: ileal conduit; onlay mesh placement; parastomal hernia; self-gripping mesh; small bowel obstruction.
Copyright © 2025, Kitamura et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. Research Ethics Committee for Life Science and Medical Research, Tohoku Medical and Pharmaceutical University issued approval 2024-4-070-0000. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
Similar articles
-
Perioperative and extended outcomes of patients undergoing parastomal hernia repair following cystectomy and ileal conduit.World J Urol. 2024 Aug 12;42(1):482. doi: 10.1007/s00345-024-05123-w. World J Urol. 2024. PMID: 39133311 Free PMC article.
-
Preventing Parastomal Hernia After Ileal Conduit by the Use of a Prophylactic Mesh: A Randomised Study.Eur Urol. 2020 Nov;78(5):757-763. doi: 10.1016/j.eururo.2020.07.033. Epub 2020 Aug 13. Eur Urol. 2020. PMID: 32800407 Clinical Trial.
-
Laparoscopic repair for recurrent parastomal hernia of an end stoma using the sandwich technique while preserving an ileal conduit: A case report.Int J Surg Case Rep. 2016;25:75-8. doi: 10.1016/j.ijscr.2016.06.007. Epub 2016 Jun 16. Int J Surg Case Rep. 2016. PMID: 27337702 Free PMC article.
-
Parastomal hernias after cystectomy and ileal conduit urinary diversion: surgical treatment and the use of prophylactic mesh: a systematic review.BMC Surg. 2022 Mar 29;22(1):118. doi: 10.1186/s12893-022-01509-y. BMC Surg. 2022. PMID: 35351086 Free PMC article.
-
[Median incisional hernias and coexisting parastomal hernias : new surgical strategies and an algorithm for simultaneous repair].Chirurg. 2014 Aug;85(8):697-704. doi: 10.1007/s00104-014-2746-6. Chirurg. 2014. PMID: 24823998 Review. German.
References
-
- Parastomal hernia following cystectomy and ileal conduit urinary diversion: a systematic review. Narang SK, Alam NN, Campain NJ, Pathak S, McGrath JS, Daniels IR, Smart NJ. Hernia. 2017;21:163–175. - PubMed
-
- Long-term outcome of ileal conduit diversion. Madersbacher S, Schmidt J, Eberle JM, Thoeny HC, Burkhard F, Hochreiter W, Studer UE. J Urol. 2003;169:985–990. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
