A Quality Improvement Initiative to Improve Normothermia While Transitioning Premature Infants to an Open Crib
- PMID: 40255666
- PMCID: PMC12007872
- DOI: 10.1097/pq9.0000000000000809
A Quality Improvement Initiative to Improve Normothermia While Transitioning Premature Infants to an Open Crib
Abstract
Introduction: Current literature focuses on the optimal lowest weight and incubator temperature to transition an infant to an open crib, with minimal data quantifying the rate of failed attempts or standardizing the process. Due to multiple failed attempts at this institution in 2021, the project aimed to reduce the rate of preterm newborns who failed the crib by 10% in 1 year.
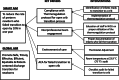
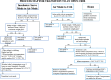
Methods: Interventions, including nursing education, an audit checklist, environmental changes, and a standardized protocol, were implemented after establishing baseline data.
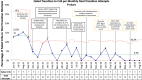
Results: The incidence of failed transitions to an open crib decreased from a baseline of 13.5% failed cribs per monthly transition attempts to 3.3% failed cribs per monthly transition attempts in 18 months, a 76% decrease, where it is currently sustained. Of note, infants born between 32 and 35 weeks gestation had higher failure rates compared with those born <32 weeks.
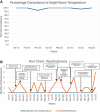
Conclusions: Compliance with a thermoregulation protocol, utilizing an audit checklist, and standardizing the process improved the success rate of transitioning to an open crib.
Copyright © 2025 the Author(s). Published by Wolters Kluwer Health, Inc.
Figures

Similar articles
-
As easy as ABC: evaluation of safe sleep initiative on safe sleep compliance in a freestanding pediatric hospital.Inj Epidemiol. 2019 May 29;6(Suppl 1):26. doi: 10.1186/s40621-019-0205-z. eCollection 2019. Inj Epidemiol. 2019. PMID: 31333992 Free PMC article.
-
Effects of an early transfer from incubator to a warming crib in very low birthweight preterm infants.BMC Pediatr. 2024 May 9;24(1):319. doi: 10.1186/s12887-024-04795-y. BMC Pediatr. 2024. PMID: 38724933 Free PMC article. Clinical Trial.
-
Research from the research utilization project: environmental temperatures.J Obstet Gynecol Neonatal Nurs. 1994 May;23(4):341-4. doi: 10.1111/j.1552-6909.1994.tb01886.x. J Obstet Gynecol Neonatal Nurs. 1994. PMID: 8057188
-
The effect of thermoregulation quality improvement initiatives on the admission temperature of premature/very low birth-weight infants in neonatal intensive care units: A systematic review.J Spec Pediatr Nurs. 2020 Apr;25(2):e12286. doi: 10.1111/jspn.12286. Epub 2020 Jan 7. J Spec Pediatr Nurs. 2020. PMID: 31909894
-
Comparing different scoring systems for predicting mortality risk in preterm infants: a systematic review and network meta-analysis.Front Pediatr. 2023 Dec 15;11:1287774. doi: 10.3389/fped.2023.1287774. eCollection 2023. Front Pediatr. 2023. PMID: 38161435 Free PMC article. Review.
References
-
- Goodstein MH, Stewart DL, Keels EL, et al. ; Committee on Fetus and Newborn, Task Force on Sudden Infant Death Syndrome. Transition to a safe home sleep environment for the NICU patient. Pediatrics (Evanston). 2021;148:e2021052046. 10.1542/peds.2021-052045 - PubMed
-
- Vilinsky A, Sheridan A. Hypothermia in the newborn: an exploration of its cause, effect and prevention. Br J Midwifery. 2014;22:557–562. 10.12968/bjom.2014.22.8.557
-
- Lunze K, Hamer DH. Thermal protection of the newborn in resource-limited environments. J Perinatol. 2012;32:317–324. 10.1038/jp.2012.11 - PubMed
-
- Waldron S, MacKinnon R. Neonatal thermoregulation. Infant. 2007;3:101–104.
-
- Bedwell S, Holtzclaw BJ. Early interventions to achieve thermal balance in term neonates. Nurs Womens Health. 2022;26:389–396. 10.1016/j.nwh.2022.07.006 - PubMed
LinkOut - more resources
Full Text Sources
