Tectal Plate Glioma Presenting With Intratumoral Hemorrhage
- PMID: 40255728
- PMCID: PMC12007068
- DOI: 10.7759/cureus.80813
Tectal Plate Glioma Presenting With Intratumoral Hemorrhage
Abstract
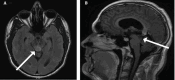
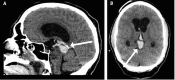
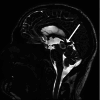
Tectal gliomas are rare brainstem tumors. These tumors typically cause obstructive hydrocephalus due to mass effect on the cerebral aqueduct; however, intratumoral hemorrhage is exceedingly rare, with only one previously documented case to our knowledge. Patients typically present with symptoms of hydrocephalus, including headaches, nausea, and visual disturbances. We report the case of a 43-year-old man with a known tectal plate glioma who presented with acute obstructive hydrocephalus secondary to intratumoral hemorrhage. Following the patient's rapid neurological decline, computed tomography (CT) and magnetic resonance imaging (MRI) confirmed the diagnosis. The patient underwent an endoscopic third ventriculocisternostomy (ETV) for cerebrospinal fluid diversion, along with an endoscopic biopsy of the tectal mass. The patient's postoperative course was favorable, with gradual resolution of symptoms, including diplopia and headaches. A follow-up MRI revealed reduced tumor size and stable ventriculomegaly. Histopathological analysis suggested the tumor to be of glial origin and low-grade in nature, based on its contrast enhancement on MRI and the patient's clinical trajectory. This case illustrates a rare presentation of intratumoral hemorrhage in tectal gliomas, emphasizing the need for heightened clinical suspicion in such cases. ETV remains an effective treatment for obstructive hydrocephalus, though the potential for hemorrhagic complications warrants close monitoring.
Keywords: case report; intracranial hemorrhage; midbrain tumor; midbrain tumor hemorrhage; tectal glioma.
Copyright © 2025, Passman et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures

Similar articles
-
Tectal plate cyst-associated hydrocephalus in an adult: Case report of a rare clinical entity.Radiol Case Rep. 2023 Nov 4;19(1):301-304. doi: 10.1016/j.radcr.2023.10.028. eCollection 2024 Jan. Radiol Case Rep. 2023. PMID: 38028311 Free PMC article.
-
Pediatric midbrain tectal glioneuronal tumor with intratumoral hemorrhage: a case report and literature review.Childs Nerv Syst. 2025 Jun 10;41(1):207. doi: 10.1007/s00381-025-06871-9. Childs Nerv Syst. 2025. PMID: 40490585 Review.
-
Pediatric tectal glioma presented with acute hydrocephalus and ventriculomegaly. Two case reports.Arch Argent Pediatr. 2024 Oct 1;122(5):e202310244. doi: 10.5546/aap.2023-10244.eng. Epub 2024 Feb 15. Arch Argent Pediatr. 2024. PMID: 38320212 English, Spanish.
-
Fatal intratumoral hemorrhage in tectal plate glioblastoma multiforme following ventriculoperitoneal shunt.J Pediatr Neurosci. 2014 May;9(2):192-5. doi: 10.4103/1817-1745.139366. J Pediatr Neurosci. 2014. PMID: 25250086 Free PMC article.
-
Tectal plate gliomas: a review.Childs Nerv Syst. 2013 Oct;29(10):1827-33. doi: 10.1007/s00381-013-2110-z. Epub 2013 Apr 24. Childs Nerv Syst. 2013. PMID: 23612874 Review.
References
-
- Tectal plate glioma: a clinical and radiologic analysis of progression and management in adults. Richardson GE, Clynch AL, Mustafa MA, et al. World Neurosurg. 2024;184:0–73. - PubMed
-
- Tectal plate gliomas: a review. Igboechi C, Vaddiparti A, Sorenson EP, Rozzelle CJ, Tubbs RS, Loukas M. Childs Nerv Syst. 2013;29:1827–1833. - PubMed
-
- Fatal intratumoral hemorrhage in pineal tumors following cerebrospinal fluid diversion. Peng P, Li J, Sun L, Zhou D, Ao X, Chen F. https://e-century.us/files/ijcem/9/10/ijcem0031473.pdf Int J Clin Exp Med. 2016;9:20380–20382.
Publication types
LinkOut - more resources
Full Text Sources
