Impact of Anesthesia on Brain Functional Networks in Moyamoya Disease and Spinal Lesions
- PMID: 40256909
- PMCID: PMC12010199
- DOI: 10.1111/cns.70358
Impact of Anesthesia on Brain Functional Networks in Moyamoya Disease and Spinal Lesions
Abstract
Aims: To analyze the effects of intravenous propofol combined with remifentanil on whole-brain functional networks in patients with ischemic moyamoya disease (IMMD) and intraspinal space-occupying lesions (SOLs) using resting-state functional magnetic resonance imaging (rs-fMRI).
Methods: Ten patients with IMMD and 10 sex- and age-matched patients with lumbar SOL (normal cerebrovascular findings on preoperative MRI) were recruited. General anesthesia was administered using propofol and remifentanil. rs-fMRI imaging was performed in both awake and anesthetized states. Whole-brain functional network in different states was constructed based on graph theory tools.
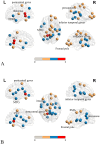
Results: In awake patients with IMMD, significant reductions in nodal strength (NS) were observed in the default mode network (DMN), sensorimotor network, and frontoparietal control network (FPN), compared to patients with SOL. Nodal efficiency (NE) showed further significant network declines. Under anesthesia, patients with IMMD: (1) exhibited disease-specific decreases in NS and NE across several networks, potentially reflecting underlying cerebral pathology. (2) Propofol's effects also contributed to significant NS and NE reductions in several brain regions. Changes before and after anesthesia in patients with IMMD were significantly decreased in specific regions (discussed in detail) per analysis of NS versus NE. DMN connectivity correlated moderately with Montreal Cognitive Assessment scores.
Conclusions: Reduced whole-brain functional connectivity in patients with IMMD before anesthesia was similar to the alterations caused by systemic intravenous drugs administered after anesthesia.
Trial registration: ChiCTR2300075268.
Keywords: brain network; intraspinal space‐occupying lesions; ischemic Moyamoya disease; propofol; resting‐state functional magnetic resonance.
© 2025 The Author(s). CNS Neuroscience & Therapeutics published by John Wiley & Sons Ltd.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures



Similar articles
-
Multi-modal analysis of functional connectivity and cerebral blood flow reveals shared and unique effects of propofol in large-scale brain networks.Neuroimage. 2017 Mar 1;148:130-140. doi: 10.1016/j.neuroimage.2016.12.080. Epub 2017 Jan 6. Neuroimage. 2017. PMID: 28069540 Free PMC article.
-
Mapping altered brain connectivity and its clinical associations in adult moyamoya disease: A resting-state functional MRI study.PLoS One. 2017 Aug 4;12(8):e0182759. doi: 10.1371/journal.pone.0182759. eCollection 2017. PLoS One. 2017. PMID: 28783763 Free PMC article.
-
Changes in Whole Brain Dynamics and Connectivity Patterns during Sevoflurane- and Propofol-induced Unconsciousness Identified by Functional Magnetic Resonance Imaging.Anesthesiology. 2019 Jun;130(6):898-911. doi: 10.1097/ALN.0000000000002704. Anesthesiology. 2019. PMID: 31045899
-
Reorganization of rich-clubs in functional brain networks during propofol-induced unconsciousness and natural sleep.Neuroimage Clin. 2020;25:102188. doi: 10.1016/j.nicl.2020.102188. Epub 2020 Jan 21. Neuroimage Clin. 2020. PMID: 32018124 Free PMC article.
-
Mapping cognitive and emotional networks in neurosurgical patients using resting-state functional magnetic resonance imaging.Neurosurg Focus. 2020 Feb 1;48(2):E9. doi: 10.3171/2019.11.FOCUS19773. Neurosurg Focus. 2020. PMID: 32006946 Free PMC article. Review.
References
MeSH terms
Substances
Grants and funding
- Ministry of Science and Technology of the People's Republic of China grant STI2030-Major Projects+2021ZD0204300
- 82271222/National Natural Science Foundation of China
- Research Project of Peking University Third Hospital in State Key Laboratory of Vascular Homeostasis and Remodeling (Peking University): 2024-VHR-SY-10
LinkOut - more resources
Full Text Sources
Miscellaneous

