Fiberoptic Endoscopic Evaluation of Swallowing (FEES) in Head and Neck Cancer Patients with Late Radiation-Associated Dysphagia: Swallowing Safety, Efficacy, and Dysphagia Phenotype
- PMID: 40277789
- PMCID: PMC12025715
- DOI: 10.3390/curroncol32040233
Fiberoptic Endoscopic Evaluation of Swallowing (FEES) in Head and Neck Cancer Patients with Late Radiation-Associated Dysphagia: Swallowing Safety, Efficacy, and Dysphagia Phenotype
Abstract
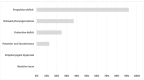
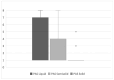
Late radiation-associated dysphagia (late-RAD) remains a challenge in head and neck cancer (HNC) survivorship, despite advancements in treatment methods. Although Fiberoptic Endoscopic Evaluation of Swallowing (FEES) stands as the preferred diagnostic approach for oropharyngeal dysphagia assessment in the HNC population, current studies lack a FEES-derived swallowing parameter characterization and phenotypic classification within this specific cohort. This study sought to employ FEES-based assessment to characterize swallowing safety and efficacy profiles, identify distinct phenotypes in HNC patients suffering from late-RAD, and examine potential correlations between safety and efficacy parameters. A retrospective analysis included twenty-four post-radiotherapy HNC patients evaluated using standardized FEES protocols across three bolus consistencies (liquid, semisolid, and solid). Swallowing safety was quantified using the Penetration-Aspiration Scale (PAS), while efficacy was measured via the Yale Pharyngeal Residue Severity Rating Scale (YPRSRS). Additionally, six distinct dysphagia phenotypes were characterized within the cohort. Propulsion deficit was the predominant phenotype (92%), followed by delayed pharyngeal phase (37.5%) and protective deficit (25%), with 46% of patients exhibiting multiple phenotypes. Unsafe swallowing occurred most frequently with liquid consistency (62.5%), while residue was most prevalent with semisolid (82.6% valleculae, 52.2% pyriform sinuses) and solid consistencies (92.3% valleculae, 53.8% pyriform sinuses). Significant correlations were found between penetration-aspiration and pharyngeal residue scores across consistencies (p < 0.05). FEES examination revealed distinct phenotypes in late radiation-associated dysphagia, with a predominance of propulsion deficit and significant interdependence between safety and efficacy parameters.
Keywords: dysphagia phenotypes; fiberoptic endoscopic evaluation of swallowing; head and neck cancer; radiation-associated dysphagia; swallowing efficacy; swallowing safety.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


Similar articles
-
Fiberoptic endoscopic evaluation of swallowing (FEES) in children with spinal muscular atrophy type 1: feasibility, swallowing safety and efficacy, and dysphagia phenotype.Eur Arch Otorhinolaryngol. 2024 Dec;281(12):6523-6532. doi: 10.1007/s00405-024-08922-4. Epub 2024 Sep 4. Eur Arch Otorhinolaryngol. 2024. PMID: 39230607 Free PMC article.
-
Association Between Pharyngeal Pooling and Aspiration Using Fiberoptic Endoscopic Evaluation of Swallowing in Head and Neck Cancer Patients with Dysphagia.Dysphagia. 2020 Feb;35(1):42-51. doi: 10.1007/s00455-019-09992-x. Epub 2019 Mar 13. Dysphagia. 2020. PMID: 30868301 Free PMC article.
-
Correlation Between Pharyngeal Residue and Aspiration in Fiber-Optic Endoscopic Evaluation of Swallowing: An Observational Study.Arch Phys Med Rehabil. 2019 Mar;100(3):488-494. doi: 10.1016/j.apmr.2018.05.028. Epub 2018 Jun 27. Arch Phys Med Rehabil. 2019. PMID: 29959934
-
Pneumonia, Mortality, and Other Outcomes Associated with Unsafe Swallowing Detected via Fiberoptic Endoscopic Evaluation of Swallowing (FEES) in Patients with Functional Oropharyngeal Dysphagia: A Systematic Review and Meta-analysis.Dysphagia. 2022 Dec;37(6):1662-1672. doi: 10.1007/s00455-022-10427-3. Epub 2022 Feb 28. Dysphagia. 2022. PMID: 35226186
-
Fiberoptic Endoscopic Evaluation of Swallowing in Infants and Children: Protocol, Safety, and Clinical Efficacy: 25 Years of Experience.Ann Otol Rhinol Laryngol. 2020 May;129(5):469-481. doi: 10.1177/0003489419893720. Epub 2019 Dec 17. Ann Otol Rhinol Laryngol. 2020. PMID: 31845586 Review.
References
-
- Schindler A., Denaro N., Russi E.G., Pizzorni N., Bossi P., Merlotti A., Spadola Bissetti M., Numico G., Gava A., Orlandi E., et al. Dysphagia in Head and Neck Cancer Patients Treated with Radiotherapy and Systemic Therapies: Literature Review and Consensus. Crit. Rev. Oncol. Hematol. 2015;96:372–384. doi: 10.1016/j.critrevonc.2015.06.005. - DOI - PubMed
-
- Baijens L.W.J., Walshe M., Aaltonen L.-M., Arens C., Cordier R., Cras P., Crevier-Buchman L., Curtis C., Golusinski W., Govender R., et al. European White Paper: Oropharyngeal Dysphagia in Head and Neck Cancer. Eur. Arch. Otorhinolaryngol. 2021;278:577–616. doi: 10.1007/s00405-020-06507-5. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

