Incidence and Prognostic Significance of Hormonal Receptors and HER2 Status Conversion in Recurrent Breast Cancer: A Retrospective Study in a Single Institute
- PMID: 40282854
- PMCID: PMC12028628
- DOI: 10.3390/medicina61040563
Incidence and Prognostic Significance of Hormonal Receptors and HER2 Status Conversion in Recurrent Breast Cancer: A Retrospective Study in a Single Institute
Abstract
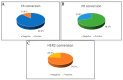
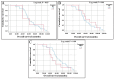
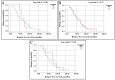
Background and Objectives: Changes in biomarker status are not rare and usually occur in an unfavorable direction. Evaluating changes in biomarker status is advantageous for assessing treatment options and prognosticating patients. Currently, only a few studies have explored the association between biomarker conversion and breast cancer relapse. In this study, we sought to determine the incidence of receptor conversions in patients diagnosed with recurrent breast cancer in comparison to their corresponding primary tumors and to evaluate possible influencing factors. Moreover, we aimed to assess the prognostic significance of biomarker conversion, if any was detected, in breast cancer patients. Materials and Methods: A retrospective cohort study was conducted among breast cancer patients treated at King Khalid University Hospital, Riyadh, Saudi Arabia. Data were collected from recurrent breast cancer patients about different parameters to assess the incidence of hormonal receptors and human epidermal growth factor 2 (HER2) status conversion between primary and recurrent tumors. The calculation of progression-free survival (PFS)/ relapse-free survival (RFS) and the overall survival (OS) was conducted to assess the prognostic value of the assessed biomarker conversion. Results: Progesterone receptor (PR) conversion had the highest incidence (29.9%), followed by HER2 (23%) and estrogen receptor (ER) (12.6%). Menopausal status and concurrent receptor conversion were significant factors influencing receptor status changes. However, no significant associations were found between receptor conversion and other clinical factors, including tumor stage and histological subtype. The survival analysis revealed no statistically significant differences in OS or RFS between patients with and without receptor conversion. Conclusions: Receptor conversion, particularly for PR and HER2, is common in recurrent breast cancer, emphasizing the importance of re-biopsy at recurrence to ensure accurate treatment decisions. While receptor conversion does not significantly impact survival outcomes in this cohort, further large-scale prospective studies are warranted to validate these findings and explore their clinical implications in breast cancer management.
Keywords: HER2 status; breast cancer; estrogen receptor; progesterone receptor; prognostic significance; receptor conversion; survival analysis.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
Similar articles
-
Prognostic significance of estrogen, progesterone and HER2 receptors' status conversion following neoadjuvant chemotherapy in patients with locally advanced breast cancer: Results from a tertiary Cancer Center in Saudi Arabia.PLoS One. 2021 Mar 5;16(3):e0247802. doi: 10.1371/journal.pone.0247802. eCollection 2021. PLoS One. 2021. PMID: 33667252 Free PMC article.
-
Receptor discordance rate and its effects on survival in primary and recurrent breast cancer patients.J BUON. 2016 Nov-Dec;21(6):1425-1432. J BUON. 2016. PMID: 28039703
-
Prospective comparison of switches in biomarker status between primary and recurrent breast cancer: the Breast Recurrence In Tissues Study (BRITS).Breast Cancer Res. 2010;12(6):R92. doi: 10.1186/bcr2771. Epub 2010 Nov 8. Breast Cancer Res. 2010. PMID: 21059212 Free PMC article.
-
Factors predictive of response to hormone therapy in breast cancer.Tumori. 2008 May-Jun;94(3):370-83. doi: 10.1177/030089160809400314. Tumori. 2008. PMID: 18705406 Review.
-
A Systematic Literature Review of the Prognostic and Predictive Value of PIK3CA Mutations in HR+/HER2- Metastatic Breast Cancer.Clin Breast Cancer. 2020 Jun;20(3):e232-e243. doi: 10.1016/j.clbc.2019.08.011. Epub 2019 Sep 10. Clin Breast Cancer. 2020. PMID: 32234362
References
-
- Vemuru S., Huang J., Colborn K., Yoon Y., Huynh V., Leonard L., Ahrendt G., Christian N., Afghahi A., McLemore L., et al. Clinical implications of receptor conversions in breast cancer patients who have undergone neoadjuvant chemotherapy. Breast Cancer Res. Treat. 2023;200:247–256. doi: 10.1007/s10549-023-06978-0. - DOI - PMC - PubMed
-
- Li C., Fan H., Xiang Q., Xu L., Zhang Z., Liu Q., Zhang T., Ling J., Zhou Y., Zhao X., et al. Prognostic value of receptor status conversion following neoadjuvant chemotherapy in breast cancer patients: A systematic review and meta-analysis. Breast Cancer Res. Treat. 2019;178:497–504. doi: 10.1007/s10549-019-05421-7. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

