Pathophysiology, Clinical Heterogeneity, and Therapeutic Advances in Amyotrophic Lateral Sclerosis: A Comprehensive Review of Molecular Mechanisms, Diagnostic Challenges, and Multidisciplinary Management Strategies
- PMID: 40283201
- PMCID: PMC12029092
- DOI: 10.3390/life15040647
Pathophysiology, Clinical Heterogeneity, and Therapeutic Advances in Amyotrophic Lateral Sclerosis: A Comprehensive Review of Molecular Mechanisms, Diagnostic Challenges, and Multidisciplinary Management Strategies
Abstract
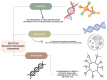
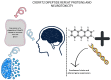
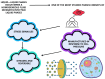
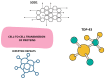
Amyotrophic lateral sclerosis (ALS) is a progressive neurodegenerative disorder characterized by the progressive degeneration of upper and lower motor neurons, leading to muscle atrophy, paralysis, and respiratory failure. This comprehensive review synthesizes the current knowledge on ALS pathophysiology, clinical heterogeneity, diagnostic frameworks, and evolving therapeutic strategies. Mechanistically, ALS arises from complex interactions between genetic mutations (e.g., in C9orf72, SOD1, TARDBP (TDP-43), and FUS) and dysregulated cellular pathways, including impaired RNA metabolism, protein misfolding, nucleocytoplasmic transport defects, and prion-like propagation of toxic aggregates. Phenotypic heterogeneity, manifesting as bulbar-, spinal-, or respiratory-onset variants, complicates its early diagnosis, which thus necessitates the rigorous application of the revised El Escorial criteria and emerging biomarkers such as neurofilament light chain. Clinically, ALS intersects with frontotemporal dementia (FTD) in up to 50% of the cases, driven by shared TDP-43 pathology and C9orf72 hexanucleotide expansions. Epidemiological studies have revealed a lifetime risk of 1:350, with male predominance (1.5:1) and peak onset between 50 and 70 years. Disease progression varies widely, with a median survival of 2-4 years post-diagnosis, underscoring the urgency for early intervention. Approved therapies, including riluzole (glutamate modulation), edaravone (antioxidant), and tofersen (antisense oligonucleotide), offer modest survival benefits, while dextromethorphan/quinidine alleviates the pseudobulbar affect. Non-pharmacological treatment advances, such as non-invasive ventilation (NIV), prolong survival by 13 months and improve quality of life, particularly in bulb-involved patients. Multidisciplinary care-integrating physical therapy, respiratory support, nutritional management, and cognitive assessments-is critical to addressing motor and non-motor symptoms (e.g., dysphagia, spasticity, sleep disturbances). Emerging therapies show promise in preclinical models. However, challenges persist in translating genetic insights into universally effective treatments. Ethical considerations, including euthanasia and end-of-life decision-making, further highlight the need for patient-centered communication and palliative strategies.
Keywords: C9orf72 expansion; SOD1 mutations; TDP-43 proteinopathy; amyotrophic lateral sclerosis; frontotemporal dementia; multidisciplinary care; neurodegenerative disease; neurofilament light chain; non-invasive ventilation; riluzole.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- Van Damme P., Al-Chalabi A., Andersen P.M., Chio A., Couratier P., De Carvalho M., Hardiman O., Kuzma-Kozakiewicz M., Ludolph A., McDermott C.J., et al. European Academy of Neurology (EAN) guideline on the management of amyotrophic lateral sclerosis in collaboration with European Reference Network for Neuromuscular Diseases (ERN EURO-NMD) Eur. J. Neurol. 2024;31:e16264. doi: 10.1111/ene.16264. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

