Establishment and analysis of the prediction model for the prognosis of children with sepsis based on pSOFA score
- PMID: 40290256
- PMCID: PMC12022587
- DOI: 10.12669/pjms.41.4.10001
Establishment and analysis of the prediction model for the prognosis of children with sepsis based on pSOFA score
Abstract
Objective: To investigate the prognostic risk factors of sepsis in children diagnosed based on the pediatric sequential organ failure assessment (pSOFA) scoring system, and to establish and evaluate related prediction model.
Methods: This was a retrospective study. Two hundred and seventy three children with sepsis admitted to Hebei Children's Hospital from January 1, 2019 to December 31, 2022 were divided into survival group and mortality group according to the prognosis. Multivariate Logisitic regression was used to analyze the independent risk factors affecting the prognosis of septic children, and a predictive model was established to analyze the predictive value of the model on the prognosis of septic children.
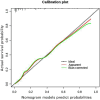
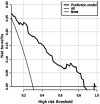
Results: The results of multivariate logistic regression analysis showed that systemic vascular resistance index (SVRI) <1143, febrile neutropenia (FN) and pSOFA score were independent risk factors for sepsis-related death in children. This equation of 5.140+2.069 × (SVRI<1143) + 1.718 × FN+0.290 × pSOFA score indicates that, the area under the ROC curve of the prediction model is greater than that of SVRI<1143, FN, and pSOFA score alone, and the sensitivity and specificity of the model were 81.5% and 84.5%, respectively.
Conclusion: The prediction model has a good clinical predictive value and has practical significance for the prognosis evaluation and treatment guidance.
Keywords: Febrile neutropenia; Pediatric sequential organ failure assessment (pSOFA); Sepsis; Systemic vascular resistance index (SVRI).
Copyright: © Pakistan Journal of Medical Sciences.
Conflict of interest statement
Conflicts of interest: None.
Figures
References
-
- Guo Y, Yang H, Gao W, Ma CE, Li T. Combination of Biomarkers in Predicting 28-Day Mortality for Septic Patients. J Coll Physicians Surg Pak. 2018;28(9):672–676. doi:10.29271/jcpsp.2018.09.672. - PubMed
-
- Goldstein B, Giroir B, Randolph A International Consensus Conference on Pediatric Sepsis. International pediatric sepsis consensus conference:definitions for sepsis and organ dysfunction in pediatrics. Pediatr Crit Care Med. 2005;6(1):2–8. doi:10.1097/01. PCC.0000149131.72248. E6. - PubMed
-
- Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, Opal SM, et al. Surviving sepsis campaign:international guidelines for management of severe sepsis and septic shock:2012. Crit Care Med. 2013;41(2):580–637. doi:10.1097/CCM.0b013e31827e83af. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous