Paraneoplastic Syndromes Mimicking Dermatomyositis and Remitting Seronegative Symmetrical Synovitis With Pitting Edema (RS3PE) Syndrome in Cancer of Unknown Primary Origin: A Case Report
- PMID: 40291331
- PMCID: PMC12034368
- DOI: 10.7759/cureus.81376
Paraneoplastic Syndromes Mimicking Dermatomyositis and Remitting Seronegative Symmetrical Synovitis With Pitting Edema (RS3PE) Syndrome in Cancer of Unknown Primary Origin: A Case Report
Abstract
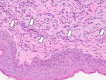
A 70-year-old male patient presented with fever, polyarthritis, systemic muscle weakness and pain, and skin rash, initially suspected to be an autoimmune disorder. Imaging revealed right supraclavicular and paratracheal lymphadenopathy, and a right supraclavicular lymph node biopsy confirmed squamous cell carcinoma. Still, the primary site remained unidentified, leading to a diagnosis of cancer of unknown primary origin (CUP). Laboratory tests showed no positive autoantibodies such as anti-Jo-1, anti-ribonucleoprotein (RNP), anti-Smith (Sm), and anti-SS-A antibodies, and a skin biopsy of the back indicated panniculitis with neutrophilic infiltration. Given the absence of infectious or autoimmune causes, the symptoms were attributed to paraneoplastic syndrome (PNS) associated with CUP, mimicking dermatomyositis and remitting seronegative symmetrical synovitis with pitting edema (RS3PE) syndrome. Treatment with prednisolone (15 mg/day) led to the rapid resolution of joint pain, rash, and fever. Chemotherapy with carboplatin and paclitaxel for CUP was initiated with minimal adverse effects, allowing for continued outpatient management. This case highlights the importance of considering PNS when collagen disease-like symptoms are present in malignancy, particularly in CUP. Early recognition and corticosteroid therapy can improve performance status, enabling timely cancer treatment. Identifying atypical PNS presentations in CUP remains challenging, but a multidisciplinary approach can aid in diagnosis and management.
Keywords: arthritis; carcinoma; dermatomyositis; neoplasms; paraneoplastic syndromes; remitting seronegative symmetrical synovitis with pitting edema syndrome; rheumatoid; squamous cell; steroids; unknown primary.
Copyright © 2025, Mochizuki et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
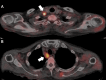
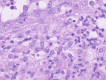
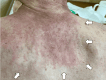
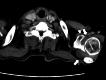
Similar articles
-
Remitting seronegative symmetrical synovitis with pitting edema syndrome with two different underlying malignancies: A case report.Medicine (Baltimore). 2025 Apr 4;104(14):e42091. doi: 10.1097/MD.0000000000042091. Medicine (Baltimore). 2025. PMID: 40193665 Free PMC article.
-
Idiopathic remitting seronegative symmetrical synovitis with pitting edema syndrome mimicking symptoms of polymyalgia rheumatica: a case report.J Med Case Rep. 2022 Aug 27;16(1):334. doi: 10.1186/s13256-022-03535-z. J Med Case Rep. 2022. PMID: 36028914 Free PMC article. Review.
-
Remitting seronegative symmetrical synovitis with pitting edema syndrome complicated with primary lung cancer.Int Cancer Conf J. 2016 Sep 26;6(1):16-21. doi: 10.1007/s13691-016-0264-8. eCollection 2017 Jan. Int Cancer Conf J. 2016. PMID: 31149462 Free PMC article.
-
Synchronous Occurrence of Bazex Syndrome and Remitting Seronegative Symmetrical Synovitis with Pitting Edema Syndrome in a Patient with Lung Cancer.Intern Med. 2019 Nov 15;58(22):3267-3271. doi: 10.2169/internalmedicine.3032-19. Epub 2019 Jul 10. Intern Med. 2019. PMID: 31292397 Free PMC article.
-
The occurrence of remitting seronegative symmetrical synovitis with pitting edema (RS3PE) after arthroplasty mimicking a periprosthetic joint infection: A case report and literature review.Medicine (Baltimore). 2024 Nov 1;103(44):e40344. doi: 10.1097/MD.0000000000040344. Medicine (Baltimore). 2024. PMID: 39495994 Free PMC article. Review.
References
-
- Frequency of specific cancer types in dermatomyositis and polymyositis: a population-based study. Hill CL, Zhang Y, Sigurgeirsson B, et al. Lancet. 2001;357:96–100. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
