Uncovering Social States in Healthy and Clinical Populations Using Digital Phenotyping and Hidden Markov Models: Observational Study
- PMID: 40294408
- PMCID: PMC12070022
- DOI: 10.2196/64007
Uncovering Social States in Healthy and Clinical Populations Using Digital Phenotyping and Hidden Markov Models: Observational Study
Abstract
Background: Brain-related disorders are characterized by observable behavioral symptoms, for example, social withdrawal. Smartphones can passively collect behavioral data reflecting digital activities such as communication app usage and calls. These data are collected objectively in real time, avoiding recall bias, and may, therefore, be a useful tool for measuring behaviors related to social functioning. Despite promising clinical utility, analyzing smartphone data is challenging as datasets often include a range of temporal features prone to missingness.
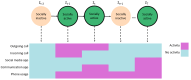
Objective: Hidden Markov models (HMMs) provide interpretable, lower-dimensional temporal representations of data, allowing for missingness. This study aimed to investigate the HMM as a method for modeling smartphone time series data.
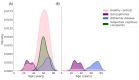
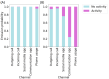
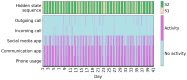
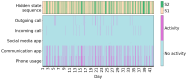
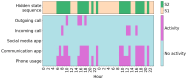
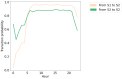
Methods: We applied an HMM to an aggregate dataset of smartphone measures designed to assess phone-related social functioning in healthy controls (HCs) and participants with schizophrenia, Alzheimer disease (AD), and memory complaints. We trained the HMM on a subset of HCs (91/348, 26.1%) and selected a model with socially active and inactive states. Then, we generated hidden state sequences per participant and calculated their "total dwell time," that is, the percentage of time spent in the socially active state. Linear regression models were used to compare the total dwell time to social and clinical measures in a subset of participants with available measures, and logistic regression was used to compare total dwell times between diagnostic groups and HCs. We primarily reported results from a 2-state HMM but also verified results in HMMs with more hidden states and trained on the whole participant dataset.
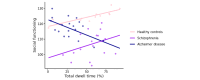
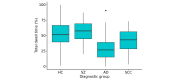
Results: We identified lower total dwell times in participants with AD (26/257, 10.1%) versus withheld HCs (156/257, 60.7%; odds ratio 0.95, 95% CI 0.92-0.97; false discovery rate [FDR]-corrected P<.001), as well as in participants with memory complaints (57/257, 22.2%; odds ratio 0.97, 95% CI 0.96-0.99; FDR-corrected P=.004). The result in the AD group was very robust across HMM variations, whereas the result in the memory complaints group was less robust. We also observed an interaction between the AD group and total dwell time when predicting social functioning (FDR-corrected P=.02). No significant relationships regarding total dwell time were identified for participants with schizophrenia (18/257, 7%; P>.99).
Conclusions: We found the HMM to be a practical, interpretable method for digital phenotyping analysis, providing an objective phenotype that is a possible indicator of social functioning.
Keywords: Alzheimer disease; cognitive impairment; digital phenotyping; hidden Markov model; mHealth; mobile health; mobile phone; passive monitoring; schizophrenia; smartphone; social behavior.
©Imogen E Leaning, Andrea Costanzo, Raj Jagesar, Lianne M Reus, Pieter Jelle Visser, Martien J H Kas, Christian F Beckmann, Henricus G Ruhé, Andre F Marquand. Originally published in the Journal of Medical Internet Research (https://www.jmir.org), 28.04.2025.
Conflict of interest statement
Conflicts of Interest: CFB is the director of SBGNeuro. HGR received grants from the Hersenstichting, ZonMw, the Dutch Ministry of Health, and an unrestricted educational grant from Janssen. In addition, he received speaking fees from Lundbeck, Janssen, Benecke, and Prelum, all outside the current work. All other authors declare no conflicts of interest.
Figures

Similar articles
-
Measuring Environmental and Behavioral Drivers of Chronic Diseases Using Smartphone-Based Digital Phenotyping: Intensive Longitudinal Observational mHealth Substudy Embedded in 2 Prospective Cohorts of Adults.JMIR Public Health Surveill. 2024 Oct 11;10:e55170. doi: 10.2196/55170. JMIR Public Health Surveill. 2024. PMID: 39392682 Free PMC article.
-
Mobility-Based Smartphone Digital Phenotypes for Unobtrusively Capturing Everyday Cognition, Mood, and Community Life-Space in Older Adults: Feasibility, Acceptability, and Preliminary Validity Study.JMIR Hum Factors. 2024 Nov 22;11:e59974. doi: 10.2196/59974. JMIR Hum Factors. 2024. PMID: 39576984 Free PMC article.
-
Digital phenotyping of social functioning and employment in people with schizophrenia: Pilot data from an international sample.Psychiatry Clin Neurosci. 2025 Mar;79(3):125-130. doi: 10.1111/pcn.13786. Epub 2025 Jan 22. Psychiatry Clin Neurosci. 2025. PMID: 39840820
-
Working definitions, subjective and objective assessments and experimental paradigms in a study exploring social withdrawal in schizophrenia and Alzheimer's disease.Neurosci Biobehav Rev. 2019 Feb;97:38-46. doi: 10.1016/j.neubiorev.2018.06.020. Epub 2018 Jun 24. Neurosci Biobehav Rev. 2019. PMID: 29949732 Review.
-
Digital Phenotyping in Adults with Schizophrenia: A Narrative Review.Curr Psychiatry Rep. 2023 Nov;25(11):699-706. doi: 10.1007/s11920-023-01467-z. Epub 2023 Oct 20. Curr Psychiatry Rep. 2023. PMID: 37861979 Review.
References
-
- van der Wee NJ, Bilderbeck A, Cabello M, Ayuso-Mateos JL, Saris IM, Giltay EJ, Penninx BW, Arango C, Post A, Porcelli S. Working definitions, subjective and objective assessments and experimental paradigms in a study exploring social withdrawal in schizophrenia and Alzheimer's disease. Neurosci Biobehav Rev. 2019 Feb;97:38–46. doi: 10.1016/j.neubiorev.2018.06.020. https://linkinghub.elsevier.com/retrieve/pii/S0149-7634(17)30758-3 S0149-7634(17)30758-3 - DOI - PubMed
-
- Porcelli S, van der Wee N, van der Werff S, Aghajani M, Glennon JC, van Heukelum S, Mogavero F, Lobo A, Olivera FJ, Lobo E, Posadas M, Dukart J, Kozak R, Arce E, Ikram A, Vorstman J, Bilderbeck A, Saris I, Kas MJ, Serretti A. Social brain, social dysfunction and social withdrawal. Neurosci Biobehav Rev. 2019 Feb;97:10–33. doi: 10.1016/j.neubiorev.2018.09.012. https://linkinghub.elsevier.com/retrieve/pii/S0149-7634(18)30195-7 S0149-7634(18)30195-7 - DOI - PubMed
-
- Saris IM, Aghajani M, van der Werff SJ, van der Wee NJ, Penninx BW. Social functioning in patients with depressive and anxiety disorders. Acta Psychiatr Scand. 2017 Oct;136(4):352–61. doi: 10.1111/acps.12774. https://europepmc.org/abstract/MED/28767127 - DOI - PMC - PubMed
-
- Jagesar RR, Vorstman JA, Kas MJ. Requirements and operational guidelines for secure and sustainable digital phenotyping: design and development study. J Med Internet Res. 2021 Apr 07;23(4):e20996. doi: 10.2196/20996. https://www.jmir.org/2021/4/e20996/ v23i4e20996 - DOI - PMC - PubMed
-
- Bai R, Xiao L, Guo Y, Zhu X, Li N, Wang Y, Chen Q, Feng L, Wang Y, Yu X, Xie H, Wang G. Tracking and monitoring mood stability of patients with major depressive disorder by machine learning models using passive digital data: prospective naturalistic multicenter study. JMIR Mhealth Uhealth. 2021 Mar 08;9(3):e24365. doi: 10.2196/24365. https://mhealth.jmir.org/2021/3/e24365/ v9i3e24365 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

