Impact of age on degenerative joint disease of the temporomandibular joint: A systematic review and meta-analysis
- PMID: 40295246
- PMCID: PMC12040012
- DOI: 10.1097/MD.0000000000041915
Impact of age on degenerative joint disease of the temporomandibular joint: A systematic review and meta-analysis
Abstract
Background: It is unclear that the influence of age on degenerative joint disease (DJD) of the temporomandibular joint (TMJ).
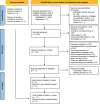
Methods: Relevant literature was retrieved from PubMed, Elsevier, Web of Science, and Google Scholar. EndNote 21 was used to consolidate the literature retrieved from these databases. Key information were extracted from the included studies, statistical analysis was performed using Stata 15.0. The quality of the studies was evaluated using the cross-sectional study evaluation criteria recommended by the Agency for Healthcare Research and Quality.
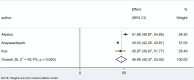
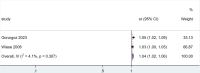
Results: A total of 11 studies involving 2832 participants (1099 males, 1744 females) were included. The incidence of DJD of the TMJ was approximately 35% among individuals aged 20 to 39, 43% among those aged 40 to 59, and 54% among those aged 60-69.
Conclusion: Age progression is a key risk factor for the development of DJD of the TMJ. The incidence of DJD of the TMJ increases progressively across different age groups, with a significant rise observed in middle to older age groups.
Keywords: age; degenerative joint disease of the temporomandibular joint; influencing factors; meta-analysis; temporomandibular joint.
Copyright © 2025 the Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures

Similar articles
-
Prevalence of degenerative disease in temporomandibular disorder patients with disc displacement: A systematic review and meta-analysis.J Craniomaxillofac Surg. 2020 Oct;48(10):942-955. doi: 10.1016/j.jcms.2020.08.004. Epub 2020 Aug 25. J Craniomaxillofac Surg. 2020. PMID: 32896478
-
Prevalence of degenerative joint disease of the temporomandibular joint: a systematic review.Clin Oral Investig. 2019 May;23(5):2475-2488. doi: 10.1007/s00784-018-2664-y. Epub 2018 Oct 11. Clin Oral Investig. 2019. PMID: 30311063
-
Functional, physical and psychosocial impact of degenerative temporomandibular joint disease.J Oral Rehabil. 2022 Mar;49(3):301-308. doi: 10.1111/joor.13288. Epub 2021 Dec 14. J Oral Rehabil. 2022. PMID: 34862971
-
Association of radiographic and clinical findings in patients with temporomandibular joints osseous alteration.Clin Oral Investig. 2020 Jan;24(1):221-227. doi: 10.1007/s00784-019-02945-6. Epub 2019 May 11. Clin Oral Investig. 2020. PMID: 31079244
-
Validation of the clinical diagnostic criteria for temporomandibular disorders for the diagnostic subgroup of degenerative joint disease.J Oral Rehabil. 2003 Apr;30(4):401-6. doi: 10.1046/j.1365-2842.2003.01035.x. J Oral Rehabil. 2003. PMID: 12631164
Cited by
-
Diagnostic Value of Panoramic Radiographs in the Assessment of Degenerative Joint Disease: A Retrospective Study.Int Dent J. 2025 Jul 19;75(5):100910. doi: 10.1016/j.identj.2025.100910. Online ahead of print. Int Dent J. 2025. PMID: 40684678 Free PMC article.
References
-
- Thamwatharsaree N, Panyarak W, Wantanajittikul K, Yarach U, Tachasuttirut K. Does articular disc position change following mandibular setback surgery? J Oral Maxillofac Surg. 2024;82:144–51. - PubMed
-
- Su C-L, Su A-C, Chang C-C, Lin AY-H, Yeh C-H. Temporomandibular joint degenerative changes following mandibular fracture: a computed tomography-based study on the role of condylar involvement. Oral Radiol. 2024;40:385–93. - PubMed
-
- Hu X, Sujanamulk B, Lakshmi CR, Li C. Age and gender-related morphometric assessment and degenerative changes of temporomandibular joint in symptomatic subjects and controls using cone beam computed tomography (CBCT): a comparative analysis. Curr Med Imaging. 2024;20:1–12. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

