Incidence of extended spectrum beta-lactamase (ESBL) producing Escherichia coli isolated from women with urinary tract infections in Jordan
- PMID: 40330060
- PMCID: PMC12049747
- DOI: 10.18502/ijm.v17i1.17800
Incidence of extended spectrum beta-lactamase (ESBL) producing Escherichia coli isolated from women with urinary tract infections in Jordan
Abstract
Background and objectives: Urinary tract infections are one of the world's major health problems. In addition, clinical disorders may result from the presence of bacteria or fungi in urine. The aim of this study was to isolate Escherichia coli (E. coli) strains from midstream urine samples, and to determine molecular characterization of encoded Extended Spectrum Beta-Lactamase (ESBL) genes.
Materials and methods: Collected urine samples were streaked on MacConkey, blood and EMB agar plates, then identifying E. coli isolates by using antibiotic susceptibility tests. ESBL production was measured using double disc diffusion. Furthermore, uniplex PCR was performed to identify two ESBL genes (bla CTX and bla TEM).
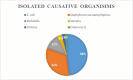
Results: Among 412 isolates, 198 (48.1%) were E. coli strains, followed by Staphylococcus saprophyticus, Klebsiella sp., Serratia sp., Enterococci sp. and Proteus sp. with frequency of 132 (32.0%), 51 (12.4%), 15 (3.6%), 10 (2.4%), and 6 (1.5%) respectively. Female participants who were between the ages of 40 and 49 years old, married, and pregnant were more likely to develop urinary tract infections (UTIs). E. coli species were present in 189 (95.5) of the recurrent UTIs. Regarding antimicrobial susceptibility testing of E. coli isolates, the highest percentage of resistance and susceptible rates were found for nalidixic acid (75.8%) and gentamicin (64.1%) respectively. Among the E. coli isolates, 25 (12.6%) were ESBL-producers. The bla CTX-M gene was genetically confirmed in 20 (10.1%) of the isolates.
Conclusion: E. coli is the most common cause of UTI and ESBL production leads to increased resistance to common antibiotics and complicates treatment strategies.
Keywords: Antibiotic resistance; Erythromycin; Escherichia coli; Extended-spectrum beta-lactamase; Urinary tract infections; blaCTX-M gene.
Copyright© 2025 The Author. Published by Tehran University of Medical Sciences.
Figures

Similar articles
-
Molecular characteristics and antibiotic resistance profiles of Escherichia coli strains isolated from urinary tract infections in children admitted to children's referral hospital of Qom, Iran.Ann Ig. 2019 May-Jun;31(3):252-262. doi: 10.7416/ai.2019.2288. Ann Ig. 2019. PMID: 31069370
-
Integron-mediated multidrug resistance in extended-spectrum β-lactamase-producing Escherichia coli and Klebsiella pneumoniae isolated from fecal specimens in Egypt.J Egypt Public Health Assoc. 2016 Jun;91(2):73-9. doi: 10.1097/01.EPX.0000483165.56114.d8. J Egypt Public Health Assoc. 2016. PMID: 27455084
-
Prevalence of TEM, SHV, and CTX-M genes of extended-spectrum β-lactamase-producing Escherichia coli strains isolated from urinary tract infections in adults.3 Biotech. 2017 Aug;7(4):244. doi: 10.1007/s13205-017-0879-2. Epub 2017 Jul 14. 3 Biotech. 2017. PMID: 28710743 Free PMC article.
-
Molecular characterization of extended spectrum β -lactamases enterobacteriaceae causing lower urinary tract infection among pediatric population.Antimicrob Resist Infect Control. 2018 Jul 28;7:90. doi: 10.1186/s13756-018-0381-6. eCollection 2018. Antimicrob Resist Infect Control. 2018. PMID: 30069306 Free PMC article.
-
High prevalence of CTX-M-15 and first report of CTX-M-3, CTX-M-22, CTX-M-28 and plasmid-mediated AmpC beta-lactamase producing Enterobacteriaceae causing urinary tract infections in Bosnia and Herzegovina in hospital and community settings.J Infect Chemother. 2015 May;21(5):363-9. doi: 10.1016/j.jiac.2015.01.003. Epub 2015 Jan 9. J Infect Chemother. 2015. PMID: 25638292
Cited by
-
Epidemiology, antibiotic resistance, and molecular detection of blaOXA and blaCTX-M Genes in ESBL-Producing Escherichia coli from urinary tract infections in Jordanian hospitals.BMC Microbiol. 2025 Aug 28;25(1):557. doi: 10.1186/s12866-025-04156-4. BMC Microbiol. 2025. PMID: 40877762 Free PMC article.
References
-
- Kaur R, Kaur R. Symptoms, risk factors, diagnosis and treatment of urinary tract infections. Postgrad Med J 2021; 97: 803–812. - PubMed
-
- Sahu R, Sahoo RK, Prusty SK, Sahu PK. Urinary tract infection and its management. Syst Rev Pharm 2019; 10: 42–48.
-
- Salari N, Khoshbakht Y, Hemmati M, Khodayari Y, Khaleghi AA, Jafari F, et al. Global prevalence of urinary tract infection in pregnant mothers: a systematic review and meta-analysis. Public Health 2023; 224: 58–65. - PubMed
-
- Víquez-Molina G, Aragón-Sánchez J, Pérez-Corrales C, Murillo-Vargas C, López-Valverde ME, Lipsky BA. Virulence factor genes in Staphylococcus aureus isolated from Diabetic foot soft tissue and bone infections. Int J Low Extrem Wounds 2018; 17: 36–41. - PubMed
LinkOut - more resources
Full Text Sources
