Association of the gut microbiota with type 2 diabetes: Links to disease and remission in the Japanese population
- PMID: 40331921
- PMCID: PMC12209512
- DOI: 10.1111/jdi.70061
Association of the gut microbiota with type 2 diabetes: Links to disease and remission in the Japanese population
Abstract
Background: Although the gut microbiota is associated with type 2 diabetes (T2D) and its remission in clinical settings, their relationship in the general population remains unclear. This study aimed to investigate the association between the gut microbiota and T2D and its remission in a population-based setting.
Methods: A cross-sectional study was conducted on 1,639 Japanese participants with (n = 106) or without (n = 1,533) T2D. The gut microbiota was compared between the two groups using multivariable-adjusted logistic regression. The relative abundance of the gut microbiota in fecal samples was calculated using 16S ribosomal RNA amplification. The association between the gut microbiota and T2D remission was determined via longitudinal analyses.
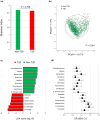
Results: Six genera were independently associated with T2D; a higher abundance of Faecalibacterium, Blautia, Roseburia, and Oscillibacter was significantly associated with a lower odds ratio for T2D, whereas a higher abundance of Megasphaera and Lactobacillus was significantly associated with a higher odds ratio for T2D. Of these, only Blautia abundance was significantly increased in the remission group compared with that in the non-remission group. In the remission group, an increase in Blautia abundance was significantly correlated with an increase in adiponectin level and skeletal muscle mass.
Conclusions: Specific gut microbes were significantly associated with T2D and its remission. The gut microbiota may represent a potential area for further exploration in T2D treatment and prevention. However, additional large-scale cohort studies or intervention studies using a probiotic or prebiotic approach are needed to validate these findings.
Keywords: Gut microbiota; Remission; Type 2 diabetes.
© 2025 The Author(s). Journal of Diabetes Investigation published by Asian Association for the Study of Diabetes (AASD) and John Wiley & Sons Australia, Ltd.
Conflict of interest statement
K. K., N. O., T. Y., K. M. (Kenta Mori), and Y. K. are employed by Kao Corporation (Tokyo, Japan). All other authors declare no potential competing interests. The results of the study are presented clearly, honestly, and without fabrication, falsification, or inappropriate data manipulation.
Approval of the research protocol: The study was approved by the Ethics Committee of Hirosaki University COI‐NEXT (HCN2024‐19‐0723) and conducted in accordance with the principles of the Declaration of Helsinki.
Informed consent: Written informed consent was obtained from all participants prior to the health check‐up. In this study, participants had the opportunity to object to the use of their data, but none of the participants did.
Approval date of Registry and the Registration No. of the study/trial: N/A.
Animal studies: N/A.
Figures

Similar articles
-
[Relationship Between Different Traditional Chinese Medicine Syndrome Types and Gut Microbiota in Patients With Type 2 Diabetes Mellitus].Sichuan Da Xue Xue Bao Yi Xue Ban. 2025 Mar 20;56(2):389-399. doi: 10.12182/20250360507. Sichuan Da Xue Xue Bao Yi Xue Ban. 2025. PMID: 40599291 Free PMC article. Chinese.
-
Association of gut microbiota with overweight/obesity combined with gestational diabetes mellitus.J Med Microbiol. 2025 May;74(5):002010. doi: 10.1099/jmm.0.002010. J Med Microbiol. 2025. PMID: 40366751 Free PMC article.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
-
Validation of the IHE type 2 diabetes cohort model in the Japanese clinical setting.J Med Econ. 2025 Dec;28(1):944-963. doi: 10.1080/13696998.2025.2517506. Epub 2025 Jun 22. J Med Econ. 2025. PMID: 40501229
Cited by
-
Type 2 Diabetes Mellitus Remission, Dream or Reality? A Narrative Review of Current Evidence and Integrated Care Strategies.Diabetes Ther. 2025 Aug;16(8):1557-1579. doi: 10.1007/s13300-025-01761-4. Epub 2025 Jun 13. Diabetes Ther. 2025. PMID: 40512404 Free PMC article. Review.
References
-
- International Diabetes Federation , IDF diabetes atlas, 10th ed. International Diabetes Federation, 2021. https://diabetesatlas.org/atlas/tenth‐edition/.
-
- Heitmeier S, Kiessling S, Clavell T, et al. Arrhythmic gut microbiome signatures predict risk of type 2 diabetes. Cell Host Microbe 2020; 28: 258–272.e6. - PubMed
MeSH terms
Supplementary concepts
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

