Relationship between the systemic immune-inflammatory index and overactive bladder risk: A cross-sectional assessment involving United States Adults
- PMID: 40333820
- PMCID: PMC12057966
- DOI: 10.1371/journal.pone.0323052
Relationship between the systemic immune-inflammatory index and overactive bladder risk: A cross-sectional assessment involving United States Adults
Abstract
Aims: This study aimed to evaluate the association between the systemic immune-inflammatory index (SII) and the risk of overactive bladder (OAB) in the adult United States population.
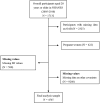
Methods: Data from the National Health and Nutrition Examination Survey (NHANES) 2005-2010 were analyzed. A non-pregnant cohort aged ≥20 years with available SII and OAB data was included. Weighted univariate and multivariate logistic regression analyses were performed to assess the association between SII and OAB risk. Additionally, subgroup, interaction, and restricted cubic spline analyses were conducted.
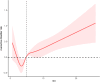
Results: A total of 4,545 participants were included, of whom 16.13% had OAB, with a mean SII of 5.75 ± 0.07. OAB risk increased with higher SII tertiles. In the fully adjusted model (Model 2), individuals in the highest SII tertile exhibited a 41% higher risk of OAB compared to those in the lowest tertile (OR: 1.41, 95% CI: 1.13-1.76, P = 0.004). Two-piece-wise regression analysis identified an SII breakpoint at 3.40, where a significant positive association was found for SII ≥ 3.40 (OR = 1.06, P < 0.0001), whereas no significant association was detected for SII < 3.40 (P = 0.06). Subgroup and interaction analyses revealed a consistent relationship between SII and OAB across different population strata, except for diabetes mellitus.
Conclusion: SII, an easily accessible biomarker, was independently associated with an increased risk of OAB, highlighting its potential utility in diagnostic prediction.
Copyright: © 2025 Zheng et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
The association between overactive bladder and systemic immunity-inflammation index: a cross-sectional study of NHANES 2005 to 2018.Sci Rep. 2024 May 31;14(1):12579. doi: 10.1038/s41598-024-63448-3. Sci Rep. 2024. PMID: 38822015 Free PMC article.
-
Association between novel inflammatory markers and overactive bladder: a cross-sectional study of NHANES 2009 to 2018.BMC Urol. 2025 Apr 8;25(1):78. doi: 10.1186/s12894-025-01743-5. BMC Urol. 2025. PMID: 40197316 Free PMC article.
-
Associations between serum total bilirubin and overactive bladder from the National Health and Nutrition Examination Survey.Front Endocrinol (Lausanne). 2025 Jan 14;15:1421426. doi: 10.3389/fendo.2024.1421426. eCollection 2024. Front Endocrinol (Lausanne). 2025. PMID: 39877842 Free PMC article.
-
Association between weight-adjusted waist index and overactive bladder syndrome among adult women in the United States: a cross-sectional study.BMC Womens Health. 2024 Sep 4;24(1):488. doi: 10.1186/s12905-024-03339-x. BMC Womens Health. 2024. PMID: 39232696 Free PMC article.
-
Association Between Systemic Immune-Inflammation Index and Psoriasis, Psoriasis Comorbidities, and All-Cause Mortality: A Study Based on NHANES.Immun Inflamm Dis. 2024 Oct;12(10):e70050. doi: 10.1002/iid3.70050. Immun Inflamm Dis. 2024. PMID: 39467182 Free PMC article. Review.
References
-
- Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, et al.. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn. 2010;29(1):4-20. - PubMed
-
- Mingin GC, Heppner TJ, Tykocki NR, Erickson CS, Vizzard MA, Nelson MT. Social stress in mice induces urinary bladder overactivity and increases TRPV1 channel-dependent afferent nerve activity. Am J Physiol Regul Integr Comp Physiol. 2015;309(6):R629-38. doi: 10.1152/ajpregu.00013.2015 - DOI - PMC - PubMed
-
- Irwin DE, Milsom I, Hunskaar S, Reilly K, Kopp Z, Herschorn S, et al.. Population-based survey of urinary incontinence, overactive bladder, and other lower urinary tract symptoms in five countries: results of the EPIC study. Eur Urol. 2006;50(6):1306–14; discussion 1314-5. doi: 10.1016/j.eururo.2006.09.019 - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical