Assessment of cardiovascular disease risk factors in Korean children: impact of various pediatric hypertension guidelines and application of the Korean blood pressure reference
- PMID: 40335981
- PMCID: PMC12060489
- DOI: 10.1186/s12887-025-05713-6
Assessment of cardiovascular disease risk factors in Korean children: impact of various pediatric hypertension guidelines and application of the Korean blood pressure reference
Abstract
Background: The global rise in pediatric hypertension (HTN) is a significant concern as it serves as a precursor to cardiovascular disease (CVD). To address this, we performed a comparative analysis of two guidelines for pediatric HTN: the 2017 American Academy of Pediatrics (AAP) and the 2016 European Society for Hypertension (ESH), applying the Korean blood pressure (BP) reference specifically to the Korean pediatric population.
Methods: Data from 2,060 children and adolescents aged 10-18 years from the Korean National Health and Nutrition Examination Survey (2016-2018) were analyzed. BP was classified according to the AAP, the ESH, and the Korea Regional BP Classification (KRC). High BP was defined as BP exceeding the normotensive range.
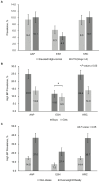
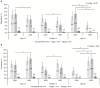
Results: The prevalence of high BP in Korean youth was significantly higher according to the AAP group than that in the ESH group (19.5% vs. 10.6%, P < 0.0001). Variations in prevalence were noted based on age, sex, and obesity. No significant differences were observed between the AAP and KRC groups in terms of high BP prevalence. The application of the AAP and KRC provided a more comprehensive reflection of CVD risk factors, including obesity and metabolic profiles, compared to the ESH. The KRC showed a tendency to classify more non-obese individuals as having elevated BP, although this difference was not statistically significant.
Conclusions: In comparing the AAP, ESH, and KRC criteria in the Korean pediatric population, the KRC demonstrated a tendency to identify individuals with CVD risk factors as having high BP. This finding suggests that using the KRC as the criterion for high BP may facilitate earlier intervention in the management of CVD risk.
Keywords: Cardiovascular disease; Korean population; Pediatric hypertension.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: The present study was approved by the Institutional Review Board (IRB) of Samsung Medical Center (IRB number 21-10-074). The informed consent was waived by IRB of Samsung Medical Center. All the data were obtained in accordance with the ethical principles for medical research involving human subjects established in the Declaration of Helsinki 1975 (revised in 2000). Consent for publication: Not applicable. Competing interests: The authors declare no competing interests. Clinical trial number: Not applicable.
Figures
Similar articles
-
Difference in the Prevalence of Elevated Blood Pressure and Hypertension by References in Korean Children and Adolescents.Front Med (Lausanne). 2022 Feb 24;9:793771. doi: 10.3389/fmed.2022.793771. eCollection 2022. Front Med (Lausanne). 2022. PMID: 35280904 Free PMC article.
-
The American Academy of Pediatrics hypertension guidelines identify obese youth at high cardiovascular risk among individuals non-hypertensive by the European Society of Hypertension guidelines.Eur J Prev Cardiol. 2020 Jan;27(1):8-15. doi: 10.1177/2047487319868326. Epub 2019 Aug 6. Eur J Prev Cardiol. 2020. PMID: 31387383
-
Impact of the 2017 American Academy of Pediatrics Guideline on Hypertension Prevalence Compared With the Fourth Report in an International Cohort.Hypertension. 2019 Dec;74(6):1343-1348. doi: 10.1161/HYPERTENSIONAHA.119.13807. Epub 2019 Oct 21. Hypertension. 2019. PMID: 31630571 Review.
-
Impact of ESH and AAP hypertension guidelines for children and adolescents on office and ambulatory blood pressure-based classifications.J Hypertens. 2019 Dec;37(12):2414-2421. doi: 10.1097/HJH.0000000000002229. J Hypertens. 2019. PMID: 31688292
-
Comparison of the 2017 American Academy of Pediatrics with the fourth report and the 2016 European Society of Hypertension guidelines for the diagnosis of hypertension and the detection of left ventricular hypertrophy in children and adolescents: a systematic review and meta-analysis.J Hypertens. 2022 Feb 1;40(2):197-204. doi: 10.1097/HJH.0000000000003005. J Hypertens. 2022. PMID: 34475347
References
-
- Xi B, Bovet P, Hong YM, Zong X, Chiolero A, Kim HS, et al. Recent blood pressure trends in adolescents from China, Korea, Seychelles and the united States of America, 1997–2012. J Hypertens. 2016;34(10):1948–58. 10.1097/hjh.0000000000001058. - PubMed
-
- Daniels SR, Loggie JM, Khoury P, Kimball TR. Left ventricular geometry and severe left ventricular hypertrophy in children and adolescents with essential hypertension. Circulation. 1998;97(19):1907–11. 10.1161/01.cir.97.19.1907. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

