Effects of continuous positive airway pressure therapy on inflammatory markers in patients with obstructive sleep apnea: a meta-analysis of randomized controlled trials
- PMID: 40346316
- PMCID: PMC12064446
- DOI: 10.1007/s11325-025-03348-6
Effects of continuous positive airway pressure therapy on inflammatory markers in patients with obstructive sleep apnea: a meta-analysis of randomized controlled trials
Abstract
Objective: In this meta-analysis, we provide the findings of randomized controlled trials on the levels of inflammatory markers in patients with obstructive sleep apnea (OSA) receiving continuous positive airway pressure (CPAP).
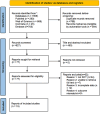
Methods: Literature published in the PubMed, Web of Science, Embase and Cochrane databases up to May 21, 2024, was comprehensively searched, and inclusion and exclusion criteria were developed. Pooled estimates of CPAP therapy were analyzed via the standardized mean difference (SMD). This meta-analysis follows the PRISMA 2020 guidelines and is registered with PROSPERO (ID CRD42024548588).
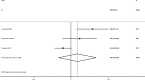
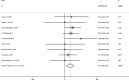
Results: A total of 15 studies were included, each reporting data on one or more inflammatory markers, as follows: 10 studies on C-reactive protein (CRP), 12 studies on interleukin-6 (IL-6), 3 studies on interleukin-8 (IL-8), and 9 studies on tumor necrosis factor-α (TNF-α). The results revealed that the SMDs (95% confidence intervals [CIs]) for CRP, IL-6, IL-8 and TNF-α levels before and after CPAP treatment were 0.88 (95% CI 0.28-1.48), 0.58 (95% CI 0.12-1.05), 0.20 (95% CI 0.39-0.80) and 0.17 (95% CI 0.05-0.29), separately.
Conclusion: CPAP therapy used for a certain duration can lower CRP, IL-6 and TNF-α levels in OSA patients, and there are substantial differences observed in the various inflammatory indicators. To confirm the usefulness of these biomarkers in evaluating CPAP therapy for cardiovascular risk reduction among OSA patients, more randomized controlled trials (RCTs) have to be carried out in the future.
Keywords: Continuous positive airway pressure; Inflammatory markers; Meta-analysis; Obstructive sleep apnea.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethical approval: Ethical permission was not sought for this meta-analysis, as only pooled data from previously permitted individual studies were included. Informed consent: Every individual participant in the earlier research gave their informed permission. Conflict of interest: The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as potential conflicts of interest.
Figures


Similar articles
-
CPAP Does Not Reduce Inflammatory Biomarkers in Patients With Coronary Artery Disease and Nonsleepy Obstructive Sleep Apnea: A Randomized Controlled Trial.Sleep. 2017 Nov 1;40(11). doi: 10.1093/sleep/zsx157. Sleep. 2017. PMID: 29029237 Clinical Trial.
-
Effects of continuous positive airway pressure on cardiovascular biomarkers in patients with obstructive sleep apnea: a meta-analysis of randomized controlled trials.Sleep Breath. 2019 Mar;23(1):77-86. doi: 10.1007/s11325-018-1662-2. Epub 2018 Apr 22. Sleep Breath. 2019. PMID: 29682699
-
Effects of continuous positive airway pressure therapy on systemic inflammation in obstructive sleep apnea: a meta-analysis.Sleep Med. 2013 Nov;14(11):1139-50. doi: 10.1016/j.sleep.2013.07.006. Epub 2013 Aug 14. Sleep Med. 2013. PMID: 24054505
-
Efficacy of continuous positive airway pressure on subcutaneous adipose tissue in patients with obstructive sleep apnea: a meta-analysis of randomized controlled trials.Sleep Breath. 2021 Mar;25(1):1-8. doi: 10.1007/s11325-020-02078-1. Epub 2020 Apr 24. Sleep Breath. 2021. PMID: 32333260 Review.
-
Impact of continuous positive airway pressure on vascular endothelial growth factor in patients with obstructive sleep apnea: a meta-analysis.Sleep Breath. 2019 Mar;23(1):5-12. doi: 10.1007/s11325-018-1660-4. Epub 2018 Apr 18. Sleep Breath. 2019. PMID: 29671205 Review.
Cited by
-
Obstructive sleep apnea is a risk factor for incident COVID-19 infection.Sleep Breath. 2025 Jun 25;29(4):226. doi: 10.1007/s11325-025-03401-4. Sleep Breath. 2025. PMID: 40560295 No abstract available.
References
-
- Martinez D, Klein C, Rahmeier L, Silva RP, Da CZ, Fiori CM, Cassol SC, Goncalves, Bos AJ (2012) Sleep apnea is a stronger predictor for coronary heart disease than traditional risk factors. Sleep Breath 2012:695–701. 10.1007/s11325-011-0559-0 - PubMed
-
- Yilmaz F, Ozyildirim S, Talay F, Karaaslan K, Gunduz H (2007) Obstructive sleep apnea as a risk factor for cardiovascular diseases. Cardiol. J 2007:534–537 - PubMed
-
- Ip MS, Tse HF, Lam B, Tsang KW, Lam WK (2004) Endothelial function in obstructive sleep apnea and response to treatment. Am. J. Respir. Crit. Care Med 2004:348–353. 10.1164/rccm.200306-767OC - PubMed
-
- Dalmases M, Sole-Padulles C, Torres M, Embid C, Nunez MD, Martinez-Garcia MA, Farre R, Bargallo N, Bartres-Faz D, Montserrat JM (2015) Effect of CPAP on Cognition, Brain Function, and Structure Among Elderly Patients With OSA: A Randomized Pilot Study. Chest 2015:1214–1223. 10.1378/chest.15-0171 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

