Bridging the gap: family resilience as a mediator between parental psychological resilience and care competence in premature infant transitions
- PMID: 40349077
- PMCID: PMC12065373
- DOI: 10.1186/s40359-025-02797-8
Bridging the gap: family resilience as a mediator between parental psychological resilience and care competence in premature infant transitions
Abstract
Background: High levels of parental infant care competence could facilitate the transition of preterm infants from hospital to home and reduce their readmission rate and emergency visits after discharge. Researchers have confirmed psychological resilience and family resilience were excellent psychological resources that played important roles in the development of parental infant care competence. However, the interaction between these three variables in the parents of preterm infants remains unclear and requires further validation. This study aimed to explore the association between parental psychological resilience and premature infant care competence and the mediating role of family resilience on this relationship.
Methods: A multi-center cross-sectional study recruited a convenience sample of 381 parents of premature infants across four public hospitals in East China between November 2022 and December 2023. Research instruments included Connor-Davidson Resilience Scale, Family Hardiness Index, and Premature Infant Care Competency Scale. Structure equation modeling (SEM) were used to detect mediating effect of family resilience, while controlling for covariates.
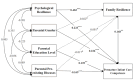
Results: The average score of parental premature infant care competence was 134.02 points. Differences in levels of premature infant care competence were found across parental gender, education levels and pre-existing diseases. The results of SEM showed a direct relationship between the mentioned three covariates and transitional parental premature infant care competence, but not with family resilience. SEM also revealed psychological resilience as a significant predictor of transitional parental care competence, exerting both direct effects (β = 0.318, P < 0.001, 95%CI: [0.166, 0.464]) and indirect effects (β = 0.111, P = 0.001, 95%CI: [0.049, 0.183]) mediated through family resilience.
Conclusions: The findings suggested higher psychological resilience related to better family resilience which can provide supportive environment, thus contributing to increased parental premature infant care competence. Future researchers could pay more attention to the early resilience assessment of parents and family resilience improvements based on the formation of therapeutic alliance with the entire family system of preterm babies.
Keywords: Cross-sectional survey; Family care; Parents; Premature infant; Resilience.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Ethical approval for this study was obtained from the Ethics Review Committee of Children’s Hospital of Shanghai(2022R110-E01). All methods were performed by the Declaration of Helsinki. Prior to the study, we obtained the informed consent of all participating parents. Data were kept confidential and processed anonymously. Consent for publication: Not applicable. Competing interests: The authors declare no competing interests.
Figures
References
-
- Chawanpaiboon S, Vogel JP, Moller AB, Lumbiganon P, Petzold M, Hogan D, Landoulsi S, Jampathong N, Kongwattanakul K, Laopaiboon M, et al. Global, regional, and National estimates of levels of preterm birth in 2014: a systematic review and modelling analysis. Lancet Glob Health. 2019;7(1):e37–46. - DOI - PMC - PubMed
-
- World Health Organization, Preterm. birth. 2023.https://www.who.int/es/news-room/fact-sheets/detail/preterm-birth. Accessed 4 March 2025.
-
- Zhang YJ, Zhu Y, Chen C. Incidence and trend of premature infants. Chin J Neonatology. 2021;36(04):74–7.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous