A rare case of multiple brain abscesses caused by Nocardia abscessus co-infection with tuberculous meningitis in an immunocompetent patient
- PMID: 40360973
- PMCID: PMC12070615
- DOI: 10.1186/s12879-025-11056-5
A rare case of multiple brain abscesses caused by Nocardia abscessus co-infection with tuberculous meningitis in an immunocompetent patient
Abstract
Background: Nocardial brain abscesses are extremely rare and predominantly affect immunocompromised patients, exhibiting a high overall mortality rate. Tuberculosis infections, although they can occur in immunocompetent individuals, are more prevalent in those with compromised immune systems. Tuberculous meningitis (TBM), the most severe manifestation of tuberculosis, is associated with a high fatality rate. Co-infection with both pathogens is unusual. To our knowledge, this is the first reported case of multiple brain abscesses caused by Nocardia abscessus (N. abscessus) in a young immunocompetent patient, complicated by tuberculous meningitis.
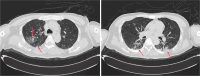
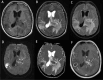
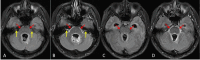
Case presentation: A 34-year-old male patient initially presented with a week-long history of headaches, predominantly localized in the bilateral frontal region. Additionally, the patient experienced fever, and due to the recurrence of these symptoms, he was admitted to the hospital. Chest computed tomography (CT) scans revealed bilateral pneumonia, and brain magnetic resonance imaging (MRI) strongly suggested the presence of multiple brain abscesses accompanied by meningitis. On the fourth day of hospitalization, the patient's condition deteriorated, becoming lethargic with severe headaches. His body temperature spiked to 39.5 °C, and signs of elevated intracranial pressure emerged. Subsequently, he underwent neuro-navigation-assisted resection of deep lesions, ventriculostomy for external drainage, and drainage of abscesses. The next day, cerebrospinal fluid (CSF) Xpert MTB/RIF testing yielded positive results for multiple probes and the Mycobacterium tuberculosis (MTB) complex. Pus cultures and sequencing further confirmed an N. abscessus infection. Consequently, the patient was diagnosed with multiple brain abscesses caused by N. abscessus, complicated by tuberculous meningitis. We administered TMP-SMX, imipenem-cilastatin, and intravenous linezolid for the management of nocardial brain abscesses infections, while continuing decompressive ventricular drainage. For empiric treatment of tuberculous meningitis, the patient was started on isoniazid 600 mg/day via intravenous injection, rifampicin 600 mg/day orally, pyrazinamide 1500 mg/day (divided into three oral doses), ethambutol 750 mg/day orally, and dexamethasone at an initial dose of 0.4 mg/kg/day, with a planned gradual reduction starting one week later. Despite 10 days of treatment, the patient showed no significant clinical improvement in the infection, and hydrocephalus worsened. On the 16th day of admission, emergency external ventricular drain placement was performed, and intrathecal amikacin was administered to combat the nocardial brain abscesses. Unfortunately, by the 39th day of admission, the patient's infection continued to progress, eventually succumbing to septic shock and resulting in death.
Conclusions: Nocardial brain abscesses are associated with a high mortality rate, especially among immunocompromised patients and those with multiple abscesses. Prompt diagnosis, aggressive surgical intervention, and sensitive antibiotic treatment offer the best prospects for curing nocardiosis. Tuberculous meningitis, the most lethal manifestation of Mycobacterium tuberculosis infection, often leads to severe outcomes primarily due to delayed diagnosis and treatment. The GeneXpert/RIF assay, an emerging diagnostic tool, provides a more sensitive and rapid means of detecting TBM. For patients with a high clinical suspicion of TBM, empirical anti-tuberculosis treatment should be initiated immediately. Timely and accurate management, coupled with continuous monitoring of the patient's condition, is crucial for achieving a favorable prognosis.
Clinical trial number: Not applicable.
Keywords: Nocardia abscessus; Brain abscesses; Case report; Co-infection; Tuberculous meningitis.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: The study was approved by the medical ethics committee of the People’s Hospital of Guangxi Zhuang Autonomous Region. The study is supported by the patient’s wife and she has signed informed consent. Consent for publication: Written informed consent was obtained from the patient’s wife for the publication of the case details. Competing interests: The authors declare no competing interests.
Figures

Similar articles
-
Triple-drug antibiotic therapy for disseminated nocardial abscess in the mediastinum and brain of an immunocompetent patient: a case report.BMC Infect Dis. 2025 Jan 8;25(1):42. doi: 10.1186/s12879-025-10445-0. BMC Infect Dis. 2025. PMID: 39780099 Free PMC article.
-
Utility of clinical metagenomics in complex infections: Cryptococcal meningitis complicated by Nocardia brain abscess.Diagn Microbiol Infect Dis. 2025 Sep;113(1):116895. doi: 10.1016/j.diagmicrobio.2025.116895. Epub 2025 May 8. Diagn Microbiol Infect Dis. 2025. PMID: 40367908
-
Idiopathic thrombocytopenic purpura with brain abscess caused by Nocardia farcinica diagnosed using metagenomics next-generation sequencing of the cerebrospinal fluid: a case report.BMC Infect Dis. 2021 Apr 23;21(1):380. doi: 10.1186/s12879-021-06071-1. BMC Infect Dis. 2021. PMID: 33892637 Free PMC article.
-
Successful management of Nocardia farcinica brain abscess in an immunocompetent adult with trimethoprim/sulfamethoxazole hypersensitivity: A case report and review.Diagn Microbiol Infect Dis. 2025 Oct;113(2):116954. doi: 10.1016/j.diagmicrobio.2025.116954. Epub 2025 Jun 11. Diagn Microbiol Infect Dis. 2025. PMID: 40543441 Review.
-
Mycobacterium tuberculosis combine with EBV infection in severe adult meningoencephalitis: a rare case reports and literature review.Front Cell Infect Microbiol. 2024 Oct 14;14:1361119. doi: 10.3389/fcimb.2024.1361119. eCollection 2024. Front Cell Infect Microbiol. 2024. PMID: 39469454 Free PMC article. Review.
References
-
- Kumar VA, Augustine D, Panikar D, Nandakumar A, Dinesh KR, Karim S, Philip R. Nocardia farcinica brain abscess: epidemiology, pathophysiology, and literature review. Surg Infect (Larchmt). 2014;15(5):640–6. - PubMed
-
- Mamelak AN, Obana WG, Flaherty JF, Rosenblum ML. Nocardial brain abscess: treatment strategies and factors influencing outcome. Neurosurgery. 1994;35(4):622–31. - PubMed
-
- Alijani N, Mahmoudzadeh S, Hedayat Yaghoobi M, Geramishoar M, Jafari S. Multiple brain abscesses due to nocardia in an immunocompetent patient. Arch Iran Med. 2013;16(3):192–4. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

