The effect of chronic yoga interventions on sleep quality in people with sleep disorders: a scoping review
- PMID: 40365457
- PMCID: PMC12071090
- DOI: 10.3389/fneur.2025.1566445
The effect of chronic yoga interventions on sleep quality in people with sleep disorders: a scoping review
Abstract
Background: Poor or insufficient sleep adversely affects various physiological and psychological functions, impacting body systems such as the endocrine, metabolic, and immune systems.
Objectives: Despite available pharmacological and non-pharmacological treatments, the impact of chronic yoga interventions on sleep quality in individuals with sleep problem syndrome remains underexplored. This scoping review aims to consolidate existing research on yoga interventions and their effects on sleep quality, providing evidence for yoga as a non-pharmacological alternative to reduce reliance on medications.
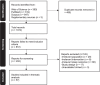
Methods: A systematic search across PubMed, Web of Science, and Scopus identified 1,559 studies, with 57 meeting inclusion criteria for yoga's effects on sleep quality.
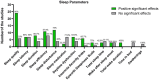
Results: Overall, the included studies reported either significant improvements in sleep quality (or related) parameters or no change. Moderator analyses revealed that intervention duration and session frequency can influence sleep outcomes. Short-duration interventions (≤6 weeks) showed a large mean effect on sleep quality (9.41%; 95% CI 3.06 to 15.42%), with 54% of studies reporting statistically significant improvements. Medium-duration interventions (7-16 weeks) demonstrated consistent benefits, including a large mean effect on sleep quality (8.74%; 95% CI 2.93 to 14.55%) and a very large reduction in insomnia severity (13.19%; 95% CI 11.10 to 15.98%). However, sleep efficiency exhibited smaller effects (0.73%; 95% CI -1.99 to 3.45%). Long-duration interventions (≥17 weeks) produced the most robust results, with 100% of the studies reporting significant improvements, including a 7.92% increase in sleep quality (95% CI 3.23 to 12.60%). With regard to session frequency, low-frequency sessions (1-2 per week) yielded significant improvements in insomnia severity (13.66%; 95% CI 8.72 to 18.59%) and sleep quality (8.13%; 95% CI 2.67 to 13.59%). Moderate-frequency sessions (3-4 per week) balanced accessibility and efficacy, producing a large mean effect on sleep quality (9.21%; 95% CI 3.66 to 14.76%). High-frequency sessions (≥5 per week) demonstrated a similarly large effect on sleep quality (8.24%; 95% CI 2.28 to 14.20%), although the data were limited.
Conclusion: Tailoring yoga interventions by duration and frequency is valuable, with chronic practice offering a safe, effective alternative to medication. Future research should refine protocols for specific populations and sleep challenges.
Keywords: exercise therapy; non-pharmacological treatment; sleep problem syndrome; sleep quality; yoga.
Copyright © 2025 Alghosi, Sharifi, Namavari, Rajamand, Bamorovat, Norouzi, Alimoradi and Konrad.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Optimal exercise dose and type for improving sleep quality: a systematic review and network meta-analysis of RCTs.Front Psychol. 2024 Oct 3;15:1466277. doi: 10.3389/fpsyg.2024.1466277. eCollection 2024. Front Psychol. 2024. PMID: 39421847 Free PMC article.
-
Speech and language therapy for management of chronic cough.Cochrane Database Syst Rev. 2019 Jul 23;7(7):CD013067. doi: 10.1002/14651858.CD013067.pub2. Cochrane Database Syst Rev. 2019. PMID: 31335963 Free PMC article.
-
Yoga for asthma.Sao Paulo Med J. 2016 Jul-Aug;134(4):368. doi: 10.1590/1516-3180.20161344T2. Sao Paulo Med J. 2016. PMID: 27557146 Free PMC article.
-
Chair-based yoga programme for older adults with multimorbidity: RCT with embedded economic and process evaluations.Health Technol Assess. 2024 Sep;28(53):1-152. doi: 10.3310/KPGN4216. Health Technol Assess. 2024. PMID: 39259017 Free PMC article. Clinical Trial.
-
Effects of Exercise on Sleep Quality and Insomnia in Adults: A Systematic Review and Meta-Analysis of Randomized Controlled Trials.Front Psychiatry. 2021 Jun 7;12:664499. doi: 10.3389/fpsyt.2021.664499. eCollection 2021. Front Psychiatry. 2021. PMID: 34163383 Free PMC article.
References
Publication types
LinkOut - more resources
Full Text Sources