Impact of SARS-CoV-2 Infection on the Outcomes of Trauma Patients at a Level I Trauma Center: An Ambispective Observational Study
- PMID: 40370923
- PMCID: PMC12076266
- DOI: 10.7759/cureus.82162
Impact of SARS-CoV-2 Infection on the Outcomes of Trauma Patients at a Level I Trauma Center: An Ambispective Observational Study
Abstract
Introduction: Trauma remained a leading cause of hospital admissions even during the COVID-19 pandemic. Trauma and surgical interventions are known to impair the patient's immune function. Clinically, some asymptomatic COVID-19 patients experienced rapid deterioration following surgery. Surgeons and anesthesiologists need to be aware that acute lung injury caused by COVID-19 could be present preoperatively or may worsen postoperatively. Hence, an ambispective observational study was planned to assess the impact of severe acute respiratory syndrome coronavirus (SARS-CoV-2) infection on trauma patient outcomes.
Aims and objectives: This study aims to evaluate the impact of SARS-CoV-2 infection on the outcomes of trauma patients at a level I trauma center.
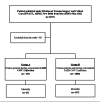
Materials and methods: This ambispective observational study was conducted at a level 1 trauma center and included patients admitted under the trauma surgery service in the COVID-19 facility. Their outcomes were compared with those of patients admitted to the non-COVID-19 facility from March 2020 to March 2022.
Results: A total of 2,017 patients were admitted under the Division of Trauma Surgery and Critical Care from March 2020 to March 2022. The mean duration of intercostal drainage (ICD) was significantly longer in SARS-CoV-2-positive trauma patients (7.03 ± 3.69 days) compared to SARS-CoV-2-negative trauma patients (5.28 ± 2.75). Acute respiratory distress syndrome (ARDS) was also more common among SARS-CoV-2-positive trauma patients. Additionally, these patients had a longer hospital stay. Notably, SARS-CoV-2-positive trauma patients who died had a significantly lower average injury severity score (ISS) compared to SARS-CoV-2-negative counterparts.
Discussion: Although the average ISS was lower and the average trauma and injury severity score (TRISS) was higher in SARS-CoV-2-positive trauma patients who died compared to SARS-CoV-2-negative trauma patients, overall mortality rates were comparable between the two groups.
Conclusion: Trauma patients with concomitant SARS-CoV-2 infection had a longer duration of ICD, along with an increased incidence of chest infections and ARDS. A greater proportion of SARS-CoV-2-positive trauma patients required ventilatory support. The mortality observed in SARS-CoV-2-positive trauma patients is likely attributed to the concomitant SARS-CoV-2 infection.
Keywords: covid-19; impact of sars-cov-2; sars cov-2; trauma; trauma mortality.
Copyright © 2025, Manwatkar et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. The Institute Ethics Committee For Post Graduate Research, All India Institute Of Medical Sciences, Ansari Nagar, New Delhi, 110029 issued approval IECPG-497/23.09.2021, RT-06/28.10.2021. Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures

Similar articles
-
Safety and Efficacy of Imatinib for Hospitalized Adults with COVID-19: A structured summary of a study protocol for a randomised controlled trial.Trials. 2020 Oct 28;21(1):897. doi: 10.1186/s13063-020-04819-9. Trials. 2020. PMID: 33115543 Free PMC article.
-
Testing the efficacy and safety of BIO101, for the prevention of respiratory deterioration, in patients with COVID-19 pneumonia (COVA study): a structured summary of a study protocol for a randomised controlled trial.Trials. 2021 Jan 11;22(1):42. doi: 10.1186/s13063-020-04998-5. Trials. 2021. PMID: 33430924 Free PMC article.
-
Analyzing the Impact of Concomitant COVID-19 Infection on Outcomes in Trauma Patients.Am Surg. 2024 Jun;90(6):1599-1607. doi: 10.1177/00031348241246176. Epub 2024 Apr 13. Am Surg. 2024. PMID: 38613452
-
Workplace interventions to reduce the risk of SARS-CoV-2 infection outside of healthcare settings.Cochrane Database Syst Rev. 2024 Apr 10;4(4):CD015112. doi: 10.1002/14651858.CD015112.pub3. Cochrane Database Syst Rev. 2024. PMID: 38597249 Free PMC article.
-
Inflammation, Thrombosis, and Destruction: The Three-Headed Cerberus of Trauma- and SARS-CoV-2-Induced ARDS.Front Immunol. 2020 Sep 25;11:584514. doi: 10.3389/fimmu.2020.584514. eCollection 2020. Front Immunol. 2020. PMID: 33101314 Free PMC article. Review.
References
-
- A novel coronavirus outbreak of global health concern. Wang C, Horby PW, Hayden FG, Gao GF. https://linkinghub.elsevier.com/retrieve/pii/S0140673620301859 The Lancet. 2020;395:470–473. - PMC - PubMed
-
- Challenges of diagnosis of COVID-19 in trauma patients: a case series. Sabetian G, Feiz F, Shakibafard A, et al. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7435208/ Trauma. 2020;23:218–229. - PMC - PubMed
-
- Incidence of adult respiratory distress syndrome in trauma patients: a systematic review and meta-analysis over a period of three decades. Pfeifer R, Heussen N, Michalewicz E, Hilgers RD, Pape HC. J Trauma Acute Care Surg. 2017;83:496–506. - PubMed
-
- Impact and modifications of in-hospital trauma care workflow due to COVID 19 pandemic: lessons learnt for the future. Kaushik G, Sharma A, Bagaria D, Kumar S, Sagar S, Gupta A. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8195829/ Bull Emerg Trauma. 2021;9:60–66. - PMC - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
