Role of Heart Rate Recovery in Chronic Heart Failure: Results From the MyoVasc Study
- PMID: 40371587
- PMCID: PMC12184589
- DOI: 10.1161/JAHA.124.039792
Role of Heart Rate Recovery in Chronic Heart Failure: Results From the MyoVasc Study
Abstract
Background: Cardiac autonomic dysfunction is associated with heart failure (HF). Reduced heart rate recovery (HRR) indicates impaired parasympathetic reactivation after physical activity. Heart rate recovery 60 seconds after peak effort (HRR60) is linked to autonomic dysfunction, but data on its relevance across HF phenotypes are scarce. This study aimed to identify clinical determinants of HRR60 in an HF cohort and assess its relationship with clinical outcomes.
Methods: Data from the MyoVasc study (NCT04064450; N=3289) were analyzed. Participants underwent standardized clinical phenotyping including cardiopulmonary exercise testing. HRR60 was defined as the heart rate decline 60 seconds after exercise termination. Clinical determinants of HRR60 were evaluated using multivariate regression, whereas Cox regression analyses assessed all-cause death and worsening of HF.
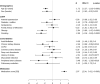
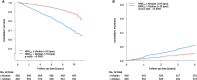
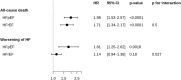
Results: The analysis sample comprised 1289 individuals (median age, 66.0 [interquartile range {IQR}, 58.0-73.0] years, 30.4% women) ranging from stage B to stage C/D according to the universal definition of HF. Age, sex, smoking, obesity, peripheral artery disease, and chronic kidney disease were identified as determinants of HRR60. HRR60 showed a strong association with all-cause death (hazard ratio [HR]HRR60 [10 bpm], 1.56 [95% CI, 1.32-1.85]; P<0.0001) and worsening of HF (HRHRR60 [10 bpm], 1.36 [95% CI, 1.10-1.69]; P=0.0052) independent of age, sex, and clinical profile. Sensitivity analysis showed a stronger association with worsening HF in HF with preserved left ventricular ejection fraction (Pinteraction=0.027).
Conclusions: HRR60 was associated with clinical outcome in chronic HF. Because it showed a stronger association with outcomes in HF with preserved ejection fraction, future research should consider phenotype-specific differences.
Keywords: all‐cause death; autonomic dysfunction; heart failure; heart rate recovery; prognosis; worsening of heart failure.
Conflict of interest statement
Dr Wild reports, for the submitted work, grants from Bayer AG. Outside the submitted work, he reports nonfinancial grants from Philips Medical Systems, grants and consulting fees from Boehringer Ingelheim, Daiichi Sankyo Europe, Novartis Pharma, Sanofi‐Aventis, grants, consulting, and lecturing fees from Bayer Health Care, lecturing fees from Pfizer Pharma, lecturing fees from Bristol Myers Squibb, consulting fees from Astra Zeneca, consulting fees and nonfinancial support from Diasorin, and nonfinancial support from I.E.M. Dr Wild is the principal investigator of the future cluster curATime (BMBF 03ZU1202AA, 03ZU1202CD, 03ZU1202DB, 03ZU1202JC, 03ZU1202KB, 03ZU1202LB, 03ZU1202MB, and 03ZU1202OA) and principal investigator of the DIASyM research core, which focuses on the study of the heart failure syndrome (BMBF 161L0217A). Drs Wild and Münzel are principal investigators of the German Center for Cardiovascular Research, Partner Site Rhine‐Main, Mainz, Germany. Dr Prochaska has received honoraria for lectures from Bayer AG, Boehringer Ingelheim, Daiichi‐Sankyo, and Sanofi Aventis outside the topic of this work. Dr. Prochaska has received research funding from the German Center for Cardiovascular Research, which focuses on the study of HF. Dr Tröbs has received lecture fees from Philips AG outside the submitted work. Drs Dinh, Prochaska, and Tröbs, and G Buch are employees of Boehringer Ingelheim. Dr Müller is supported by a rotation grant of the Heart of Mainz Foundation. Dr Velmeden has received lecture fees from Astra Zeneca outside the submitted work. Dr. Mondritzki is an employee of Bayer AG.
Figures
References
-
- Vos T, Flaxman AD, Naghavi M, Lozano R, Michaud C, Ezzati M, Shibuya K, Salomon JA, Abdalla S, Aboyans V, et al. Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the global burden of disease study 2010. Lancet. 2012;380:2163–2196. doi: 10.1016/S0140-6736(12)61729-2 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

