The combination of left ventricular ejection fraction and end-diastolic diameter and outcomes in peritoneal dialysis patients: a multicenter retrospective study
- PMID: 40384403
- PMCID: PMC12090317
- DOI: 10.1080/0886022X.2025.2497493
The combination of left ventricular ejection fraction and end-diastolic diameter and outcomes in peritoneal dialysis patients: a multicenter retrospective study
Abstract
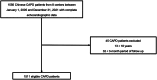
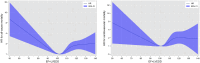
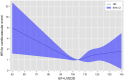
End-stage renal disease (ESRD) is often complicated by left ventricular dysfunction, which is associated with a poor prognosis. This study aims to investigate the association between baseline left ventricular ejection fraction (LVEF) plus left ventricular end-diastolic diameter (LVEDD) with outcomes in peritoneal dialysis (PD) patients. In this multicenter retrospective study, 1,511 incident Chinese patients on PD between 1 January 2005 and 31 December 2021 were enrolled. Restricted cubic splines (RCS) were used to explore the non-linear associations between LVEF+LVEDD and the risk of mortality. Parametric models for interval-censored survival-time data (stintreg) were used to examine the association between LVEF+LVEDD quartiles and the outcomes. During 6,451.11 person-years of follow-up [median 4.81 (IQR 3.61-6.81) years], 247 (17.8%) patients died, including 88 cardiovascular deaths. RCS showed a U-shaped association between LVEF+LVEDD and the risks of all-cause and CV mortality. According to the quartiles, the optimal range of LVEF+LVEDD associated with the lowest risk of all-cause and CV mortality was 103-107, which was set as the reference range. Both higher (≥115) and lower (<103) levels of LVEF+LVEDD were associated with increased risks of all-cause mortality (hazard ratio [HR] 2.20, 95% confidence interval [CI] 1.58-3.07; HR 1.68, 95% CI 1.19-2.36) and cardiovascular mortality (HR 2.51, 95% CI 1.33-4.75; HR 1.86, 95% CI 0.96-3.61). Low and high levels of baseline LVEF+LVEDD were associated with increased risks of all-cause and cardiovascular mortality in PD patients.
Keywords: Left ventricular ejection fraction; left ventricular end-diastolic diameter; mortality; peritoneal dialysis.
Conflict of interest statement
No potential conflict of interest was reported by the author(s).
Figures


Similar articles
-
Association of left ventricular systolic dysfunction with mortality in incident peritoneal dialysis patients.Nephrology (Carlton). 2018 Oct;23(10):927-932. doi: 10.1111/nep.13154. Nephrology (Carlton). 2018. PMID: 28815812
-
Aortic valve replacement for severe aortic regurgitation in asymptomatic patients with normal ejection fraction and severe left ventricular dilatation.Interact Cardiovasc Thorac Surg. 2016 Apr;22(4):425-30. doi: 10.1093/icvts/ivv365. Epub 2015 Dec 30. Interact Cardiovasc Thorac Surg. 2016. PMID: 26718321
-
Associations of sensitive cardiac troponin-I with left ventricular morphology, function and prognosis in end-stage renal disease patients with preserved ejection fraction.Heart Vessels. 2018 Nov;33(11):1334-1342. doi: 10.1007/s00380-018-1192-7. Epub 2018 May 22. Heart Vessels. 2018. PMID: 29789900
-
Prevalence of left ventricular systolic dysfunction in pre-dialysis and dialysis patients with preserved left ventricular ejection fraction.Eur J Heart Fail. 2018 Mar;20(3):560-568. doi: 10.1002/ejhf.1077. Epub 2017 Nov 21. Eur J Heart Fail. 2018. PMID: 29164753
-
Blood pressure and cardiovascular mortality in dialysis patients with left ventricular systolic dysfunction.Am J Hypertens. 2014 Mar;27(3):401-8. doi: 10.1093/ajh/hpt190. Epub 2013 Oct 9. Am J Hypertens. 2014. PMID: 24108864
References
-
- Fatema K, Hirono O, Takeishi Y, et al. . Hemodialysis improves myocardial interstitial edema and left ventricular diastolic function in patients with end-stage renal disease: noninvasive assessment by ultrasonic tissue characterization. Heart Vessels. 2002;16(6):227–231. doi: 10.1007/s003800200029. - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
