The natural history of anal high-grade squamous intraepithelial lesions among MSM and transgender women in an acute HIV cohort in Thailand
- PMID: 40387542
- PMCID: PMC12337930
- DOI: 10.1097/QAD.0000000000004238
The natural history of anal high-grade squamous intraepithelial lesions among MSM and transgender women in an acute HIV cohort in Thailand
Abstract
Objective: To describe the incidence and clearance rates of anal high-grade squamous intraepithelial lesions (HSIL) among MSM and transgender women who initiated immediate antiretroviral therapy during acute HIV acquisition.
Design: A prospective cohort study of MSM and transgender women diagnosed with acute HIV acquisition in Bangkok, Thailand.
Methods: Participants who were enrolled from May 2017 to June 2020 underwent anal human papillomavirus (HPV) genotyping, high-resolution anoscopy, and anal biopsies as indicated, at baseline and 6-monthly follow-up visits.
Results: Among 89 MSM and 4 transgender women (median age 26 years), the anal HSIL incidence rate was 22.7 per 100 person-years over 180.9 person-years, while the clearance rate was 119.4 per 100 person-years over 32.7 person-years. After adjusting for age, smoking, and baseline CD4 + cell count, incident anal HSIL was greater in those with persistent HPV 16 [adjusted hazards ratio (aHR) 14.98, 95% confidence interval (CI) 1.73-129.48], nonpersistent HPV 16 (aHR 15.12, 95% CI 1.84-124.50), persistent non-16 cancer-associated HPV types (aHR 17.90, 95% CI 2.34-136.74), and nonpersistent non-16 cancer-associated HPV types (aHR 10.65, 95% CI 1.34-84.93) compared to participants with consistently negative cancer-associated HPV. Persistent (aHR 0.17, 95% CI 0.04-0.66) and nonpersistent HPV 16 (aHR 0.22, 95% CI 0.05-0.98) were associated with lower HSIL clearance likelihood.
Conclusion: Among predominantly young participants initiating antiretroviral therapy during acute HIV acquisition, anal HSIL showed high incidence yet markedly high clearance rates. Anal HPV 16 infection increased risk of incident anal HSIL and decreased lesion clearance. HPV vaccination and HSIL screening/treatment should be implemented despite rapid antiretroviral therapy initiation.
Keywords: HIV; antiretroviral therapy; human papillomavirus viruses; precancerous conditions; sexual and gender minorities.
Copyright © 2025 The Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
There are no conflicts of interest.
Figures

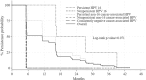
References
-
- Piketty C, Selinger-Leneman H, Grabar S, Duvivier C, Bonmarchand M, Abramowitz L, et al. Marked increase in the incidence of invasive anal cancer among HIV-infected patients despite treatment with combination antiretroviral therapy. AIDS 2008; 22:1203–1211. - PubMed
-
- Darragh TM, Colgan TJ, Cox JT, Heller DS, Henry MR, Luff RD, et al. The lower anogenital squamous terminology standardization project for HPV-associated lesions: background and consensus recommendations from the College of American Pathologists and the American Society for Colposcopy and Cervical Pathology. Arch Pathol Lab Med 2012; 136:1266–1297. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

