Adherence to plant based diets reduce the risk of hepatic fibrosis in nonalcoholic fatty liver disease
- PMID: 40389596
- PMCID: PMC12089538
- DOI: 10.1038/s41598-025-02613-8
Adherence to plant based diets reduce the risk of hepatic fibrosis in nonalcoholic fatty liver disease
Abstract
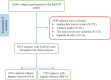
Adherence to plant-based diets has significantly increased in popularity recently, with claims that they reduce the risk of non-communicable diseases. This study investigated whether high adherence to plant-based diets can reduce the risk of hepatic steatosis and fibrosis. In this study, 8516 participants from the Ravansar Noncommunicable Disease cohort completed a validated food frequency questionnaire (FFQ) to assess their plant-based diet scores. The study used the fatty liver index and fibrosis-4 index to predict hepatic steatosis and fibrosis. The plant-based diet index (PDI) was used to measure the overall quality of diets from healthy and unhealthy plant-derived foods and animal-derived foods. Associations were determined using binary logistic regression, considering potential confounders. Participants in the highest tertiles of plant-based diet scores had higher energy-adjusted intakes of fructose than those in the lowest tertiles (16.09 ± 12.11 vs. 26.65 ± 12; P-value < 0.001). In multivariable-adjusted models, participants in the highest tertile of PDI had lower odds of hepatic fibrosis than those in the lowest tertile (OR: 0.59; 95%CI: 0.43-0.81). There was no significant association between adherence to PDI and hepatic steatosis after adjustment for potential confounders (OR: 0.989; 95%CI 0.78 - 1.25). The odds of hepatic fibrosis decreased by 6% for each unit increase in healthy plant-based foods (OR: 0.94; 95%CI: 0.91-0.97). The odds of hepatic steatosis increased by 14% for each 1 SD increase in fructose intake (OR: 1.14; 95% CI: 1.02-1.28). This study highlights the potential benefits of high adherence to plant-based diets in reducing the risk of hepatic fibrosis, but high fructose content in some plant-based foods may have an unfavorable role in hepatic steatosis. These findings highlight the importance of selecting whole, fiber-rich plant foods and minimizing intake of fructose-dense products in plant-based diets to promote liver health. Therefore, selecting low-fructose food items in plant-based diets is recommended, though further research is needed to confirm these findings.
Keywords: Fibrosis; Hepatic steatosis; NAFLD; Non-alcoholic fatty liver disease; Plant-Based diets.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Competing interests: The authors declare no competing interests. Consent for publication: Consent is available for publication. Ethics approval and consent to participate: The study was approved by the ethics committee of Kermanshah University of Medical Sciences (IR.KUMS.REC.1401.426). All methods were carried out by relevant guidelines and regulations. All the participants were provided oral and written informed consent. All methods were carried out according to relevant guidelines and regulations. This study was conducted by the Declaration of Helsinki. Ethics approval statement: The RaNCD cohort was conducted by the Declaration of Helsinki, and written informed consent was obtained from all participants. The current study was approved by the steering committee of the RaNCD and the ethics committee of Kermanshah University of Medical Sciences (IR.KUMS.REC.1402.403).
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical