Management and Outcomes of Umbilical Hernia in Decompensated Chronic Liver Disease: A Single-Unit Experience of Six Cases
- PMID: 40390754
- PMCID: PMC12087388
- DOI: 10.7759/cureus.82578
Management and Outcomes of Umbilical Hernia in Decompensated Chronic Liver Disease: A Single-Unit Experience of Six Cases
Abstract
Background Complicated umbilical hernia in decompensated chronic liver disease is a significant cause of morbidity and mortality. This study evaluates the management strategies and factors predicting outcomes following emergency umbilical hernia repair. Methods A retrospective analysis was conducted on six patients with decompensated chronic liver disease who presented with complicated umbilical hernia in an emergency setting to the hepatopancreatobiliary (HPB) surgical unit between July and December 2024. Preoperative characteristics, intraoperative findings, and postoperative outcomes were reviewed. Results A total of six patients were included. The mean age was 51.16 years (range: 44-58), and all presented with abdominal pain (6, 100%). Among them, two (33.3%) presented with a strangulated umbilical hernia, two (33.3%) with an obstructed hernia, and two (33.3%) with a ruptured hernia associated with ascites fluid leak. All patients (6, 100%), underwent emergency surgery. Bowel resection was required in three (50.0%) patients, of whom two (33.3%) underwent primary anastomosis and one (16.7%) underwent a double-barrelled ileostomy. All six (100%) patients underwent primary repair of the hernial defect without mesh placement. Postoperative recovery was uneventful in four (66.7%) patients; one (16.7%) patient developed an ascites fluid leak, and one (16.7%) died. The mean postoperative hospital stay was 14.83 days. Conclusion Emergency repair of complicated umbilical hernia in patients with decompensated chronic liver disease is associated with high morbidity and mortality. Contributing factors include increased ascites, portal hypertension, and liver decompensation following surgery. Preoperative optimization and intraoperative ascites drainage may play a crucial role in improving outcomes, even in emergency settings.
Keywords: decompensated chronic liver disease; emergency hernia repair; end-stage liver disease; transjugular intrahepatic portosystemic shunt; umbilical hernia.
Copyright © 2025, Singh et al.
Conflict of interest statement
Human subjects: Consent for treatment and open access publication was obtained or waived by all participants in this study. All India Institute of Medical Sciences, Rishikesh Institutional Ethics Committee issued approval AIIMS/RISH/GS/2025-246. Animal subjects: All authors have confirmed that this study did not involve animal subjects or tissue. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work.
Figures
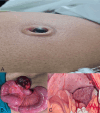
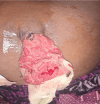
References
-
- Poor outcomes in cirrhosis-associated hernia repair: a nationwide cohort study of 32,033 patients. Carbonell AM, Wolfe LG, DeMaria EJ. Hernia. 2005;9:353–357. - PubMed
-
- Umbilical hernia repair in patients with signs of portal hypertension: surgical outcome and predictors of mortality. Cho SW, Bhayani N, Newell P, Cassera MA, Hammill CW, Wolf RF, Hansen PD. Arch Surg. 2012;147:864–869. - PubMed
-
- Management in patients with liver cirrhosis and an umbilical hernia. Marsman HA, Heisterkamp J, Halm JA, Tilanus HW, Metselaar HJ, Kazemier G. Surgery. 2007;142:372–375. - PubMed
-
- Umbilical herniorrhapy in cirrhosis: improved outcomes with elective repair. Gray SH, Vick CC, Graham LA, Finan KR, Neumayer LA, Hawn MT. J Gastrointest Surg. 2008;12:675–681. - PubMed
LinkOut - more resources
Full Text Sources
