The association of sepsis bundle compliance with mortality in patients with ICU-acquired sepsis: a cohort study
- PMID: 40394519
- PMCID: PMC12093641
- DOI: 10.1186/s12879-025-11134-8
The association of sepsis bundle compliance with mortality in patients with ICU-acquired sepsis: a cohort study
Abstract
Background: The efficacy of the SEP-1 Bundle has been questioned in the treatment of patients with hospital-acquired sepsis. We aimed to investigate bundle compliance and its association with survival in a subset of patients with HA sepsis: those with ICU-acquired sepsis.
Methods: A single-center retrospective cohort study was conducted in a tertiary care referral hospital. Adult patients diagnosed with ICU-acquired sepsis between 1 January 2019 and 31 December 2022 were identified. Survival to hospital discharge adjusted for disease severity based on 3-hour, 6-hour, and total bundle compliance was calculated. Secondary outcomes included the need for mechanical ventilation, vasopressors, initiation of acute hemodialysis, and discharge location.
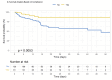
Results: Of 191 patients with ICU-acquired sepsis, 61 patients (31.9%) demonstrated total bundle compliance. There was no difference in survival based on the unadjusted analysis of 3-hour bundle compliance, compliant versus non-compliant (78.9% vs. 67.0%; P = 0.100). However, there was a survival benefit in 6-hour and total bundle, compliance versus non-compliance (82.2% vs. 60.0%, P < 0.001; 86.9% vs. 64.6%, P = 0.002). When adjusted for SOFA and CCI, logistic regression demonstrated similar results: 3-hour compliance (OR: 0.60; 95% CI: 0.29-1.18, P = 0.150), 6-hour compliance (OR: 0.35; 95% CI: 0.17-0.68, P = 0.002) and total compliance (OR: 0.31; 95% CI: 0.13-0.69, P = 0.006). Components of the SEP-1 Bundle that showed a mortality benefit included the collection of "blood cultures prior to antibiotic administration" (OR: 0.46; 95% CI 0.22-0.96, P = 0.037) and "tissue perfusion assessment" (OR: 0.41; 95% CI 0.18-0.90, P = 0.028).
Conclusions: Six-hour and total SEP-1 bundle compliance was associated with increased hospital survival in patients with ICU-acquired sepsis. These findings suggest the importance of sepsis bundle compliance in the ICU environment.
Clinical trial number: Not Applicable.
Keywords: ICU-acquired sepsis; Nosocomial sepsis; SEP-1 bundle; Sepsis; Sepsis bundle compliance.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethical approval: The study received ethical approval and was conducted in accordance with ethical standards. This study adhered to the Declaration of Helsinki. Cooper University Healthcare, IRB approval 22–292. Consent to participate: Given the study’s retrospective nature, consent to participate was waived per CUH IRB guidelines. Obtaining consent would have precluded the ability to complete the project. No unnecessary protected health information was collected and standard procedures to protect the information were taken. Consent for publication: NA. Competing interests: The authors declare no competing interests.
Figures
Similar articles
-
Evaluating the impact of severe sepsis 3-hour bundle compliance on 28-day in-hospital mortality: A propensity adjusted, nested case-control study.Pharmacotherapy. 2022 Aug;42(8):651-658. doi: 10.1002/phar.2715. Epub 2022 Jul 18. Pharmacotherapy. 2022. PMID: 35774011
-
Improvement in process of care and outcome after a multicenter severe sepsis educational program in Spain.JAMA. 2008 May 21;299(19):2294-303. doi: 10.1001/jama.299.19.2294. JAMA. 2008. PMID: 18492971
-
Hour-1 bundle adherence was associated with reduction of in-hospital mortality among patients with sepsis in Japan.PLoS One. 2022 Feb 14;17(2):e0263936. doi: 10.1371/journal.pone.0263936. eCollection 2022. PLoS One. 2022. PMID: 35157744 Free PMC article.
-
Antibiotic- and Fluid-Focused Bundles Potentially Improve Sepsis Management, but High-Quality Evidence Is Lacking for the Specificity Required in the Centers for Medicare and Medicaid Service's Sepsis Bundle (SEP-1).Crit Care Med. 2019 Oct;47(10):1290-1300. doi: 10.1097/CCM.0000000000003892. Crit Care Med. 2019. PMID: 31369426 Free PMC article.
-
The Surviving Sepsis Campaign: results of an international guideline-based performance improvement program targeting severe sepsis.Intensive Care Med. 2010 Feb;36(2):222-31. doi: 10.1007/s00134-009-1738-3. Epub 2010 Jan 13. Intensive Care Med. 2010. PMID: 20069275 Free PMC article. Review.
References
-
- Vincent JL, Marshall JC, Namendys-Silva SA, et al. Assessment of the worldwide burden of critical illness: the intensive care over nations (ICON) audit. Lancet Respir Med. 2014;2(5):380–6. - PubMed
-
- Evans L, Rhodes A, Alhazzani W, et al. Executive summary: surviving Sepsis campaign: international guidelines for the management of Sepsis and septic shock 2021. Crit Care Med. 2021;49(11):1974–82. - PubMed
-
- Prasad PA, Shea ER, Shiboski S, Sullivan MC, Gonzales R, Shimabukuro D. Relationship between a Sepsis intervention bundle and In-Hospital mortality among hospitalized patients: A retrospective analysis of Real-World data. Anesth Analg. 2017;125(2):507–13. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical