Research progress on osteoclast regulation by biodegradable magnesium and its mechanism
- PMID: 40395819
- PMCID: PMC12092085
- DOI: 10.1093/rb/rbaf026
Research progress on osteoclast regulation by biodegradable magnesium and its mechanism
Abstract
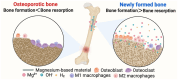
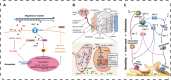
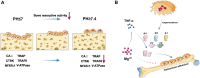
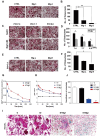
Continuous advancements in medical technology and biomaterials have underscored the significant advantages of biodegradable implant materials for bone repair and remodelling over traditional inert metallic implants. Notably, biodegradable magnesium-based materials have gained much attention because of their optimal corrosion rates. Importantly, extensive clinical experience has resulted in the use of biodegradable magnesium-based orthopaedic implants. Both preclinical and clinical studies have consistently demonstrated that Mg has an excellent ability to promote bone tissue formation, a process that is closely associated with the release of Mg2+ and other degradation byproducts. Bone metabolism depends on a dynamic balance of bone formation and bone resorption. Mg2+ has been shown to increase osteoblast (OB) activity while suppressing osteoclast (OC) formation, thus playing a crucial role in bone remodelling and regeneration. In terms of osteolysis inhibition, Mg2+ plays a multifaceted role. First, Mg2+ inhibits OC formation by modulating the activity of mature OCs, their migratory behaviour and the activity of precursor cells. Second, Mg2+ influences OC production by regulating the expression of osteoprotegerin (OPG), receptor activator of nuclear factor kappa-Β ligand (RANKL) and nuclear factor kappa-light-chain-enhancer of activated B cells (NF-κB). Additionally, Mg2+ impacts bone resorption by altering the immune microenvironment and the levels of hormones and peptides within the body. Furthermore, the alkaline environment generated around the biodegradable magnesium implant and its degradation products (e.g. H2) also significantly inhibit OC formation. Recent research on magnesium-based implants has focused predominantly on their osteogenic properties, with few systematic reviews addressing the mechanisms through which biodegradable magnesium alloys suppress osteoclastic activity. This article summarizes the latest clinical research progress concerning biodegradable magnesium implant materials and their significant regulatory effects and discusses recent advances in the understanding of the regulatory mechanisms of action Mg-based biomaterials on OCs, with the aim of providing a more theoretical basis for the clinical application of biodegradable magnesium-based implants.
Keywords: biodegradable magnesium alloys; bone remodelling; osteoblast; osteoclast; regulatory mechanisms.
© The Author(s) 2025. Published by Oxford University Press.
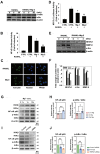
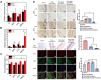
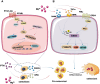
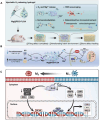
Figures


Similar articles
-
RNA interference-mediated osteoprotegerin silencing increases the receptor activator of nuclear factor-kappa B ligand/osteoprotegerin ratio and promotes osteoclastogenesis.World J Stem Cells. 2025 Apr 26;17(4):101290. doi: 10.4252/wjsc.v17.i4.101290. World J Stem Cells. 2025. PMID: 40308885 Free PMC article.
-
Dual modulation of bone formation and resorption with zoledronic acid-loaded biodegradable magnesium alloy implants improves osteoporotic fracture healing: An in vitro and in vivo study.Acta Biomater. 2018 Jan;65:486-500. doi: 10.1016/j.actbio.2017.10.033. Epub 2017 Oct 25. Acta Biomater. 2018. PMID: 29079514
-
Ion channel functional protein kinase TRPM7 regulates Mg ions to promote the osteoinduction of human osteoblast via PI3K pathway: In vitro simulation of the bone-repairing effect of Mg-based alloy implant.Acta Biomater. 2017 Nov;63:369-382. doi: 10.1016/j.actbio.2017.08.051. Epub 2017 Sep 4. Acta Biomater. 2017. PMID: 28882757
-
Biofunctionalisation of porous additively manufactured magnesium-based alloys for Orthopaedic applications: A review.Biomater Adv. 2025 Apr;169:214170. doi: 10.1016/j.bioadv.2024.214170. Epub 2025 Jan 2. Biomater Adv. 2025. PMID: 39793150 Review.
-
Biodegradable magnesium alloys as temporary orthopaedic implants: a review.Biometals. 2019 Apr;32(2):185-193. doi: 10.1007/s10534-019-00170-y. Epub 2019 Jan 18. Biometals. 2019. PMID: 30659451 Review.
References
-
- Zhang X, Zu H, Zhao D, Yang K, Tian S, Yu X, Lu F, Liu B, Yu X, Wang B, Wang W, Huang S, Wang Y, Wang Z, Zhang Z. Ion channel functional protein kinase TRPM7 regulates Mg ions to promote the osteoinduction of human osteoblast via PI3K pathway: in vitro simulation of the bone-repairing effect of Mg-based alloy implant. Acta Biomater 2017;63:369–82. - PubMed
-
- Zhang Y, Xu J, Ruan YC, Yu MK, O'Laughlin M, Wise H, Chen D, Tian L, Shi D, Wang J, Chen S, Feng JQ, Chow DH, Xie X, Zheng L, Huang L, Huang S, Leung K, Lu N, Zhao L, Li H, Zhao D, Guo X, Chan K, Witte F, Chan HC, Zheng Y, Qin L. Implant-derived magnesium induces local neuronal production of CGRP to improve bone-fracture healing in rats. Nat Med 2016;22:1160–9. - PMC - PubMed
-
- Qiao W, Wong KHM, Shen J, Wang W, Wu J, Li J, Lin Z, Chen Z, Matinlinna JP, Zheng Y, Wu S, Liu X, Lai KP, Chen Z, Lam YW, Cheung KMC, Yeung KWK. TRPM7 kinase-mediated immunomodulation in macrophage plays a central role in magnesium ion-induced bone regeneration. Nat Commun 2021;12:2885. - PMC - PubMed
-
- Plaass C, von Falck C, Ettinger S, Sonnow L, Calderone F, Weizbauer A, Reifenrath J, Claassen L, Waizy H, Daniilidis K, Stukenborg-Colsman C, Windhagen H. Bioabsorbable magnesium versus standard titanium compression screws for fixation of distal metatarsal osteotomies – 3 year results of a randomized clinical trial. J Orthop Sci 2018;23:321–7. - PubMed
-
- Lee JW, Han HS, Han KJ, Park J, Jeon H, Ok MR, Seok HK, Ahn JP, Lee KE, Lee DH, Yang SJ, Cho SY, Cha PR, Kwon H, Nam TH, Han JH, Rho HJ, Lee KS, Kim YC, Mantovani D. Long-term clinical study and multiscale analysis of in vivo biodegradation mechanism of Mg alloy. Proc Natl Acad Sci U S A 2016;113:716–21. - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

