Comparison of pancreaticojejunostomy under the theory of mucosal priority healing with duct-to-mucosa anastomosis and invagination pancreaticojejunostomy after pancreaticoduodenectomy: A single-centre case-control study
- PMID: 40397114
- PMCID: PMC12099170
- DOI: 10.1177/00368504251345016
Comparison of pancreaticojejunostomy under the theory of mucosal priority healing with duct-to-mucosa anastomosis and invagination pancreaticojejunostomy after pancreaticoduodenectomy: A single-centre case-control study
Abstract
ObjectiveThe technological aspects of pancreaticoduodenectomy have progressed greatly, but the risk of postoperative complications, especially postoperative pancreatic fistula (POPF), postpancreatectomy haemorrhage (PPH) and mortality, is high. Therefore, we aimed to explore the safety and feasibility of pancreaticojejunostomy (PJ) under the mucosal priority healing theory through a case-control study.MethodsWe have described in detail PJ under the theory of preferential mucosal healing (PM-PJ). In a cohort of patients based on predictors of pancreatic fistula, comparisons were made according to the type of PJ: PM-PJ (n = 312); duct-to-mucosa PJ (DtoM-PJ, n = 116); and invagination PJ (IPJ, n = 109). The primary endpoint was the occurrence of clinically relevant postoperative pancreatic fistula (CR-POPF). The secondary endpoints were PPH, secondary surgery, death 90 days after surgery, and other postoperative complications.ResultsThe incidence rate of CR-POPF in the PM-PJ group was not significantly different from that in the DtoM-PJ group (13.78% vs. 6.9%; p = 0.051) or the IPJ group (13.78% vs. 11.9%; p = 0.623). However, the PM-PJ group exhibited significant reductions in serious postoperative complications (7.4% versus 30.2%; p < 0.001), PPH (1.3% versus 8.4%; p < 0.001), reoperation rates (0.6% versus 9.3%; p < 0.001) and 90-day postoperative mortality rates (0.32% versus 2.6%; p = 0.023). Multivariate LASSO regression analysis revealed that BMI, hypertension, gland texture, duct size, vascular resection and pathological type were independent risk factors for CR-POPF.ConclusionsPM-PJ is safe and reliable. During surgery, there are fewer suture needles and less trauma, which may reduce the incidence of serious complications such as postoperative bleeding and mortality.
Keywords: Pancreaticojejunostomy; intestinal metaplasia; postoperative pancreatic fistula; postpancreatectomy haemorrhage; preferential mucosal healing.
Conflict of interest statement
Declaration of conflicting interestsThe authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
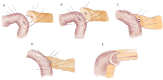

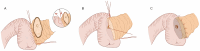

References
-
- Yamguchi T, Mori K, Kojima Y, et al. Joint research committee of Japanese society of oral care. Efficacy of perioperative oral care management in the prevention of surgical complications in 503 patients after pancreaticoduodenectomy for resectable malignant tumor: a multicenter retrospective analysis using propensity score matching. Surgery 2024; 175: 1128–1133. - PubMed
-
- Yasokawa K, Ito K, Tamada T, et al. Postprandial changes in secretory flow of pancreatic juice in the main pancreatic duct: evaluation with cine-dynamic MRCP with a spatially selective inversion-recovery (IR) pulse. Eur Radiol 2016; 26: 4339–4344. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

