Renal-Cardiac Crosstalk in the Pathogenesis and Progression of Heart Failure
- PMID: 40403103
- PMCID: PMC12105978
- DOI: 10.1161/CIRCRESAHA.124.325488
Renal-Cardiac Crosstalk in the Pathogenesis and Progression of Heart Failure
Abstract
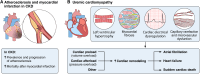
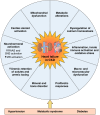
Chronic kidney disease (CKD) represents a global health issue with a high socioeconomic impact. Beyond a progressive decline of kidney function, patients with CKD are at increased risk of cardiovascular diseases, including heart failure (HF) and sudden cardiac death. HF in CKD can manifest both as HF with reduced ejection fraction and HF with preserved ejection fraction, with the latter further increasing in relative importance in the more advanced stages of CKD. Typical cardiac remodeling characteristics in uremic cardiomyopathy include left ventricular hypertrophy, myocardial fibrosis, cardiac electrical dysregulation, capillary rarefaction, and microvascular dysfunction, which are triggered by increased cardiac preload, cardiac afterload, and preload and afterload-independent factors. The pathophysiological mechanisms underlying cardiac remodeling in CKD are multifactorial and include neurohormonal activation (with increased activation of the renin-angiotensin-aldosterone system, the sympathetic nervous system, and mineralocorticoid receptor signaling), cardiac steroid activation, mitochondrial dysfunction, inflammation, innate immune activation, and oxidative stress. Furthermore, disturbances in cardiac metabolism and calcium homeostasis, macrovascular and microvascular dysfunction, increased cellular profibrotic responses, the accumulation of uremic retention solutes, and mineral and bone disorders also contribute to cardiovascular disease and HF in CKD. Here, we review the current knowledge of HF in CKD, including the clinical characteristics and pathophysiological mechanisms revealed in animal studies. We also elaborate on the detrimental impact of comorbidities of CKD on HF using hypertension as an example and discuss the clinical characteristics of hypertensive heart disease and the genetic predisposition. Overall, this review aims to increase the understanding of HF in CKD to support future research and clinical translational approaches for improved diagnosis and therapy of this vulnerable patient population.
Keywords: cardiovascular diseases; heart failure; hypertension; inflammation; metabolism.
Conflict of interest statement
J. Jankowski has given lectures for Bayer and Fresenius Medical Care. In addition, he holds 4 patents on the topic of the article and is the inventor of an additional, already-sold patent to Baxter. N. Marx has given lectures for Bayer, Boehringer Ingelheim, Sanofi-Aventis, MSD (Merck Sharp and Dohme), Bristol Myers Squibb (BMS), AstraZeneca, Lilly, and Novo Nordisk; has received unrestricted research grants from Boehringer Ingelheim; and has served as an advisor for Bayer, Boehringer Ingelheim, Sanofi-Aventis, MSD, BMS, AstraZeneca, and Novo Nordisk. In addition, he served in trial leadership for Boehringer Ingelheim and Novo Nordisk. N. Marx declines all personal compensation from pharma or device companies. The other authors report no conflicts.
Figures

Similar articles
-
Systemic aging fuels heart failure: Molecular mechanisms and therapeutic avenues.ESC Heart Fail. 2025 Apr;12(2):1059-1080. doi: 10.1002/ehf2.14947. Epub 2024 Jul 22. ESC Heart Fail. 2025. PMID: 39034866 Free PMC article. Review.
-
Pro-oxidative priming but maintained cardiac function in a broad spectrum of murine models of chronic kidney disease.Redox Biol. 2022 Oct;56:102459. doi: 10.1016/j.redox.2022.102459. Epub 2022 Aug 30. Redox Biol. 2022. PMID: 36099852 Free PMC article.
-
Heart failure and kidney dysfunction: epidemiology, mechanisms and management.Nat Rev Nephrol. 2016 Oct;12(10):610-23. doi: 10.1038/nrneph.2016.113. Epub 2016 Aug 30. Nat Rev Nephrol. 2016. PMID: 27573728 Review.
-
Renin-angiotensin system inhibitors for patients with mild or moderate chronic kidney disease and heart failure with mildly reduced or preserved ejection fraction.Int J Cardiol. 2024 Aug 15;409:132190. doi: 10.1016/j.ijcard.2024.132190. Epub 2024 May 16. Int J Cardiol. 2024. PMID: 38761975
-
Soluble Flt-1 links microvascular disease with heart failure in CKD.Basic Res Cardiol. 2015 May;110(3):30. doi: 10.1007/s00395-015-0487-4. Epub 2015 Apr 21. Basic Res Cardiol. 2015. PMID: 25893874
Cited by
-
CARDIAL-MS (CArdio-Renal-DIAbetes-Liver-Metabolic Syndrome): a new proposition for an integrated multisystem metabolic disease.Diabetol Metab Syndr. 2025 Jun 16;17(1):218. doi: 10.1186/s13098-025-01796-4. Diabetol Metab Syndr. 2025. PMID: 40524210 Free PMC article. Review.
-
Interorgan Crosstalk in Heart Failure and Cardiometabolic Diseases: A Compendium.Circ Res. 2025 May 23;136(11):1167-1169. doi: 10.1161/CIRCRESAHA.125.326720. Epub 2025 May 22. Circ Res. 2025. PMID: 40403104 Review. No abstract available.
References
-
- Jager KJ, Kovesdy C, Langham R, Rosenberg M, Jha V, Zoccali C. A single number for advocacy and communication-worldwide more than 850 million individuals have kidney diseases. Kidney Int. 2019;96:1048–1050. doi: 10.1016/j.kint.2019.07.012 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

