Fecal microbiota transplantation from a healthy pouch donor for chronic pouchitis: a proof-of-concept study
- PMID: 40413728
- PMCID: PMC12118383
- DOI: 10.1080/19490976.2025.2510464
Fecal microbiota transplantation from a healthy pouch donor for chronic pouchitis: a proof-of-concept study
Abstract
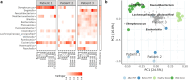
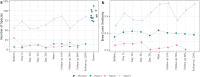
Chronic pouchitis is a common complication after ileal pouch-anal anastomosis (IPAA) with limited treatment options. In this case series, we aimed to investigate clinical and microbiome changes, as well as adverse events, associated with using fecal microbiota transplantation (FMT) from a donor with a normal functioning IPAA to induce remission in patients with chronic pouchitis. Methods The study was a case-series including a 4-week intervention period and 12-month follow-up. Patients with chronic pouchitis who met the inclusion criteria were recruited from the Department of Gastrointestinal Surgery at Aalborg University Hospital, Denmark. Participants received FMT derived from a donor with a normal functioning IPAA. Treatment was administered by enema daily for two weeks, then every other day for two more weeks. Disease severity and quality of life (QoL) were accessed at baseline and 30-day follow-up. Clinical remission was defined as Pouchitis Disease Activity Index (PDAI) <7. Fecal samples from participants, healthy donors, and the IPAA donor were analyzed using shotgun metagenomic sequencing. Results Three patients with chronic pouchitis were included and completed the treatment protocol and follow-up visits. At the 30-day follow-up, all participants achieved clinical remission with reduced endoscopic inflammation. The median total PDAI score decreased from 8 (range 10-8) at baseline to 6 (range 6-5) at 30 days. Two participants reported improved QoL, while one reported no change. Few mild, self-limited adverse events were reported by all participants during treatment, with no serious events. Principal component analysis of fecal samples distinguished two clusters: healthy donors and the IPAA donor, with participant samples forming a separate cluster Conclusion We observed that all participants achieved clinical remission with reduced endoscopic inflammation following a 4-week FMT intervention. Adverse events were mild and self-limited. Metagenomic analysis revealed distinct microbiome clusters between IPAA donor and recipients, both of which differed from those of healthy donors.
Keywords: IPAA; Pouchitis; fecal microbiota transplantation; metagenomics; microbiome.
Conflict of interest statement
No potential conflict of interest was reported by the author(s).
Figures
References
-
- Shen B, Kochhar GS, Rubin DT, Kane SV, Navaneethan U, Bernstein CN, Cross RK, Sugita A, Schairer J, Kiran RP, et al. Treatment of pouchitis, Crohn’s disease, cuffitis, and other inflammatory disorders of the pouch: consensus guidelines from the international ileal pouch consortium. Lancet Gastroenterol Hepatol. 2021;7(1):69–95. doi: 10.1016/S2468-1253(21)00214-4. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous
