Clinical, radiological, and radiomics feature-based explainable machine learning models for prediction of neurological deterioration and 90-day outcomes in mild intracerebral hemorrhage
- PMID: 40420050
- PMCID: PMC12105149
- DOI: 10.1186/s12880-025-01717-x
Clinical, radiological, and radiomics feature-based explainable machine learning models for prediction of neurological deterioration and 90-day outcomes in mild intracerebral hemorrhage
Abstract
Background: The risks and prognosis of mild intracerebral hemorrhage (ICH) patients were easily overlooked by clinicians. Our goal was to use machine learning (ML) methods to predict mild ICH patients' neurological deterioration (ND) and 90-day prognosis.
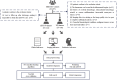
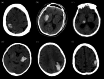
Methods: This prospective study recruited 257 patients with mild ICH for this study. After exclusions, 148 patients were included in the ND study and 144 patients in the 90-day prognosis study. We trained five ML models using filtered data, including clinical, traditional imaging, and radiomics indicators based on non-contrast computed tomography (NCCT). Additionally, we incorporated the Shapley Additive Explanation (SHAP) method to display key features and visualize the decision-making process of the model for each individual.
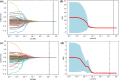
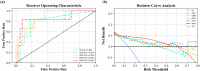
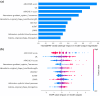
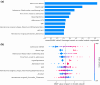
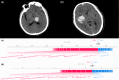
Results: A total of 21 (14.2%) mild ICH patients developed ND, and 35 (24.3%) mild ICH patients had a 90-day poor prognosis. In the validation set, the support vector machine (SVM) models achieved an AUC of 0.846 (95% confidence intervals (CI), 0.627-1.000) and an F1-score of 0.667 for predicting ND, and an AUC of 0.970 (95% CI, 0.928-1.000), and an F1-score of 0.846 for predicting 90-day prognosis. The SHAP analysis results indicated that several clinical features, the island sign, and the radiomics features of the hematoma were of significant value in predicting ND and 90-day prognosis.
Conclusion: The ML models, constructed using clinical, traditional imaging, and radiomics indicators, demonstrated good classification performance in predicting ND and 90-day prognosis in patients with mild ICH, and have the potential to serve as an effective tool in clinical practice.
Clinical trial number: Not applicable.
Keywords: Computed tomography; Intracerebral hemorrhage; Machine learning; Modified rankin scale; Neurological deterioration; Radiomics.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethical approval: This prospective study has obtained approval from the Medical Ethics Committee of Nanfang Hospital (approval number: NFEC-2022-168). All study protocols and procedures were conducted in accordance with the Declaration of Helsinki. Consent for publication: Not applicable. Informed consent: All participants provided written consent before participating in the study. Competing interests: The authors declare no competing interests.
Figures

Similar articles
-
An interpretable artificial intelligence model based on CT for prognosis of intracerebral hemorrhage: a multicenter study.BMC Med Imaging. 2024 Jul 9;24(1):170. doi: 10.1186/s12880-024-01352-y. BMC Med Imaging. 2024. PMID: 38982357 Free PMC article.
-
Quantitative imaging for predicting hematoma expansion in intracerebral hemorrhage: A multimodel comparison.J Stroke Cerebrovasc Dis. 2024 Jul;33(7):107731. doi: 10.1016/j.jstrokecerebrovasdis.2024.107731. Epub 2024 Apr 23. J Stroke Cerebrovasc Dis. 2024. PMID: 38657831
-
A Radiomics Model Based on CT Images Combined with Multiple Machine Learning Models to Predict the Prognosis of Spontaneous Intracerebral Hemorrhage.World Neurosurg. 2024 Jan;181:e856-e866. doi: 10.1016/j.wneu.2023.11.002. Epub 2023 Nov 4. World Neurosurg. 2024. PMID: 37931880
-
Prognostic value of CT scan-based radiomics in intracerebral hemorrhage patients: A systematic review and meta-analysis.Eur J Radiol. 2024 Sep;178:111652. doi: 10.1016/j.ejrad.2024.111652. Epub 2024 Jul 26. Eur J Radiol. 2024. PMID: 39079323
-
Machine learning for predicting hematoma expansion in spontaneous intracerebral hemorrhage: a systematic review and meta-analysis.Neuroradiology. 2024 Sep;66(9):1603-1616. doi: 10.1007/s00234-024-03399-8. Epub 2024 Jun 12. Neuroradiology. 2024. PMID: 38862772
References
-
- You S, Zheng D, Delcourt C, et al. Determinants of early versus delayed neurological deterioration in intracerebral hemorrhage. Stroke. 2019;50:1409–14. - PubMed
-
- Davis SM, Broderick J, Hennerici M, et al. Hematoma growth is a determinant of mortality and poor outcome after intracerebral hemorrhage. Neurology. 2006;66:1175–81. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

