Stability of maxilla after segmental Le Fort I osteotomy combined with anterior maxilla clockwise rotation in patients with maxillary hypoplasia: a retrospective study
- PMID: 40426151
- PMCID: PMC12107807
- DOI: 10.1186/s12903-025-06057-4
Stability of maxilla after segmental Le Fort I osteotomy combined with anterior maxilla clockwise rotation in patients with maxillary hypoplasia: a retrospective study
Abstract
Background: Segmental Le Fort I osteotomy combined with anterior maxillary clockwise rotation has been proposed as an effective treatment for maxillary hypoplasia. However, the stability of maxilla after the operation remains unknown.
Methods: A total of 30 patients undergoing segmental Le Fort I osteotomy were retrospectively included. The follow-up period was more than one year. The stability of anterior maxilla after clockwise rotation was evaluated by cone beam computed tomography (CBCT) performed before surgery (T0), three days after surgery (T1), and at least one year after surgery (T2), respectively. The key parameters were the postoperative relapse of the anterior maxillary clockwise rotation angle (CRA) and paranasal advancement.
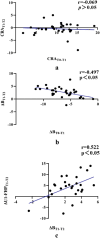
Results: Following segmental Le Fort I osteotomy, the average CRA of the anterior maxilla was 10.02° ± 3.86°, while the mean paranasal advancement was 6.22 ± 1.40 mm. At the one-year follow-up, the relapse of CRA and paranasal advancement were -0.42° ± 2.51° (p = 0.951) and -0.28 ± 0.83 mm (p = 0.08), respectively, suggesting good postoperative stability. Additionally, no significant correlation was found between the intraoperative CRA and its relapse over time.
Conclusion: Segmental Le Fort I osteotomy combined with anterior maxillary clockwise rotation demonstrates favorable stability up to one year postoperatively, making it a reliable approach for the treatment of maxillary hypoplasia.
Keywords: Anterior maxillary clockwise rotation; Maxillary hypoplasia; Segmental Le Fort I osteotomy; Stability.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study was approved by the Institutional Review Board of the Stomatology School of Peking University (PKUSSIRB202278111) and performed in accordance with the 1964 Helsinki Declaration and its later amendment. The informed consent was obtained from all subjects or if subjects were under 18, from a parent and/or legal guardian. Consent for publication: Written informed consent was obtained from the individuals for the publication of any potentially identifiable images or data included in this article. Competing interests: The authors declare no competing interests.
Figures



References
-
- Gill FBNDS. Orthognathic surgery: principles, planning and practice. New York: John Wiley & Sons Ltd.; 2017.
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

