Differential Characteristics and Outcomes of Urgent/Emergent Versus Elective Aortic Valve Replacement
- PMID: 40439170
- PMCID: PMC12229216
- DOI: 10.1161/JAHA.125.041148
Differential Characteristics and Outcomes of Urgent/Emergent Versus Elective Aortic Valve Replacement
Abstract
Background: Despite the slowly progressive nature of aortic stenosis, a proportion of aortic valve replacements (AVRs) still occur on an urgent/emergent basis. We sought to characterize the predictors, outcomes, and potential opportunities to prevent urgent/emergent AVRs.
Methods: We analyzed Medicare data to identify patients undergoing AVRs from 2017 to 2022. We used multivariable regression to identify factors associated with nonelective AVRs; we also examined the association of nonelective AVRs with clinical outcomes and health care costs.
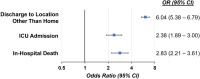
Results: In total, 15 305 patients (16% urgent/emergent) underwent AVR during the study period. Compared with patients undergoing elective AVRs, those receiving urgent/emergent AVRs were more frequently of Black race or Hispanic ethnicity, and less likely to have received a diagnosis of aortic stenosis, despite 91.7% having seen a cardiologist or primary care provider in the prior year. In multivariable-adjusted analyses, dual Medicare-Medicaid enrollment, male sex, and recent heart failure hospitalization were associated with increased risk for urgent/emergent AVR; conversely, recent aortic stenosis diagnosis and cardiologist visit were associated with lower odds of urgent/emergent AVR. In turn, urgent/emergent compared with elective AVR increased risk for in-hospital death, intensive care unit admission, and discharge to a facility versus home, in addition to longer lengths of stay and higher health care costs.
Conclusions: Urgent/emergent AVR occurs more frequently among Black, Hispanic, and dual Medicare-Medicaid-eligible patients. Nonelective AVR is also associated with worse hospital outcomes as well as greater health care costs. Importantly, variable timing in diagnosis of aortic stenosis appears to be a key determinant; thus, augmented screening efforts may improve outcomes and reduce disparities.
Keywords: Medicare; aortic valve replacement; cardiovascular outcomes; disparities.
Conflict of interest statement
Drs Kelley and Thompson and M. Platanis are Edwards Lifesciences employees. Dr Ebinger has served as a consultant and received grant funding from Edwards Lifesciences. All other authors report no relevant potential conflicts.
Figures

Similar articles
-
Elective THA for Indications Other Than Osteoarthritis Is Associated With Increased Cost and Resource Use: A Medicare Database Study of 135,194 Claims.Clin Orthop Relat Res. 2024 Jul 1;482(7):1159-1170. doi: 10.1097/CORR.0000000000002922. Epub 2023 Nov 24. Clin Orthop Relat Res. 2024. PMID: 38011034 Free PMC article.
-
Limited versus full sternotomy for aortic valve replacement.Cochrane Database Syst Rev. 2017 Apr 10;4(4):CD011793. doi: 10.1002/14651858.CD011793.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2023 Dec 6;12:CD011793. doi: 10.1002/14651858.CD011793.pub3. PMID: 28394022 Free PMC article. Updated.
-
Trends in Transcatheter and Surgical Aortic Valve Replacement Among Older Adults in the United States.J Am Coll Cardiol. 2021 Nov 30;78(22):2161-2172. doi: 10.1016/j.jacc.2021.09.855. J Am Coll Cardiol. 2021. PMID: 34823659
-
Treatment disparities and prognostic implications in octogenarians versus non-octogenarians with high-gradient severe aortic stenosis.Open Heart. 2025 Aug 14;12(2):e003405. doi: 10.1136/openhrt-2025-003405. Open Heart. 2025. PMID: 40813105 Free PMC article.
-
Limited versus full sternotomy for aortic valve replacement.Cochrane Database Syst Rev. 2023 Dec 6;12(12):CD011793. doi: 10.1002/14651858.CD011793.pub3. Cochrane Database Syst Rev. 2023. PMID: 38054555 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

