Divergent ventilatory responses during opioid-induced respiratory depression in response to repeated fentanyl use
- PMID: 40455004
- PMCID: PMC12312535
- DOI: 10.1152/ajplung.00302.2024
Divergent ventilatory responses during opioid-induced respiratory depression in response to repeated fentanyl use
Abstract
Opioid-induced respiratory depression (OIRD) is the hallmark of opioid overdose and a major risk factor for death due to fentanyl use. Although repeat opioid use (ROU) elevates the risk of death, understanding its influence over breathing and its control has been poorly resolved. We developed a mouse model of recurrent fentanyl use over 5 days to examine how ROU impacts breathing and activity from the pre-Bötzinger complex (preBötC), the brainstem network driving inspiratory rhythmogenesis. Initial fentanyl use caused a profound metabolic crisis during OIRD involving a mismatch between ventilation and oxygen consumption. By day 5 of ROU, 77% of mice exhibited an adaptive ventilatory response following ROU, which was accompanied by an improved relationship between ventilation and oxygen consumption during OIRD. However, in the remaining minority, the adaptive response during OIRD failed to emerge following ROU. This divergence emphasizes the heterogeneity in ventilatory and metabolic outcomes following ROU. Moreover, following ROU, rhythmogenesis in the preBötzinger complex was less sensitive to mu-opioid receptor agonism, indicating that adaptation to ROU involves centrally mediated changes in this brainstem network. These findings reveal a series of physiological changes following ROU, typically resulting in improved ventilation and oxygenation during OIRD. Such changes, or lack of thereof, may contribute to the unpredictable nature of overdose susceptibility among opioid users.NEW & NOTEWORTHY Recurring fentanyl use is a significant factor contributing to opioid-related deaths, yet the physiological impact of repeat opioid use on breathing remains poorly understood. This study demonstrates that divergent ventilatory responses to opioids emerge following repeated fentanyl administration. These responses coincide with changes in oxygen consumption and inspiratory rhythmogenesis from the preBötzinger complex. These observations advance an understanding of the physiological basis for susceptibility and tolerance among individuals likely to succumb to opioid overdose.
Keywords: fentanyl; opioid use disorder; oxygen metabolism; preBötzinger complex; respiratory depression.
Conflict of interest statement
Figures



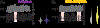
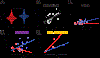

Similar articles
-
Functional modulation of retrotrapezoid neurons drives fentanyl-induced respiratory depression.Am J Physiol Lung Cell Mol Physiol. 2025 Sep 1;329(3):L357-L375. doi: 10.1152/ajplung.00025.2025. Epub 2025 Jul 22. Am J Physiol Lung Cell Mol Physiol. 2025. PMID: 40695580
-
Peripheral opioid receptor antagonism alleviates fentanyl-induced cardiorespiratory depression and is devoid of aversive behavior.Elife. 2025 Apr 1;13:RP104469. doi: 10.7554/eLife.104469. Elife. 2025. PMID: 40167443 Free PMC article.
-
Reversal of morphine-induced respiratory depression with the µ1-opioid receptor antagonist naloxonazine engenders excitation and instability of breathing.Am J Physiol Lung Cell Mol Physiol. 2025 Jul 1;329(1):L97-L111. doi: 10.1152/ajplung.00045.2025. Epub 2025 May 14. Am J Physiol Lung Cell Mol Physiol. 2025. PMID: 40366705 Free PMC article.
-
Impact of morphine, fentanyl, oxycodone or codeine on patient consciousness, appetite and thirst when used to treat cancer pain.Cochrane Database Syst Rev. 2014 May 29;2014(5):CD011056. doi: 10.1002/14651858.CD011056.pub2. Cochrane Database Syst Rev. 2014. PMID: 24874470 Free PMC article.
-
The Black Book of Psychotropic Dosing and Monitoring.Psychopharmacol Bull. 2024 Jul 8;54(3):8-59. Psychopharmacol Bull. 2024. PMID: 38993656 Free PMC article. Review.
References
-
- Dahan A, et al. , Pharmacovigilance: a review of opioid-induced respiratory depression in chronic pain patients. Pain Physician, 2013. 16(2): p. E85–94. - PubMed
-
- Hoffman JR, Schriger DL, and Luo JS, The empiric use of naloxone in patients with altered mental status: a reappraisal. Ann Emerg Med, 1991. 20(3): p. 246–52. - PubMed
-
- Darke S and Zador D, Fatal heroin ‘overdose’: a review. Addiction, 1996. 91(12): p. 1765–72. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

