Asymptomatic sigmoid diverticulum perforation-induced subcutaneous, mediastinal, and retroperitoneal emphysema: A case report and literature review
- PMID: 40476087
- PMCID: PMC12138572
- DOI: 10.1016/j.rmcr.2025.102229
Asymptomatic sigmoid diverticulum perforation-induced subcutaneous, mediastinal, and retroperitoneal emphysema: A case report and literature review
Abstract
Background: Mediastinal and subcutaneous emphysema usually result from spontaneous rupture of the alveolar wall. We present an educational case of subcutaneous, mediastinal, and retroperitoneal emphysema discovered during a routine medical check-up resulting from an asymptomatic perforation of the sigmoid diverticulum.
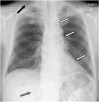
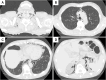
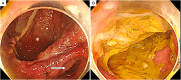
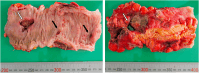
Case presentation: A 66-year-old man presented to our hospital for his health check-up. A chest X-ray revealed mediastinal emphysema during a physical examination. The patient had no subjective symptoms, fever, or hemodynamic instability. Physical examination revealed a snow grip sensation in the anterior neck but no abdominal tenderness. Blood tests showed an elevated inflammatory response, and a plain chest computed tomography scan revealed subcutaneous emphysema around the neck, as well as mediastinal and retroperitoneal emphysema. The patient was then admitted to the hospital and the patient was treated conservatively. On Day 7 post-admission, the emphysema was mildly relieved. However, on Day 10, the patient developed intestinal obstruction caused by barium. Colonoscopy revealed sigmoid colon perforation. On Day 11, partial resection of the sigmoid colon via laparotomy and colostomy (Hartmann operation) was performed. Postoperative pathology revealed a perforation of the sigmoid colon, which was confirmed to be induced by diverticulitis, as multiple diverticula were simultaneously found in the sigmoid colon.
Conclusions: Even in the absence of abdominal symptoms, retroperitoneal emphysema may develop due to perforation of the sigmoid colon. Therefore, if retroperitoneal emphysema is combined with mediastinal emphysema, evaluation, including abdominal CT, should be performed to identify the cause of emphysema.
Keywords: Mediastinal emphysema; Perforation of sigmoid diverticulum; Retroperitoneal emphysema; Subcutaneous emphysema.
© 2025 The Authors. Published by Elsevier Ltd.
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures
References
-
- Maunder R.J., Pierson D.J., Hudson L.D. Subcutaneous and mediastinal emphysema. Pathophysiology, diagnosis, and management. Arch. Intern. Med. 1984;144:1447–1453. - PubMed
-
- Macklin C.C. Transport of air along sheathes of pulmonic blood vessels from alveoli to mediastinum clinical implications. Arch lntern Med. 1939;64:913–926.
Publication types
LinkOut - more resources
Full Text Sources

