Transforaminal Percutaneous Endoscopic Discectomy for L3/4 and L4/5 Foraminal and Extraforaminal Lumbar Disc Herniation: Clinical Outcomes and Technical Note
- PMID: 40485789
- PMCID: PMC12136954
- DOI: 10.1055/s-0045-1805018
Transforaminal Percutaneous Endoscopic Discectomy for L3/4 and L4/5 Foraminal and Extraforaminal Lumbar Disc Herniation: Clinical Outcomes and Technical Note
Abstract
Study design: Retrospective cohort study.
Background: Foraminal and extraforaminal disc herniations account for 7 to 12% of lumbar herniated discs. Various surgical methods, including midline approaches with facetectomy and paramedian techniques, involve significant bone removal, risking spinal instability. The percutaneous transforaminal approach for endoscopic access to lateral disc herniations presents several advantages over traditional techniques and may be more suitable for these cases.
Objectives: This article evaluates the clinical outcomes and potential complications associated with the treatment of foraminal and extraforaminal lumbar disc herniations at the L3/4 and L4/5 levels in patients who have undergone transforaminal percutaneous endoscopic lumbar discectomy.
Materials and methods: Between 2016 and 2020, a total of 32 patients diagnosed with single-level lumbar disc herniation at the L3/4 or L4/5 foraminal or extraforaminal levels, who had not responded to conservative management, underwent transforaminal endoscopic discectomy. Follow-up evaluations were performed on postoperative day 1 and at 2 weeks, 6 weeks, 3 months, and 12 months. Both pre- and postoperative assessments employed the visual analog scale (VAS) and the Oswestry Disability Index (ODI) to quantify pain levels and functional outcomes. Clinical outcomes were assessed according to the MacNab criteria to determine the efficacy of the surgical intervention.
Results: The average age of patients was 52.6 years, with L4/5 (81.3%) and L3/4 (18.7%) being the most affected levels. The median follow-up was 18.2 months (range, 1-44 months). There was a significant reduction in VAS and ODI scores at follow-ups compared to preoperative levels ( p < 0.01). All patients with preoperative neurological deficits improved, though six patients (18.7%) experienced transient dysesthesia that resolved in 6 weeks. Per the MacNab criteria, clinical efficacy was excellent in 56.3% of patients, good in 37.5%, and fair in 6.2%.
Conclusion: Transforaminal endoscopic lumbar discectomy is a safe and effective minimally invasive procedure for foraminal and extraforaminal lumbar disc herniations at the L3/4 and L4/5 levels. It preserves spinal stability, minimizes blood loss, reduces postoperative pain, and allows for quicker recovery, presenting a strong alternative for patients needing surgery for these conditions.
Keywords: far lateral lumbar disc herniation; foraminal lumbar disc herniation; transforaminal endoscopic discectomy.
Asian Congress of Neurological Surgeons. This is an open access article published by Thieme under the terms of the Creative Commons Attribution-NonDerivative-NonCommercial License, permitting copying and reproduction so long as the original work is given appropriate credit. Contents may not be used for commercial purposes, or adapted, remixed, transformed or built upon. ( https://creativecommons.org/licenses/by-nc-nd/4.0/ ).
Conflict of interest statement
Conflict of Interest None declared.
Figures

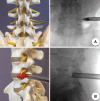
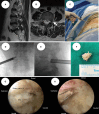
References
-
- Abdullah A F, Ditto E W, III, Byrd E B, Williams R. Extreme-lateral lumbar disc herniations. Clinical syndrome and special problems of diagnosis. J Neurosurg. 1974;41(02):229–234. - PubMed
-
- O'Hara L J, Marshall R W. Far lateral lumbar disc herniation. The key to the intertransverse approach. J Bone Joint Surg Br. 1997;79(06):943–947. - PubMed
-
- Darden B V, II, Wade J F, Alexander R, Wood K E, Rhyne A L, III, Hicks J R. Far lateral disc herniations treated by microscopic fragment excision. Techniques and results. Spine. 1995;20(13):1500–1505. - PubMed
-
- Epstein N E. Different surgical approaches to far lateral lumbar disc herniations. J Spinal Disords. 1995;8:383–394. - PubMed
-
- Garrido E, Connaughton P N. Unilateral facetectomy approach for lateral lumbar disc herniation. J Neurosurg. 1991;74(05):754–756. - PubMed
LinkOut - more resources
Full Text Sources

