Intraorbital arteriovenous fistulas: illustrative case
- PMID: 40489957
- PMCID: PMC12147662
- DOI: 10.3171/CASE24857
Intraorbital arteriovenous fistulas: illustrative case
Abstract
Background: Intraorbital arteriovenous fistulas (ioAVFs) represent a rare but distinct entity of arteriovenous shunts, separate from the more common carotid-cavernous fistulas (CCFs). There is currently no consensus on the optimal treatment approach for ioAVFs, necessitating analysis of available cases to guide clinical decision-making and establish effective management strategies.
Observations: A systematic literature review revealed a total of 28 ioAVF cases reported since 1978. An additional illustrative case is included. Intraorbital AVFs present with similar symptoms as the CCFs such as skin changes (chemosis, ecchymosis, erythema; 86.2%), proptosis (72.4%), and headaches (34.5%). Visual impairment was observed in 12 cases (41.4%); ophthalmoplegia occurred in 8 cases (27.6%). Five patients (17.2%) presented with an afferent pupillary defect. All patients underwent catheter angiography for their diagnostic workup. The ophthalmic artery (OA) was a direct feeder to the fistula in almost all patients (96.6%). Additional feeding vessels included the facial artery, sphenopalatine artery, middle meningeal artery, internal maxillary artery, and superficial temporal artery. Venous drainage was mainly via the superior ophthalmic vein (SOV). Other draining veins involved the inferior ophthalmic vein, facial vein, superior temporal vein, basal vein of Rosenthal, and superior sagittal sinus. Spontaneous resolution occurred in 5 cases (< 20%). Treatment was reported in 21 cases and included embolization (66.7%), resection (14.3%), or combined techniques (19.0%). Embolization was performed most often transvenously (14 cases). Three cases were embolized via direct puncture. A transarterial approach was selected in 6 cases. The OA was embolized directly (distal to the central retinal artery) in 2 cases, including the illustrative case. The average follow-up was 7.8 months (range 3 days-3 years). Overall, treatment was successful with a high cure rate (85.7%). Complications included extensive hemorrhage during transvenous embolization in 1 case and profound thrombosis of the SOV in 2 cases.
Lessons: Intraorbital AVFs are characterized by direct inflow via the OA. Treatment can be challenging. A multimodal approach, including observation, can result in high cure rates. Transvenous embolization is the most commonly performed intervention. Embolization via the OA is an option, but carries the risk of permanent visual deficit. https://thejns.org/doi/10.3171/CASE24857.
Keywords: arteriovenous fistulas; case report; endovascular embolization; orbit.
Figures

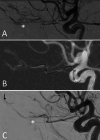
References
-
- Barrow DL Spector RH Braun IF Landman JA Tindall SC Tindall GT.. Classification and treatment of spontaneous carotid-cavernous sinus fistulas. J Neurosurg. 1985;62(2):248-256. - PubMed
-
- Machiele R Motlagh M Zeppieri M Patel BC.. Intraocular pressure. In: StatPearls [Internet]. StatPearls Publishing; 2024. - PubMed
-
- Rengachary SS Kishore PR.. Intraorbital ophthalmic aneurysms and arteriovenous fistulae. Surg Neurol. 1978;9(1):35-41. - PubMed
-
- Freitas MA Filho CA Lima R Marchiori E.. Traumatic ophthalmic fistula simulating carotid-cavernous fistula. Neurosurgery. 1983;12(1):102-104. - PubMed
-
- Tabuse J Tane K Ohta T Iwata T.. Traumatic ophthalmic artery-superior ophthalmic vein fistula: a case report. Article in Japanese. No Shinkei Geka. 1989;17(3):291-295. - PubMed
LinkOut - more resources
Full Text Sources

