Lumbar angiomatous meningioma: how to manage this rare entity? A case report
- PMID: 40499448
- PMCID: PMC12179726
- DOI: 10.1016/j.ijscr.2025.111438
Lumbar angiomatous meningioma: how to manage this rare entity? A case report
Abstract
Introduction: Spinal meningiomas (SM) are rare intradural extramedullary tumors arising from arachnoid cells of the leptomeninges. They are most commonly found in the thoracic region, with angiomatous subtypes being even rarer and carrying a high hemorrhagic risk. Diagnosis and treatment are guided by clinical presentation and imaging, with surgery being the primary therapeutic approach. Recurrence is uncommon, occurring in 1.3 % to 6.4 % of cases, and decisions between surgery and adjuvant treatments like radiotherapy depend on factors such as tumor location, histological subtype, and the surgeon's expertise. This case aims to explore the radiological features and treatment strategies for SM.
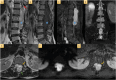
Case presentation: A 58-year-old man with a history of disc herniation surgery presented with lower back pain, bilateral sciatica, cruralgia, and sphincter dysfunction. Spinal MRI revealed an intra-dural, extra-medullary tumor, which was surgically removed and the patient had an uneventful postoperative recovery. Histopathological examination confirmed an angiomatous meningioma (WHO Grade 1).
Clinical discussion: SM are rare tumors, often causing pain and neurological issues. Imaging is crucial in assessing tumor extent and vascularization, helping in treatment decisions. Although recurrences aren't common, they are usually treated surgically, with adjuvant therapies like radiotherapy being considered for high-grade or inoperable tumors. Further research is needed to refine the understanding and management of spinal meningiomas.
Conclusion: SM are exceptional, mostly benign, slow-growing tumors, with surgical resection remaining the primary treatment and offering low recurrence rates. Adjuvant therapies, including radiotherapy and molecular-targeted treatments, remain largely investigational, with no established clinical application.
Keywords: Simpson grading; Spinal meningiomas; Spinal tumor.
Copyright © 2025. Published by Elsevier Ltd.
Conflict of interest statement
Declaration of competing interest The authors have nothing to declare.
Figures

References
-
- Dang D.D., Mugge L.A., Awan O.K., Gong A.D., Fanous A.A. Spinal meningiomas: a comprehensive review and update on advancements in molecular characterization, diagnostics, surgical approach and technology, and alternative therapies. Multidisciplinary Digital Publishing Institute (MDPI) 2024;16(7) doi: 10.3390/cancers16071426. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources

