Intensity-modulated moderately hypofractionated radiotherapy versus stereotactic body radiotherapy for prostate cancer (PACE-C): early toxicity results from a randomised, open-label, phase 3, non-inferiority trial
- PMID: 40517778
- PMCID: PMC7617972
- DOI: 10.1016/S1470-2045(25)00205-0
Intensity-modulated moderately hypofractionated radiotherapy versus stereotactic body radiotherapy for prostate cancer (PACE-C): early toxicity results from a randomised, open-label, phase 3, non-inferiority trial
Abstract
Background: Moderately hypofractionated radiotherapy (MHRT) is a standard treatment for prostate cancer. Stereotactic body radiotherapy (SBRT) is also effective, and has been shown to be non-inferior to MHRT in a lower-risk group of patients who did not require hormone therapy (PACE-B), but randomised data on toxicity for higher-risk patients are lacking. We aimed to compare the early toxicity of MHRT and SBRT.
Methods: The randomised, open-label, phase 3, non-inferiority PACE-C trial, conducted at 53 hospitals across the UK, Republic of Ireland, and New Zealand, recruited men aged at least 18 years with intermediate-risk or high-risk histologically confirmed prostate adenocarcinoma (T1-T3a, Gleason 7-8, and prostate specific antigen 10-30 ng/mL) and with WHO performance status of 0-2. Participants were centrally randomly assigned (1:1; non-masked; permuted block size of four and six; stratified by centre and risk group) to MHRT (60 Gy; 20 daily fractions over 4 weeks) or SBRT (36·25 Gy; five daily or alternate day fractions; over 1-2 weeks) with an additional mandatory clinical target volume dose target of 40 Gy (no margin) to the prostate, and proximal 1 cm of seminal vesicles. 6 months of androgen deprivation therapy was planned and was started before commencement of radiotherapy. The primary outcome of PACE-C is freedom from biochemical or clinical failure, the data for which are not yet mature. The co-primary endpoints for this preplanned safety analysis were the percentages of Radiation Therapy Oncology Group (RTOG) grade 2 or worse gastrointestinal and genitourinary toxicities at any point during or within 12 weeks of completion of radiotherapy (the early or acute period). Analyses are by treatment received, with participants included if they had one or more fractions of MHRT or SBRT, regardless of their allocated treatment. Late toxicity and efficacy data are awaited as the trial remains in follow-up. The study was prospectively registered with ClinicalTrials.gov, NCT01584258.
Findings: Between Nov 13, 2019, and June 24, 2022, 1208 participants were randomly assigned (601 to MHRT and 607 to SBRT). 608 patients received MHRT and 584 received SBRT, and thus were included in the study analysis. 1136 (95%) of 1192 patients were White, 20 (2%) were Black or Black British, 17 (1%) were Asian or Asian British, and seven (1%) were Chinese or other. During the early period (within 12 weeks of treatment), the co-primary endpoint of RTOG grade 2 or worse genitourinary toxicity was observed in 166 (27%) of 608 patients (95% CI 23·8 to 31·1) receiving MHRT and 162 (28%) of 582 patients (24·3 to 31·7) after SBRT (absolute difference 0·5%, 95% CI -4·7 to 5·7; p=0·89). For grade 2 or worse genitourinary Common Terminology Criteria for Adverse Events (CTCAE), 170 (28%) of 604 patients had events after MHRT and 195 (34%) of 581 patients had events after SBRT (p=0·050). Grade 3 CTCAE genitourinary toxicity was observed in three (<1%) patients receiving MHRT and three (1%) patients receiving SBRT. For grade 2 or worse gastrointestinal CTCAE, 60 (10%) of 604 patients had an event after MHRT and 96 (17%) of 581 patients had an event after SBRT (p=0·0011). Grade 3 CTCAE gastrointestinal toxicity was observed in three (<1%) patients receiving MHRT and four (1%) patients receiving SBRT. During the early period, the co-primary endpoint of RTOG grade 2 or worse gastrointestinal toxicity was observed in 69 (11%) of 608 patients (95% CI 9·0 to 14·2) receiving MHRT and 74 (13%) of 584 patients (10·2 to 15·8) receiving SBRT (absolute difference 1·4%, 95% CI -2·5 to 5·2; p=0·53). There were no treatment-related deaths.
Interpretation: Despite an accelerated treatment schedule and a larger treated volume than PACE-B, SBRT and MHRT had similar rates of early RTOG toxicity.
Funding: The Royal Marsden Cancer Charity.
Copyright © 2025 Elsevier Ltd. All rights reserved, including those for text and data mining, AI training, and similar technologies.
Conflict of interest statement
Declaration of interests ACT and NvA declare grants from Accuray for the PACE trial, the Royal Marsden Cancer Charity for the PACE-C trial, and from Varian, a Siemens Healthineers Company, for the PACE-A trial. ACT reports grants from Elekta for radiotherapy research and Cancer Research UK Cancer for Radiation Research Centre of Excellence at The Institute of Cancer Research (ICR) and The Royal Marsden NHS Foundation Trust (C33589/A28284, RRCOER-Jun24/100006, and C7224/A28724), payment for honoraria for talks from Elektra, Accuray, Janssen, and Bayer, travel support from Elekta, participation on the data safety and monitoring board for the KORTUC and NEPTUNES academic trials (no compensation), a role as lead genitourinary editor for the International Journal of Radiation Oncology, Biology and Physics (paid personally), and being chair of the MR Linac consortium steering committee (institutional financial support). VH, JP, GM, SBr, SBu, CG, and EH declare research grants received by their institution (ICR) for statistical analysis, later extended (at change of sponsor) to also cover central trial and data management with payment from Accuray via The Royal Marsden NHS Foundation Trust for the PACE trial, from Royal Marsden Cancer Charity with payment via The Royal Marsden NHS Foundation Trust for the PACE-C trial, and from Varian with payment via The Royal Marsden NHS Foundation Trust for the PACE-A trial. ST declares support for attending meetings and/or travel from Janssen and honoraria from Bayer and Astellas as a speaker fee for educational meetings. AL declares funding for Canadian patients received from Prostate Cure Foundation and his roles as a member of the American Society of Clinical Oncology Prostate Cancer Guideline Committee, chair/founder of the Prostate Cure Foundation, co-chair of the Program in Evidence Based Care Genitourinary Site CancerCare Ontario, co-chair Genitourinary Site Sunnybrook Health Sciences Centre, and chair of the Genitourinary Radiation Oncology Clinical Study Group, Sunnybrook Health Sciences Centre. SJ declares grants or contracts from Prostate Cancer UK and the Causeway Trust, consulting fees from Boston Scientific and BXT Nanotherapy, payment or honoraria for lectures, presentations, speakers bureaus, manuscript writing, or educational events from Accuray, Boston Scientific, Janssen, Astellas, and Bayer, support for attending meetings and/or travel from Bayer, Astellas, and Janssen, and as chair of the independent data monitoring and steering committee for the HERMES clinical trial, on advisory boards for Boston Scientific, Pfizer, Astra Zeneca, Bayer, and BXT Nanotherapy, and as a board member of the Friends of Cancer Centre, and receipt of equipment, materials, drugs, medical writing, gifts, or other services from Boston Scientific. AM declares he is a paid employee of GenesisCare UK on the MR Linac rota and stereotactic ablative radiotherapy advisory team. DP declares travel support for attending a meeting from Prostate Cancer UK. PK declares consulting fees from Boston Scientific and payment for expert testimony from State Claims Agency, Ireland. GS declares a research grant for New Zealand patients received from Auckland Medical Research Foundation. EH declares grants received by the ICR from Astra Zeneca, Janssen-Cilag, Bayer, Roche Products, from Varian, a Siemens Healthineers, Company, and Merck Sharp & Dohme. NvA declares payment or honoraria and support for attending meetings from Accuray and travel support from Accuray. All other authors declare no competing interests.
Figures


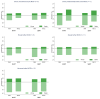
References
-
- National Prostate Cancer Audit. NPCA State of the Nation Report. https://www.npca.org.uk/content/uploads/2024/02/REF433_NPCA-SotN-Report_... .
-
- Dearnaley D, Syndikus I, Mossop H, et al. Conventional versus hypofractionated high-dose intensity-modulated radiotherapy for prostate cancer : 5-year outcomes of the randomised, non-inferiority, phase 3 CHHiP trial. Lancet Oncology. 2016;2045(16):1–14. doi: 10.1016/S1470-2045(16)30102-4. - DOI - PMC - PubMed
-
- Catton CN, Lukka H, Gu CS, et al. Randomized Trial of a Hypofractionated Radiation Regimen for the Treatment of Localized Prostate Cancer. J Clin Oncol. 2017;35:1884–1890. JOURNAL OF CLINICAL ONCOLOGY. - PubMed
-
- Kerkmeijer LGW, Groen VH, Pos FJ, et al. Focal Boost to the Intraprostatic Tumor in External Beam Radiotherapy for Patients With Localized Prostate Cancer: Results From the FLAME Randomized Phase III Trial. J Clin Oncol. 2021;39(7):787–796. - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

