A scoping review of vulvodynia research: Diagnosis, treatment, and care experiences
- PMID: 40525542
- PMCID: PMC12174717
- DOI: 10.1177/17455057251345946
A scoping review of vulvodynia research: Diagnosis, treatment, and care experiences
Abstract
Background: Vulvodynia is a significant genital pain condition, affecting an estimated 10% to 28% of individuals worldwide. Its multifactorial etiology, diagnostic challenges, and limited treatment options contribute to its substantial personal and socioeconomic burden. Despite its prevalence, vulvodynia remains under-recognized and under-researched, necessitating a comprehensive review of existing evidence to inform future research strategies.
Objective: This scoping review examines the extent and nature of clinical and psychosocial research on vulvodynia, with a focus on diagnosis, treatment, healthcare access, and its impact on quality of life, psychological well-being, and intimate relationships.
Eligibility criteria: Eligible studies included primary research using quantitative, qualitative, or mixed methods designs, as well as systematic, scoping, and topical reviews. Studies were included if they examined clinical or psychosocial aspects of vulvodynia. Research on other types of vulvar pain, animal studies, neurobiological research, and studies from non-high-income countries were excluded.Sources of Evidence and Methods:A systematic search of Medline, PubMed, CINAHL, PsycINFO, and Cochrane was conducted in March 2024 using predefined search terms related to vulvodynia, diagnosis, treatment, and patient experiences. Review findings, limitations, and recommendations were extracted to provide an overview of existing research, mapping methodologies, measures, and key findings of primary studies on vulvodynia.
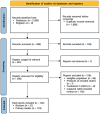
Results: A total of 144 articles were included, comprising 21 reviews and 123 primary studies. Clinical research primarily addressed diagnosis, risk factors, and comorbidities, while treatment studies evaluated pharmacological therapies, psychological therapies, laser therapy, physiotherapy, acupuncture, and multidisciplinary approaches. Psychosocial research focused on patient experiences, psychosocial factors, and barriers to care. However, methodological limitations, inconsistent measurement tools, limited patient involvement, and study heterogeneity challenge the generalizability of findings.
Conclusions: This review highlights critical gaps in vulvodynia research. Despite considerable research efforts, vulvodynia remains poorly understood. Addressing methodological weaknesses and involving patients more robustly in research design are essential to advance knowledge and improve care outcomes in vulvodynia.
Keywords: clinical; psychosocial research; vulval pain; vulvodynia.
Plain language summary
Understanding vulvodynia: What research tells us about diagnosis, treatment, and patient experiences Vulvodynia is a chronic pain condition affecting the vulva that can cause burning, stinging, or sharp pain, sometimes making daily activities and sexual intercourse difficult. Despite affecting up to 1 in 10 women, vulvodynia remains poorly understood, underdiagnosed, and undertreated. Many people with vulvodynia face long delays in getting a diagnosis, inconsistent treatment recommendations, and a lack of clear care pathways. This study reviews clinical and psychosocial research on vulvodynia published between 2015 and 2024, analyzing 144 studies to understand how the condition is diagnosed, treated, and experienced. Our findings show that diagnostic criteria and treatment approaches vary widely, making it difficult for healthcare providers to offer consistent care. Treatments range from medications (e.g. lidocaine, antidepressants, gabapentin), physiotherapy, psychological therapies (cognitive behavioral therapy, acceptance and commitment therapy), laser treatment, and even surgery. However, there is no universal treatment plan, and many approaches lack strong evidence to support their effectiveness. We also found that psychosocial factors, such as anxiety, depression, and relationship difficulties, play a significant role in the impact of vulvodynia. Many women feel dismissed by healthcare professionals and experience stigma, frustration, and isolation when seeking help. Peer support and mental health care were identified as crucial but under-researched areas. Overall, this review highlights critical gaps in vulvodynia research, including the need for standardized diagnosis and treatment guidelines, better outcome measures, and greater involvement of patients in research design. Addressing these gaps can help improve awareness, treatment options, and patient experiences.Key Takeaway: Vulvodynia research has grown in recent years, but many knowledge gaps remain. Improving diagnosis, treatment, and healthcare experiences is critical to supporting those living with this condition.
Conflict of interest statement
Declaration of conflicting interestsThe author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
Similar articles
-
Factors that influence participation in physical activity for people with bipolar disorder: a synthesis of qualitative evidence.Cochrane Database Syst Rev. 2024 Jun 4;6(6):CD013557. doi: 10.1002/14651858.CD013557.pub2. Cochrane Database Syst Rev. 2024. PMID: 38837220 Free PMC article. Review.
-
Home treatment for mental health problems: a systematic review.Health Technol Assess. 2001;5(15):1-139. doi: 10.3310/hta5150. Health Technol Assess. 2001. PMID: 11532236
-
Health professionals' experience of teamwork education in acute hospital settings: a systematic review of qualitative literature.JBI Database System Rev Implement Rep. 2016 Apr;14(4):96-137. doi: 10.11124/JBISRIR-2016-1843. JBI Database System Rev Implement Rep. 2016. PMID: 27532314
-
Exercise interventions and patient beliefs for people with hip, knee or hip and knee osteoarthritis: a mixed methods review.Cochrane Database Syst Rev. 2018 Apr 17;4(4):CD010842. doi: 10.1002/14651858.CD010842.pub2. Cochrane Database Syst Rev. 2018. PMID: 29664187 Free PMC article.
-
Interventions to improve safe and effective medicines use by consumers: an overview of systematic reviews.Cochrane Database Syst Rev. 2014 Apr 29;2014(4):CD007768. doi: 10.1002/14651858.CD007768.pub3. Cochrane Database Syst Rev. 2014. PMID: 24777444 Free PMC article.
References
-
- Bornstein J, Goldstein AT, Stockdale CK, et al. 2015 ISSVD, ISSWSH, and IPPS consensus terminology and classification of persistent vulvar pain and vulvodynia. J Sex Med 2016; 13(4): 607–612. - PubMed
-
- Bergeron S, Reed BD, Wesselmann U, et al. Vulvodynia. Nat Rev Dis Primer 2020; 6(1): 36. - PubMed
-
- Pukall CF, Goldstein AT, Bergeron S, et al. Vulvodynia: definition, prevalence, impact, and pathophysiological factors. J Sex Med 2016; 13(3): 291–304. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources