Glycogen synthase kinase 3β: a key player in progressive chronic kidney disease
- PMID: 40526103
- PMCID: PMC12238819
- DOI: 10.1042/CS20245219
Glycogen synthase kinase 3β: a key player in progressive chronic kidney disease
Abstract
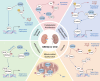
Chronic kidney disease (CKD) is a serious medical condition that poses substantial burdens on patients, families, healthcare systems, and society as a whole. It is characterized by progressive kidney damage and loss of function in the kidney, often compounded by underlying conditions such as diabetes, hypertension, and autoimmune diseases. Glycogen synthase kinase 3 beta (GSK3β), a highly conserved serine/threonine kinase originally implicated in insulin signaling, has emerged as a convergent point of multiple pathways implicated in the pathogenesis and progression of CKD. In the kidney, GSK3β regulates cell fate across diverse cells, including podocytes, mesangial cells, and renal tubular cells, through its interactions with key signaling pathways such as Wnt/β-catenin, NF-κB, Nrf2, PI3K/Akt, and cytoskeleton remodeling pathways. Evidence suggests that dysregulation of GSK3β is closely associated with pathological changes in the kidney, including podocyte injury, mesangial expansion, interstitial fibrosis, and tubular atrophy, which collectively drive chronic kidney destruction. In CKD, GSK3β is overexpressed and thus hyperactive in kidney cells. This sustained hyperactivity perpetuates oxidative stress and profibrotic signaling, particularly in renal tubular cells, thus accelerating the transition from acute kidney injury to CKD. Pharmacological targeting of GSK3β with selective inhibitors has shown promise in preclinical models, by reducing kidney injury, attenuating renal fibrosis, and promoting renal recovery, positioning GSK3β as a potential therapeutic target for CKD. This review highlights recent advances in understanding the molecular and cellular mechanisms through which GSK3β contributes to CKD and underscores its potential as a therapeutic target for various chronic renal diseases.
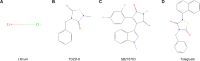
Keywords: CKD; GSK3; Lithium; Oxidative stress; podocytopathy.
© 2025 The Author(s).
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures



Similar articles
-
Aloe-emodin ameliorates chronic kidney disease fibrosis by inhibiting PI3K-mediated signaling pathway.Eur J Histochem. 2025 Jun 17;69(3). doi: 10.4081/ejh.2025.4228. Epub 2025 Aug 6. Eur J Histochem. 2025. PMID: 40832995
-
Hepatocyte Growth Factor-Modified Dental Pulp Stem Cells Potentially Regulate Novel Renal Fibrosis-Associated Gene via PI3K/AKT/GSK3β Pathway to Alleviate Renal Fibrosis.Hum Gene Ther. 2025 Jul;36(13-14):956-975. doi: 10.1089/hum.2025.044. Epub 2025 Jun 4. Hum Gene Ther. 2025. PMID: 40462757
-
HIF-1α participates in the regulation of S100A16-HRD1-GSK3β/CK1α pathway in renal hypoxia injury.Cell Death Dis. 2024 May 6;15(5):316. doi: 10.1038/s41419-024-06696-5. Cell Death Dis. 2024. PMID: 38710691 Free PMC article.
-
MAPK, PI3K/Akt Pathways, and GSK-3β Activity in Severe Acute Heart Failure in Intensive Care Patients: An Updated Review.J Cardiovasc Dev Dis. 2025 Jul 10;12(7):266. doi: 10.3390/jcdd12070266. J Cardiovasc Dev Dis. 2025. PMID: 40710791 Free PMC article. Review.
-
Glycogen Synthase Kinase-3 Beta (GSK3β) as a Potential Drug Target in Regulating Osteoclastogenesis: An Updated Review on Current Evidence.Biomolecules. 2024 Apr 21;14(4):502. doi: 10.3390/biom14040502. Biomolecules. 2024. PMID: 38672518 Free PMC article. Review.
References
-
- Hu, J., Ke, R., Teixeira, W., Dong, Y., Ding, R., Yang, J.et al. (2023) Global, regional, and national burden of ckd due to glomerulonephritis from 1990 to 2019: a systematic analysis from the global burden of disease study 2019. Clin. J. Am. Soc. Nephrol. 18, 60–71 10.2215/CJN.0000000000000017 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

