Comparing glucose monitoring methods: efficiency insights in a simulated hospital setting
- PMID: 40529215
- PMCID: PMC12170324
- DOI: 10.3389/fcdhc.2025.1517161
Comparing glucose monitoring methods: efficiency insights in a simulated hospital setting
Abstract
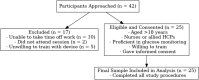
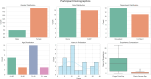
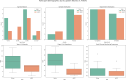
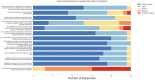
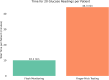
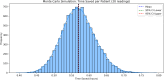
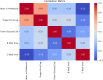
While the advantages of flash glucose monitoring, also known as dynamic interstitial glucose monitoring (DIGM), are established in outpatient diabetes care, evidence of its impact within hospital settings remains limited. This study compared the efficiency of use and healthcare staff perception of DIGM monitoring versus traditional finger-prick testing in a simulated hospital environment. Twenty-five healthcare professionals (52% nurses, 48% allied healthcare professionals [AHCPs]) participated in simulated clinical scenarios involving glucose monitoring tasks using a high-fidelity mannequin. Participants performed three tasks: (A) applying a flash sensor, (B) scanning the sensor to obtain a glucose reading, and (C) performing a finger-prick test. Task durations and staff perceptions were assessed, with statistical analyses conducted using Python (version 3). DIGM was significantly faster than finger-prick testing. Sensor application took 75.4 ± 22.4 seconds, flash scanning took 26.4 ± 11.5 seconds, and finger-prick testing required 132.8 ± 37 seconds (p < 0.05 for all comparisons). DIGM saved approximately 106 seconds per glucose check based on these timings. Furthermore, a scenario of 20 readings per hospitalized patient translates to an average of 34.2 minutes saved per patient. While staff with greater experience performed tasks slightly faster, the overall time-saving benefit of DIGM remained substantial across all levels of experience. In addition, survey responses revealed a strong staff preference for DIGM, highlighting perceived benefits in workflow efficiency, patient comfort, and infection control. In conclusion, DIGM was significantly more efficient than finger-prick testing and strongly preferred by clinical staff. These technologies offer time-saving benefits that could improve patient experience, streamline clinical workflows, and potentially enhance diabetes management outcomes.
Keywords: FreeStyle Libre; capillary blood glucose monitoring; continuous glucose monitoring; diabetes; finger-prick test; flash glucose monitoring-dynamic interstitial glucose monitoring; staff perception.
Copyright © 2025 Davasgaium, Robbins, Leca, Epure, Sankar and Randeva.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
Similar articles
-
Return to Running After Achilles Tendon Repair: How Do US Navy Service Members' Physical Readiness Tests Change After Undergoing an Achilles Tendon Repair?Clin Orthop Relat Res. 2025 Jun 18. doi: 10.1097/CORR.0000000000003590. Online ahead of print. Clin Orthop Relat Res. 2025. PMID: 40536551
-
Surveillance for Violent Deaths - National Violent Death Reporting System, 50 States, the District of Columbia, and Puerto Rico, 2022.MMWR Surveill Summ. 2025 Jun 12;74(5):1-42. doi: 10.15585/mmwr.ss7405a1. MMWR Surveill Summ. 2025. PMID: 40493548 Free PMC article.
-
Psychometric properties of the Chinese version of the pros and cons of anorexia nervosa (P-CAN-C) scale: a validation study in patients with anorexia nervosa.J Eat Disord. 2025 Jun 16;13(1):111. doi: 10.1186/s40337-025-01314-x. J Eat Disord. 2025. PMID: 40524259 Free PMC article.
-
Sociodemographic and Socioeconomic Determinants for the Usage of Digital Patient Portals in Hospitals: Systematic Review and Meta-Analysis on the Digital Divide.J Med Internet Res. 2025 Jun 3;27:e68091. doi: 10.2196/68091. J Med Internet Res. 2025. PMID: 40460427 Free PMC article. Review.
-
Assessing the comparative effects of interventions in COPD: a tutorial on network meta-analysis for clinicians.Respir Res. 2024 Dec 21;25(1):438. doi: 10.1186/s12931-024-03056-x. Respir Res. 2024. PMID: 39709425 Free PMC article. Review.
References
-
- Umpierrez GE, Pasquel FJ. Management of diabetes and hyperglycemia in hospitalized patients. In: Feingold KR, et al., editors. Endotext. MDText.com, Inc, South Dartmouth, MA: (2022). (updated 2022).
LinkOut - more resources
Full Text Sources

