Continuous Glucose Monitoring in Primary Care: Multidisciplinary Pilot Implementation Study
- PMID: 40532195
- PMCID: PMC12192913
- DOI: 10.2196/69061
Continuous Glucose Monitoring in Primary Care: Multidisciplinary Pilot Implementation Study
Abstract
Background: Continuous glucose monitoring (CGM) is used to assess glycemic trends and guide therapeutic changes for people with diabetes. We aimed to increase patient access to this tool by equipping primary care physicians (PCPs) to accurately interpret and integrate CGM into their practice via a multidisciplinary team approach.
Objective: The primary objective of this study was to evaluate the feasibility and effectiveness of integrating CGM into primary care clinics using a multidisciplinary approach that included a clinical pharmacist (PharmD) and a certified diabetes care and education specialist (CDCES).
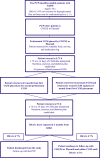
Methods: Eighteen PCPs received a 1-hour video training module from an endocrinologist teaching a systematic stepwise approach to CGM interpretation. Patient inclusion criteria included type 2 diabetes mellitus, ≥18 years old, hemoglobin A1c (HbA1c) ≥8% or concern for hypoglycemia, and no previous CGM use or an endocrinology visit in the past year. Patients saw physician extenders (CDCES or a PharmD) for professional CGM placement and education on nutrition, medication administration, and physical activity goals based on the PCP's recommendations. The CDCES or PharmD reviewed CGM data with patients and collaborated with PCPs to adjust the care plan, informed by the systematic stepwise approach to CGM interpretation. Patients either converted to personal CGM if desired or had a second professional CGM device placed after ≥1 month from the initial professional CGM placement and obtained a postintervention HbA1c measurement at ≥3 months from the initial HbA1c measurement. The primary outcomes were time in range, HbA1c, and average time from referral to the first CGM device placement. Follow-up continued with the CDCES or PharmD until patients met the study discharge criteria of HbA1c level ≤7%. Paired t tests with 1-sided P values were used to assess changes in glucose metrics from the initial to postintervention measurements. The McNemar test was used to determine the significance of change in patients meeting the goal of ≥70% time in the target range of 70-180 mg/dL.
Results: The CGM users (n=46) had a mean (SD) age of 62.39 (14.57) years, and 14/46 participants (30%) were female. The mean (SD) time in range increased by 28.06%, from 43.25% (33.41%) at baseline to 71.31% (25.49%) postintervention (P<.001), due to reduced hyperglycemia. The proportion of CGM users meeting the consensus target of the time in range ≥70% increased from 23.81% to 57.14% (P<.001). Postintervention HbA1c decreased by an average of 2.37%, from 9.68% (1.78%) to 7.31% (1.32%; P<.001).
Conclusions: The integration of CGM into primary care clinics to increase patient access is feasible and effective using a multidisciplinary approach.
Keywords: continuous glucose monitoring; diabetes education; multidisciplinary team; primary care physicians; type 2 diabetes.
© Alyssa H Zadel, Katia Chiampas, Katrina Maktaz, John G Keller, Kathy W O'Gara, Leonardo Vargas, Angela Tzortzakis, Micah J Eimer, Emily D Szmuilowicz. Originally published in JMIR Diabetes (https://diabetes.jmir.org).
Conflict of interest statement
Figures
Similar articles
-
Continuous glucose monitoring systems for type 1 diabetes mellitus.Cochrane Database Syst Rev. 2012 Jan 18;1(1):CD008101. doi: 10.1002/14651858.CD008101.pub2. Cochrane Database Syst Rev. 2012. PMID: 22258980 Free PMC article.
-
Quality improvement strategies for diabetes care: Effects on outcomes for adults living with diabetes.Cochrane Database Syst Rev. 2023 May 31;5(5):CD014513. doi: 10.1002/14651858.CD014513. Cochrane Database Syst Rev. 2023. PMID: 37254718 Free PMC article.
-
Integrated sensor-augmented pump therapy systems [the MiniMed® Paradigm™ Veo system and the Vibe™ and G4® PLATINUM CGM (continuous glucose monitoring) system] for managing blood glucose levels in type 1 diabetes: a systematic review and economic evaluation.Health Technol Assess. 2016 Feb;20(17):v-xxxi, 1-251. doi: 10.3310/hta20170. Health Technol Assess. 2016. PMID: 26933827 Free PMC article.
-
Home treatment for mental health problems: a systematic review.Health Technol Assess. 2001;5(15):1-139. doi: 10.3310/hta5150. Health Technol Assess. 2001. PMID: 11532236
-
Signs and symptoms to determine if a patient presenting in primary care or hospital outpatient settings has COVID-19.Cochrane Database Syst Rev. 2022 May 20;5(5):CD013665. doi: 10.1002/14651858.CD013665.pub3. Cochrane Database Syst Rev. 2022. PMID: 35593186 Free PMC article.
References
-
- National diabetes statistics report. Centers for Disease Control and Prevention. 2024. [04-06-2025]. https://www.cdc.gov/diabetes/php/data-research/index.html URL. Accessed.
-
- National Vital Statistics System, mortality 2018-2023 on CDC WONDER online database. Centers for Disease Control and Prevention, National Center for Health Statistics. 2024. [06-05-2025]. http://wonder.cdc.gov/controller/saved/D158/D389F360 URL. Accessed.
LinkOut - more resources
Full Text Sources
Miscellaneous

