Modulating verticality representation and uprightness by virtual reality: rationale and protocol for a within-person randomised intervention associating a basic study in healthy individuals and a pilot clinical trial in individuals exhibiting post-stroke lateropulsion (VIRGIL)
- PMID: 40533218
- PMCID: PMC12182117
- DOI: 10.1136/bmjopen-2024-092406
Modulating verticality representation and uprightness by virtual reality: rationale and protocol for a within-person randomised intervention associating a basic study in healthy individuals and a pilot clinical trial in individuals exhibiting post-stroke lateropulsion (VIRGIL)
Abstract
Introduction: Balance and gait disorders represent the most frequent and disabling sequelae after stroke. Impaired body orientation with respect to gravity (lateropulsion) is one of the primary underlying mechanisms, increasingly investigated. After hemisphere stroke, lateropulsion is caused by an impaired internal representation of verticality, for which developing rehabilitation techniques has become a priority. Among various approaches, virtual reality appears to be a promising tool for modulating spatial reference frame. The objective of this study is to investigate the effects of immersion in virtual tilted reality (VTR) on the postural vertical (PV) as a primary outcome, as well as main secondary outcomes on the visual vertical (VV) and the active standing posture (body orientation with respect to gravity and weight-bearing (WB) distribution on lower limbs), both in healthy individuals and individuals exhibiting lateropulsion at the subacute phase after a hemispheric stroke. The cumulative effect of the VTR on the post-stroke lateropulsion will also be analysed.
Methods and analysis: This pilot study is a single-centre, within-person randomised trial conducted in the department of Physical and Rehabilitation Medicine of the University Hospital of Grenoble-Alpes (France). We will include 40 individuals from 18 to 85 years old, 20 healthy individuals and 20 individuals with lateropulsion tested <9 months after a hemisphere stroke. Both groups will be matched on age. Each VTR immersion lasts about 45 min. For healthy participants, the study duration is two half-days, one devoted to testing the effect of VTR on verticality perception (PV and VV), and the other to test the effect of VTR on the active standing (body orientation with respect to gravity and WB distribution on lower limbs). For participants with post-stroke lateropulsion (score >0.5 on the Scale for Contraversive Pushing), the study lasts 4 weeks: W1 for inclusion, randomisation, planning and conventional rehabilitation; W2 and W4 to collect clinical data and conventional rehabilitation; and W3 for the VTR intervention over four consecutive mornings at the same time: 2 to test the VTR effects on verticality perception (PV and VV) and 2 to test the VTR effects on active standing (body orientation and WB distribution on lower limbs). Immediate effects and post-effects of the VTR immersion are analysed by comparing results of the following time points: for verticality perception baseline, during and after VTR and for active standing at only baseline and during VTR immersion. Linear mixed-effect models will be run with different factors/covariates according to objectives. We will analyse the proportion and features of responders (PV modulation ≥2°). The cumulative effect of the 4 days of VTR sessions will be analysed by comparing scores of the SCAle for LAteropulsion assessed at the end of every week.
Ethics and dissemination: The study was approved by an institutional review board at the national level (Comité de Protection des Personnes Ile de France X; 2020-A02941-38, amendment 2024). All participants will provide written informed consent before enrolment. Findings will be submitted to peer-reviewed journals related to rehabilitation, stroke or neuroscience.
Trial registration number: ClinicalTrials.gov, NCT04911738.
Keywords: Posture; REHABILITATION MEDICINE; Stroke; Virtual Reality.
© Author(s) (or their employer(s)) 2025. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ Group.
Conflict of interest statement
Competing interests: None declared.
Figures
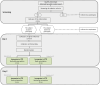
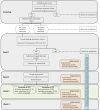


References
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
