Preventing chronic kidney disease and maintaining kidney health: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) Controversies Conference
- PMID: 40536455
- PMCID: PMC12646115
- DOI: 10.1016/j.kint.2025.04.005
Preventing chronic kidney disease and maintaining kidney health: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) Controversies Conference
Abstract
To date, the primary focus of chronic kidney disease (CKD) care has been on managing disease progression, complications, and kidney failure. In contrast, maintaining kidney health and preventing CKD have received limited attention, despite their potential to save millions of lives, reduce health care costs, and lessen environmental burdens. The cardiovascular-kidney-metabolic (CKM) concept frames CKD as part of a complex, high-risk syndrome requiring global risk assessment and multifactorial intervention. CKD incidence along with CKM risk factors may be reduced by a healthy diet, physical activity, and a supportive environment. However, risk for CKD does extend beyond the cardiovascular-metabolic component, and residual risk persists despite healthy lifestyles and treatment of risk factors. Post hoc analyses of clinical trials suggest pharmacological interventions, such as sodium-glucose cotransporter-2 inhibitors and glucagon-like peptide-1 receptor agonists, may help to prevent or regress CKD in individuals with type 2 diabetes or obesity. Clinical trials are needed to validate these findings in broader high-risk populations. Personalized strategies to improve kidney health should include CKD risk prediction via targeted testing, genetic or biomarker assessments, shared decision-making, cost considerations, selection of therapeutics, and the potential for adverse effects. The overall goals of CKD prevention should prioritize a lifespan approach to risk evaluation along with safe, efficacious, and accessible interventions to maintain kidney health.
Keywords: CKD prevention; case finding; interventions; screening.
Copyright © 2025 Kidney Disease: Improving Global Outcomes (KDIGO). Published by Elsevier Inc. All rights reserved.
Figures
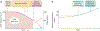

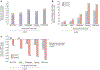
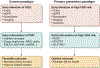

References
-
- Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2024 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int. 2024;105(4S):S117–S314. - PubMed
-
- Jager KJ, Kovesdy C, Langham R, et al. A single number for advocacy and communication-worldwide more than 850 million individuals have kidney diseases. Nephrol Dial Transplant. 2019;34:1803–1805. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

