Mass Spectrometry-Based Untargeted Metabolomics Identifies Distinct Metabolic Signatures in Infertility: A Comparative Analysis of PCOS, POR, and NOR
- PMID: 40537734
- PMCID: PMC12271243
- DOI: 10.1007/s43032-025-01908-5
Mass Spectrometry-Based Untargeted Metabolomics Identifies Distinct Metabolic Signatures in Infertility: A Comparative Analysis of PCOS, POR, and NOR
Abstract
Background: Infertility affects approximately 15% of reproductive-age couples, with polycystic ovary syndrome and poor ovarian reserve being major contributing factors. Metabolomic profiling of follicular fluid offers insights into the underlying metabolic disturbances associated with these infertility phenotypes. This study aims to identify metabolic biomarkers distinguishing PCOS, POR, and male factor infertility, which may facilitate improved diagnostic and therapeutic strategies.
Methods: A total of 119 participants were categorized into three groups: PCOS (n = 39), POR (n = 40), and NOR (n = 40). Liquid chromatography-high-resolution mass spectrometry was used for untargeted metabolomic profiling. Metabolites were identified using HMDB, MassBank, and MoNA, while pathway analysis was performed using KEGG. Statistical analyses were conducted using R and Python, including one-way ANOVA, t-tests, and Mann-Whitney U tests, with False Discovery Rate correction applied.
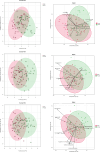
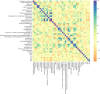
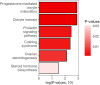
Results: Distinct metabolic alterations were observed among the groups. Trehalose-6-phosphate, taurocholate, and N,N-dimethylglycine emerged as the most significantly altered metabolites, showing strong discriminatory potential between PCOS and POR. PCOS patients exhibited reduced levels of taurocholate, mycalemide, and trehalose-6-phosphate, whereas NOR patients showed elevated levels of N,N-dimethylglycine and argininosuccinate. The POR group demonstrated increased levels of 1-methyl-2-pyrrolidone and haplopine, along with a broader metabolite distribution.
Conclusion: This study reveals phenotype-specific metabolic signatures in PCOS and POR, identifying taurocholate, mycalemide, and N,N-dimethylglycine as potential follicular biomarkers. These findings contribute to a deeper understanding of the metabolic basis of infertility and highlight the potential of follicular fluid metabolomics for precision medicine in reproductive health.
Keywords: Follicular fluid; Infertility; Metabolic pathways; Polycystic ovary syndrome; Poor ovarian reserve; Taurocholate; Trehalose-6-phosphate; Untargeted metabolomics.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Conflicts of Interest: The authors declare no conflicts of interest related to this study. Ethics Approval: This study was approved by the Research Ethics Committee of Bezmialem Vakıf University (Approval Number: 173773) Consent to Participate: All participants provided written informed consent prior to their inclusion in the study. Consent for Publication: All authors have reviewed and approved the manuscript for publication.
Figures



Similar articles
-
Non-targeted metabolomic analysis of follicular fluid in infertile individuals with poor ovarian response.Front Endocrinol (Lausanne). 2025 May 12;16:1547550. doi: 10.3389/fendo.2025.1547550. eCollection 2025. Front Endocrinol (Lausanne). 2025. PMID: 40421242 Free PMC article.
-
Biomarkers identification in follicular fluid in relation to live birth in in vitro fertilization of women with polycystic ovary syndrome in different subtypes by using UPLC-MS method.Clin Chim Acta. 2024 Apr 15;557:117860. doi: 10.1016/j.cca.2024.117860. Epub 2024 Mar 18. Clin Chim Acta. 2024. PMID: 38508572
-
Metabolomics as a tool to identify biomarkers to predict and improve outcomes in reproductive medicine: a systematic review.Hum Reprod Update. 2017 Nov 1;23(6):723-736. doi: 10.1093/humupd/dmx023. Hum Reprod Update. 2017. PMID: 29069503
-
Plasma metabolites associated with endometriosis in adolescents and young adults.Hum Reprod. 2025 May 1;40(5):843-854. doi: 10.1093/humrep/deaf040. Hum Reprod. 2025. PMID: 40107296
-
Insulin-sensitising drugs (metformin, rosiglitazone, pioglitazone, D-chiro-inositol) for women with polycystic ovary syndrome, oligo amenorrhoea and subfertility.Cochrane Database Syst Rev. 2017 Nov 29;11(11):CD003053. doi: 10.1002/14651858.CD003053.pub6. Cochrane Database Syst Rev. 2017. PMID: 29183107 Free PMC article.
References
-
- World Health Organization. Infertility prevalence estimates, 1990–2021. World Health Organization; 2023.
-
- The Rotterdam ESHRE/ASRM-sponsored PCOS Consensus Workshop Group. Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS). Hum Reprod. 2004;19:41–7. 10.1093/humrep/deh098. - PubMed
-
- Ferraretti AP, La Marca A, Fauser BC, Tarlatzis B, Nargund G, Gianaroli L, et al. ESHRE consensus on the definition of 'poor response' to ovarian stimulation for in vitro fertilization: the Bologna criteria. Hum Reprod. 2011;26:1616–24. 10.1093/humrep/der092. - PubMed
-
- Broekmans FJ, Soules MR, Fauser BC. Ovarian aging: mechanisms and clinical consequences. Endocr Rev. 2009;30:465–93. 10.1210/er.2009-0006. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

