Impact of systemic lupus erythematosus on adverse outcomes and readmission after total shoulder arthroplasty: a Nationwide Readmission Database analysis 2016-2020
- PMID: 40542928
- PMCID: PMC12182537
- DOI: 10.1186/s10195-025-00858-7
Impact of systemic lupus erythematosus on adverse outcomes and readmission after total shoulder arthroplasty: a Nationwide Readmission Database analysis 2016-2020
Abstract
Background: The impact of systemic lupus erythematosus (SLE) on total shoulder arthroplasty (TSA) outcomes is unclear. This study investigated the association between SLE and short-term TSA outcomes.
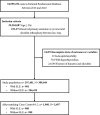
Methods: Data from the Nationwide Readmission Database (NRD) 2016-2020 of patients ≥ 20 years old who underwent primary TSA were included. SLE was identified by International Classification of Diseases, Tenth Revision, and Clinical Modification (ICD-10-CM) codes. Outcomes were compared between patients with and without SLE, and propensity-score matching based on age and sex was performed.
Results: This study included 1960 matched TSA patients (980 with SLE and 980 without SLE). The mean patient age was 65.7 years, and 92% were female. After adjusting for covariates, SLE was significantly associated with a higher risk of surgical complications (odds ratio [OR] = 1.48, 95% confidence interval [CI]: 1.13-1.93), acute postoperative hemorrhagic anemia (OR = 1.48, 95% CI 1.05-2.09), and increased 30-day (OR = 2.11, 95% CI 1.30-3.40) and 90-day (OR = 1.59, 95% CI 1.11-2.26) readmission rates. Patients with SLE with Charlson Comorbidity Index scores of 0 or > 1 had a significantly higher 90-day readmission rate (OR = 2.45 and 1.48, respectively). Additionally, patients with SLE ≥ 65 years old had a significantly higher risk of complications (OR = 1.56). Patients with SLE undergoing reverse TSA also exhibited a significantly increased 90-day readmission risk (OR = 1.71).
Conclusions: SLE significantly increases the risk of postoperative complications and readmissions following TSA, especially in older patients and those undergoing reverse TSA. However, the lack of data on immunosuppressive therapy, laboratory tests, and disease activity may weaken the strength of the evidence.
Keywords: Nationwide Readmission Database (NRD); Outcome; Readmission; Systemic lupus erythematous (SLE); Total shoulder arthroplasty (TSA).
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: This study adheres to the NRD data use agreement guidelines. The data were acquired through the Online HCUP Central Distributor and consist of secondary, anonymized information, with no involvement from individual patients. Therefore, additional informed consent was not required. Consent for publication: All authors approve the manuscript and give their consent for submission and publication. Competing interests: The authors declare no competing interests.
Figures
Similar articles
-
Hospital Readmissions Among People With Sickle Cell Disease.JAMA Netw Open. 2025 Jun 2;8(6):e2517974. doi: 10.1001/jamanetworkopen.2025.17974. JAMA Netw Open. 2025. PMID: 40526379 Free PMC article.
-
Total Shoulder Arthroplasty in Patients With Hemophilia A: Greater Odds of Postoperative Bleeding and Thromboembolic Events but No Difference in 5-year Implant Survival.Clin Orthop Relat Res. 2025 Feb 1;483(2):268-275. doi: 10.1097/CORR.0000000000003209. Epub 2024 Sep 3. Clin Orthop Relat Res. 2025. PMID: 39246053
-
30-day readmission after total hip and knee arthroplasty in patients with systemic lupus erythematosus: A US nationwide study.J Orthop. 2025 May 6;64:210-216. doi: 10.1016/j.jor.2025.05.017. eCollection 2025 Jun. J Orthop. 2025. PMID: 40548201
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
-
The safety of outpatient total shoulder arthroplasty: a systematic review and meta-analysis.Int Orthop. 2021 Mar;45(3):697-710. doi: 10.1007/s00264-021-04940-7. Epub 2021 Jan 23. Int Orthop. 2021. PMID: 33486581 Free PMC article.
References
-
- Italia K, Jomaa M, Pareyon R, Hollman F, Cutbush K, Gupta A (2023) Outcomes and survivorship of anatomic total shoulder arthroplasty: current concepts. J Isakos 8(5):284–288. 10.1016/j.jisako.2023.04.002 - PubMed
-
- Best MJ, Aziz KT, Wilckens JH, McFarland EG, Srikumaran U (2021) Increasing incidence of primary reverse and anatomic total shoulder arthroplasty in the United States. J Shoulder Elbow Surg 30(5):1159–1166. 10.1016/j.jse.2020.08.010 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials