CT delta-radiomics predicts the risks of blood transfusion and massive bleeding during spinal tumor surgery
- PMID: 40545537
- PMCID: PMC12183832
- DOI: 10.1186/s40644-025-00900-1
CT delta-radiomics predicts the risks of blood transfusion and massive bleeding during spinal tumor surgery
Abstract
Background: Intraoperative bleeding is a serious complication of spinal tumor surgery. Preoperative identification of patients at high risk of intraoperative blood transfusion (IBT) and intraoperative massive bleeding (IMB) before spinal tumor resection surgery is difficult but critical for surgical planning and blood management. This study aims to develop and validate delta radiomics prediction models for IBT and IMB in spinal tumor surgery.
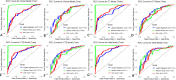
Methods: Patients diagnosed with spinal tumors who underwent spinal tumor resection surgery were retrospectively recruited. CT, CTE, delta, and clinical models based on CT native phase, CT arterial phase images, and clinical factors were constructed using 10-fold cross-validation and logistic regression (LR), random forest (RF), and support vector machine (SVM) in the training cohort. Receiver operating characteristic (ROC) curves, integrated discrimination improvement (IDI), accuracy, sensitivity, specificity, positive predictive value, and negative predictive value were used to evaluate and compare the diagnostic performance of these models.
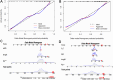
Results: 231 patients were randomly divided into training (n = 161) and test (n = 70) cohorts, comprising 146 IBT and 85 no-IBT patients, 35 IMB and 196 no-IMB patients, respectively. The delta model performed best in predicting IBT and IMB risk, with better predictive ability than the clinical model (IDI = 0.11-0.13 for IBT, and IDI = 0.02-0.08 for IMB, p < 0.05, respectively). Calibration curves indicated that the predicted probabilities of IBT and IMB in the model did not differ significantly from the actual probabilities (p > 0.05).
Conclusion: The CT delta model we constructed may be a valuable tool to improve risk stratification before spinal tumor surgery, thus contributing to preoperative planning and improving patient prognosis.
Trial registration: Retrospectively registered (M2020435).
Keywords: Blood transfusion; Delta-radiomics; Intraoperative bleeding; Logistic regression; Spinal tumor.
© 2025. The Author(s).
Conflict of interest statement
Declarations. Ethics approval and consent to participate: Written informed consent was not required for this study because retrospective study and Peking University Third Hospital Institutional Review Board approval was obtained (M2020435). Consent for publication: Written informed consent was obtained from the patient for publication of this research and any accompanying images. Competing interests: The authors declare no competing interests.
Figures




Similar articles
-
Longitudinal computed tomography-based delta-radiomics of visceral adipose tissue predicts infliximab secondary loss of response in Crohn's disease patients.World J Gastroenterol. 2025 Jun 7;31(21):105895. doi: 10.3748/wjg.v31.i21.105895. World J Gastroenterol. 2025. PMID: 40538512 Free PMC article.
-
Use of platelet transfusions prior to lumbar punctures or epidural anaesthesia for the prevention of complications in people with thrombocytopenia.Cochrane Database Syst Rev. 2018 Apr 30;4(4):CD011980. doi: 10.1002/14651858.CD011980.pub3. Cochrane Database Syst Rev. 2018. PMID: 29709077 Free PMC article.
-
CT-Based Machine Learning Radiomics Analysis to Diagnose Dysthyroid Optic Neuropathy.Semin Ophthalmol. 2025 Jul;40(5):419-425. doi: 10.1080/08820538.2025.2463948. Epub 2025 Feb 19. Semin Ophthalmol. 2025. PMID: 39968895
-
Dual-energy CT Radiomics Combined with Quantitative Parameters for Differentiating Lung Adenocarcinoma From Squamous Cell Carcinoma: A Dual-center Study.Acad Radiol. 2025 Mar;32(3):1675-1684. doi: 10.1016/j.acra.2024.09.024. Epub 2024 Sep 25. Acad Radiol. 2025. PMID: 39327138
-
Coblation versus other surgical techniques for tonsillectomy.Cochrane Database Syst Rev. 2017 Aug 22;8(8):CD004619. doi: 10.1002/14651858.CD004619.pub3. Cochrane Database Syst Rev. 2017. PMID: 28828761 Free PMC article.
References
-
- Luksanapruksa P, Buchowski JM, Tongsai S, Singhatanadgige W, Jennings JW. Systematic review and meta-analysis of effectiveness of preoperative embolization in surgery for metastatic spine disease. J Neurointerv Surg. 2018;10:596–601. 10.1136/neurintsurg-2017-013350. - PubMed
-
- Kumar N, Zaw AS, Khine HE, et al. Blood loss and transfusion requirements in metastatic spinal tumor surgery: evaluation of influencing factors. Ann Surg Oncol. 2016;23:2079–86. 10.1245/s10434-016-5092-8. - PubMed
-
- Mohme M, Mende KC, Pantel T, et al. Intraoperative blood loss in oncological spine surgery. Neurosurg Focus. 2021;50:E14. 10.3171/2021.2.Focus201117. - PubMed
-
- Pennington Z, Ehresman J, Feghali J, et al. A clinical calculator for predicting intraoperative blood loss and transfusion risk in spine tumor patients. Spine J. 2021;21:302–11. 10.1016/j.spinee.2020.09.011. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

